Surgical Treatment of Acute Compartment Syndrome
Acute compartment syndrome is a surgical emergency of increased pressure within one of the body's muscle- and nerve-containing compartments, usually in the leg or arm. It occurs when accumulation of necrotic debris and hemorrhage (especially after fracture) increases intra-compartmental pressure, and that pressure exceeds the interstitium's capillary perfusion pressure.
Acute compartment syndrome (ACS) is a surgical emergency of increased pressure within one of the body's muscle- and nerve-containing compartments, usually in the leg or arm. It occurs when accumulation of necrotic debris and hemorrhage (especially after fracture) increases intra-compartmental pressure, and that pressure exceeds the interstitium’s capillary perfusion pressure. The March 2015 issue of Muscles, Ligaments and Tendons Journal offers a review of this traumatic orthopedic emergency.
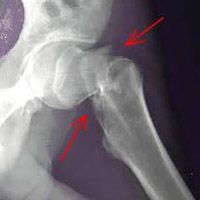
Remarkably painful, ACS occurs in closed osteofascial compartments and impairs local circulation. As noted above, it usually occurs in the leg, but the arms, hands, feet, and buttocks have also been affected. The precipitating cause is a severe fractures or crush injury in up to 75% of cases; rarely, minor injuries can trigger acute compartment syndrome, as can iatrogenic causes.
Currently, surgeons use physical examination and repeated ICP measures to diagnose ACS. ICPs that exceed 30 mm Hg of diastolic blood pressure are significant indicators of compartment syndrome. Fasciotomy is used to release compartmental pressure. ACS is a surgical emergency, as delaying fasciotomy increases the likelihood of irreversible ischemic damage to muscles and peripheral nerves.
Some surgeons believe that open fractures naturally decompress, and the authors warn against this erroneous idea. In addition, about one-quarter of cases have comorbid rhabdomyolysis that needs to be managed.
This review covers some of ACS’s uncommon causes, heightening surgeons’ awareness of many possible etiologies and the potential for serious complications. They note that even expert surgeons may have trouble diagnosing ACS when the cause is atypical—isolated vascular injury without fracture, superior gluteal artery injury, and femoral vessel injury in the absence of fracture. They note that anticoagulants can cause ACS and patients with hemophilia are at elevated risk.
The authors acknowledge the lack of consensus concerning diagnosis and treatment of ACS, and the most controversy surrounds the ICP at which fasciotomy is absolutely indicated and the timing of wound closure. Reliable diagnostic methods are sorely needed.