- Revenue Cycle Management
- COVID-19
- Reimbursement
- Diabetes Awareness Month
- Risk Management
- Patient Retention
- Staffing
- Medical Economics® 100th Anniversary
- Coding and documentation
- Business of Endocrinology
- Telehealth
- Physicians Financial News
- Cybersecurity
- Cardiovascular Clinical Consult
- Locum Tenens, brought to you by LocumLife®
- Weight Management
- Business of Women's Health
- Practice Efficiency
- Finance and Wealth
- EHRs
- Remote Patient Monitoring
- Sponsored Webinars
- Medical Technology
- Billing and collections
- Acute Pain Management
- Exclusive Content
- Value-based Care
- Business of Pediatrics
- Concierge Medicine 2.0 by Castle Connolly Private Health Partners
- Practice Growth
- Concierge Medicine
- Business of Cardiology
- Implementing the Topcon Ocular Telehealth Platform
- Malpractice
- Influenza
- Sexual Health
- Chronic Conditions
- Technology
- Legal and Policy
- Money
- Opinion
- Vaccines
- Practice Management
- Patient Relations
- Careers
Physicians Could Save Billions with Electronic Transactions
Simply shifting from manual to electronic transactions for just 6 processes could save physicians and other healthcare providers billions of dollars.

Simply shifting from manual to electronic transactions for just 6 processes could save physicians and other healthcare providers billions of dollars, according to a recent report.
The 2013 US Healthcare Efficiency Index Report on Electronic Administrative Transaction Adoption and Savings from the Coalition for Affordable Quality Healthcare (CAQH) identified 6 key administrative transactions where providers could save money: claim submission; eligibility and benefit verification; prior authorization and referral certification; claim status inquiries; claim payment; claim remittance advice and receiving and posting payments.
“Administrative costs are part of doing business,” according to the report. “But in healthcare, there is a general consensus that the costs of basic business transactions — such as claims and billing, and benefit verification and authorizations — remain too high. While some administrative costs are inescapable, many routine processes can be automated, saving time and money for healthcare providers and insurers.”
According to the results of the report, more than 40% of claim payments are made by paper checks. Claim remittance advice and posting and receiving of payments had the lowest level of adoption (53%). However, claim submission had the highest rate of adoption (91%).
Organizations could potentially save $13 per transaction by migrating prior authorization and referral certification to electronic transaction. Similarly, electronic eligibility and benefit verification could save health plans and providers $3 per transaction.
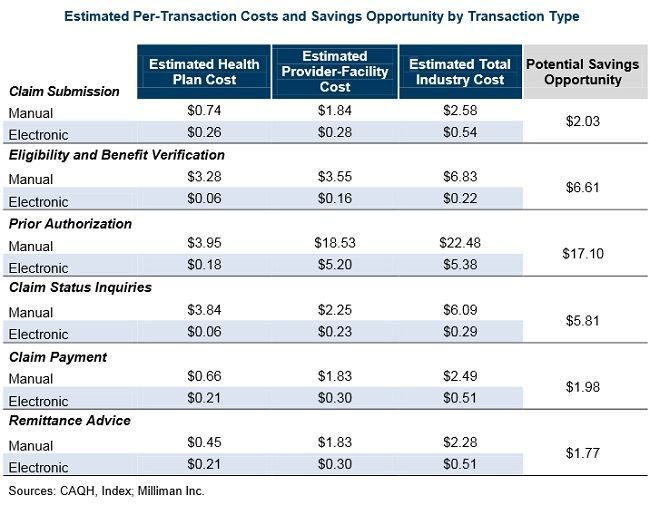
CAQH estimates that by switching to electronic transactions health plans could potentially save $460 million annually on eligibility verification; $410 million from prior authorization processes; $280 million from claim status inquiries; and $280 million from claim submission, claim payment, and remittance advice/payment posting transactions.
Meanwhile providers and facilities could save more than $3.5 million from eligibility verification processes and $1.5 billion for prior authorization transactions. The remaining processes combine to potentially save $1.7 billion.
“Early adopters of electronic transactions know from firsthand experience that cost savings and operational efficiencies are meaningful and real,” according to the report.
