A Year in Review: All About Fibromyalgia
Between daily news and conferences around the country, it was a busy year in fibromyalgia research.

Fibromyalgia continues to puzzle physicians. Its cause is unknown and there are only three drugs approved by the US Food and Drug Administration (FDA) to treat it. For reasons unknown, fibromyalgia impacts females and males in a 7:1 ratio, according to the centers for Disease Control and Prevention. Despite the challenges, researchers continue to examine where it stems from and how to make patients’ lives better.
There was a substantial amount of fibromyalgia research conducted in 2016. In addition to that, the editors at MD Magazine attended conferences that highlighted the topic, including:
- PAINWeek 2016 in Las Vegas, Nevada
- 2016 American College of Rheumatology/Association of Rheumatology Health Professionals Annual Meeting (ACR 2016) in Washington, District of Columbia
Read on to catch up on the key fibromyalgia findings over the past year, and stay up-to-date with the MD Magazine fibromyalgia condition center. Don’t forget to connect with us on Facebook, Twitter, Instagram, and LinkedIn!

Without a blood test or specific biomarker, diagnosing fibromyalgia can be a challenge. The Fibromyalgia Rapid Screening Tool (FiRST) can help physicians make the determination, but just how reliable is it?
The standard for diagnosing fibromyalgia is using the ACR 90 criteria along with a rheumatologist’s opinion. French researchers from Centre Hospitalier Universitaire (CHU) Gabriel-Montpied compared the efficacy of the FiRST against the standard method when it comes to detecting fibromyalgia in association with inflammatory rheumatic diseases.
>>> Continue reading this story here
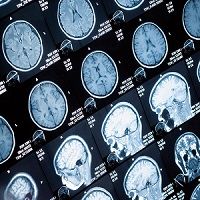
Fibromyalgia is notoriously difficult to diagnose. There is no specific blood test or biomarker that physicians can go off of, but instead the condition is characterized by chronic widespread musculoskeletal pain, along with fatigue and mood disorders. However, some healthcare providers still don’t think that fibromyalgia is a “real” condition. But a new study from the University of Colorado Boulder (CU Boulder) may have found a brain signature that red flags the disease.
“The novelty of this study is that it provides potential neuroimaging-based tools that can be used with new patients to inform about the degree of certain neural pathology underlying their pain symptoms,” lead author Marina López-Solà, PhD, a post-doctoral researcher in CU Boulder’s Cognitive and Affective Control Laboratory, said in a news release.
>>> Continue reading this story here

Many patients with a variety of chronic pain conditions think negatively about how it will affect their sleep — which ends up leading to worse sleep outcomes. A study from the University of Warwick in England shows just how powerful these negative thoughts are.
“Current psychological treatments for chronic pain have mostly focused on pain management and a lesser emphasis on sleep, but there is a recent interest in developing therapies to tackle both pain and sleep problems simultaneously,” Esther Afolalu, a PhD researcher at the University of Warwick, said in a news release.
Researchers from the Sleep and Pain Lab in the Department of Psychology at the school created the Pain-Related Beliefs and Attitudes about Sleep (PBAS) scale to measure how pain and sleep beliefs impact one another. The 10-item scale is the first of its kind to explore the correlation between the two factors.
>>> Continue reading this story here
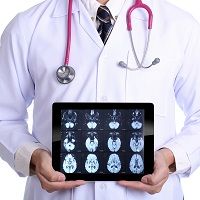
The first study to investigate the link between fibromyalgia and stroke risk revealed telling results across all ages and sexes.
Fibromyalgia is a chronic pain and fatigue condition that is more common in women than men. Although people are typically diagnosed at middle age, symptoms often begin earlier. The condition has been linked to sleep problems and depressive symptoms; now, researchers from the China Medical University Hospital found that these patients are more likely to suffer from stroke.
>>> Continue reading this story here

Fibromyalgia and sexual dysfunction are both conditions that affect more women than men; and now it looks like those who have the former are more likely to have the latter — especially if they have depression or anxiety.
While many studies have examined the association between fibromyalgia and sexual dysfunction, this is the first one to evaluate the two in connection with mood, anxiety, and personality disorders. Researchers from several institutions in Turkey found strong correlations between the conditions, as described in Dove Medical Press.
>>> Continue reading this story here

Pain medications can often cause side effects such as dizziness and sleepiness; but little do pregnant women know that they could be at risk for birth defects when taking pregabalin.
In addition to pain, the US Food and Drug Administration (FDA) approved pregabalin, branded as Lyrica, for adults with fibromyalgia, post-shingles pain, and diabetic or non-diabetic-related neuropathic pain. It can also be prescribed to treat epilepsy, anxiety, and other brain disorders. The medication’s label points out potential side effects, like allergic reactions, suicidal thoughts, and swelling limbs, but a new study published in Neurology indicates another serious potential outcome.
>>> Continue reading this story here

While previous evidence has shown pregabalin (Lyrica/Pfizer) to be effective in assuaging pain among adults with fibromyalgia, there are no approved treatments for its symptoms in adolescence.
Pfizer funded a study regarding the efficacy of Lyrica among those aged 12 to 17 in hopes of eventually changing that. Unfortunately, no primary returns showed statistically significant improvement, though there was some silver lining in secondary metrics.
>>> Continue reading this story here

Fibromyalgia, the vexing rheumatic condition that causes widespread pain and tenderness in as much as 4% of the population, still has neither a clear cause nor a consensus treatment. In a wide-ranging new review of studies on fibromyalgia treatments, the European League Against Rheumatism (EULAR) evaluated over two dozen pharmacological and non-pharmacological treatment methods and found only one, exercise, to be successful enough to warrant a unanimous “strong for” recommendation.
The organization’s original recommendations, released in 2005, predated much of the evidence discussed in this new document, relying primarily on expert opinion. In the decade that has passed, a wealth of individual trials have emerged, providing the basis for these new recommendations.
>>> Continue reading this story here
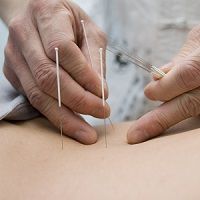
The benefits of acupuncture for fibromyalgia pain remain inconclusive despite extended research. However, a new study may have found the factor that separates successes from failure.
It was just recently that a study conducted in Brazil concluded that acupuncture does not reduce pain in women with fibromyalgia. However, like many other studies, this one looked at the effects of standard acupuncture treatment. A new analysis by researchers in Spain found that the therapy does alleviate pain — when it’s individualized for each patient.
>>> Continue reading this story here
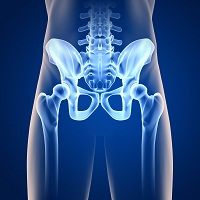
When more and more women with fibromyalgia began seeking care for pelvic pain syndromes, researchers from Oregon Health & Science University set out to examine the connection in a larger group of patients.
Fibromyalgia causes widespread pain, fatigue, and even psychological problems. The chronic condition is more prevalent in females than males and typically targets middle-aged adults. Comorbidities in these patients, such as headache, sleep problems, and other pain syndromes, are not uncommon. Recent research found that pelvic floor and urinary distress is also prevalent in women with fibromyalgia.