New Trials Bolster Dupilumab's “First Line Treatment†Potential for Atopic Dermatitis
Eric Simpson, MD, the lead author on the study, spoke to MD Magazine about the results, which showed great improvement with few side effects for those with moderate or severe atopic dermatitis.
Dupilumab, a drug currently under review by the FDA for approval, has shown signs of benefit for more than one serious, common medical condition. Along with the promise it may hold for the treatment of asthma, it is also promoted to be a strong combatant against atopic dermatitis (AD). Results of two additional Phase 3 trials were announced this month and published in The New England Journal of Medicine.
Eric Simpson, the lead author of the report, seems sold on dupilumab’s impact on AD. “I was quite surprised in the earlier phase trials we performed on the drug,” he told MD Magazine. “It was not clear which chemical messengers were most important in this condition as there are so many abnormalities you can find in the skin of affected patients. After many years of trying by many companies, Regeneron and Sanofi found two very important mediators of the disease.”
The drug is a fully human monoclonal antibody, which targets the body’s interleukin (IL)-4 receptors to block signaling of IL-4 and IL-13. Both are type 2 cytokines believed to play a major role in the manifestation of allergic diseases.
The two trials were identical, randomized, and placebo-controlled, enrolling adult patients whose AD was rated 3 (moderate) or 4 (severe) on the Investigator’s Global Assessment (IGA; 0-4 scale). SOLO 1 recruited 671 patients, and SOLO 2 contained 708. Results were consistent across the two groups, and encouraging in both cases. Each cohort was split into three groups: those who received dupilumab weekly, those who received it every other week, and those who received placebo.
After 16 weeks, the primary outcome of reducing the patient’s IGA condition rating from 3 or 4 down to 0 or 1 was met in 37% of the patients who received dupilumab biweekly and 38% who received it weekly in SOLO1, with those numbers coming in at 36% for both groups in SOLO2. In comparison, placebo patients who met that significant outcome were 10% and 8%, respectively. Across the two trials, a significantly greater portion of those who received dupilumab saw a reduction in Eczema Area and Severity Index (EASI) by 75% after 16 weeks than those who received placebo.
Reported side effects were minimal, namely nasopharyngitis and headache in a minority of patients. “Nasopharyngitis is a common side effect in general, it can be a common cold, likely not caused by the drug as it was present at the same rate with Placebo,” Dr. Simpson says, “Headache may be slightly more present in dupilumab arms, but not uncommon for injectable medications.” Among the 920 dupilumab patients in the two trials, only 6 discontinued the trial due to adverse events, a ratio almost identically consistent compared to 3 out of the 456 placebo patients who discontinued.
Simpson reported “no real differences in side effects or effects” between weekly and biweekly dosing, saying that “It is possible in clinical practice that some patients may benefit from weekly dosing, but that remains to be seen.”
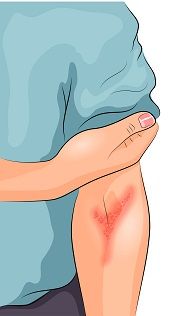
Atopic dermatitis is both extremely common and its impacts are often far from just skin deep. The intense itching can cause sleep loss and the visible lesions can spur declines in self-esteem, contributing to depression. Simpson has long been interested in the impact chronic skin diseases can have on the lives of children and adults, especially those with atopic dermatitis. “There is no better feeling,” he says, “than clearing up misunderstandings for the patients, as this disease is especially prone to misinformation, starting a treatment plan, and seeing their lives change for the better.”
Though still seeking approval and, as the study acknowledges, lacking in longer-term studies of its efficacy and safety, it’s hard to deny the positivity many in the field feel about dupilumab’s potential. In an expert opinion from 2015, a researcher wrote that “dupilumab has the potential to become a new first line standard treatment for patients with severe AD.” When asked if he agreed with that sentiment, Simpson was affirmative.
“I do, primarily in any patients who have failed adequate courses of topical therapy. There are no approved therapies for AD in the United States, outside of oral corticosteroids, a treatment discouraged by all treatment guidelines across the globe. There will be cheaper options to treat atopic dermatitis systemically, but they do not show the same level of effectiveness and are limited by significant side effects.”
Related Coverage:
Drug Trial Shows Improved Quality of Life with Atopic Dermatitis Treatment