A Year in Review: All About HIV/AIDS
Between daily news and conferences around the country, it was a busy year in HIV/AIDS research.

Progress in human immunodeficiency virus (HIV) awareness, diagnostics, and treatments have come a long way since the virus was first discovered in 1983. With the right treatment, HIV never has to move on to acquired immunodeficiency syndrome (AIDS).
From former NBA star, Magic Johnson, celebrating life 25 years after his diagnosis to further developments how the virus operates, there hasn’t been a lack in HIV/AIDS news this year.
The MD Magazine editors also attended conferences focused in this area of medicine, including:
- 20th Annual United States Conference on AIDS (USCA 2016) in Hollywood, Florida
- Infectious Disease Week (IDWeek 2016) in New Orleans, Louisiana
Read on to catch up on the key HIV/AIDS findings over the past year, and stay up-to-date with the MD Magazine HIV/AIDS condition center. Don’t forget to connect with us on Facebook, Twitter, Instagram, and LinkedIn!

It’s been known that people with the human immunodeficiency virus (HIV) have a substantially higher risk of getting certain kinds of cancer, including anal, liver, and lung, as well as Hodgkin lymphoma, according to the National Cancer Institute. As of November 3, HIV is officially considered a carcinogen.
With the addition of five viruses and two compounds, the US Department of Health and Human Services (HHS) 14th Report on Carcinogens is now up to 248.
>>> Continue reading this story

“November 7, 1991 was a life changing day that I never saw coming,” Earvin “Magic” Johnson wrote on his site, The Playbook.
That was the day that Johnson was diagnosed with the human immunodeficiency virus (HIV). Although the acronym still carries a heavy burden, it held even more weight 25 years ago.
Back then it was considered to be a death sentence and a disease called “gay cancer.” Many early diagnoses were traced back to blood transfusions, especially in babies. But Johnson was one of the first straight public figures to come out with the diagnosis — and at the time, he had only been married to his wife, Cookie, for 45 days.
>>> Continue reading this story here
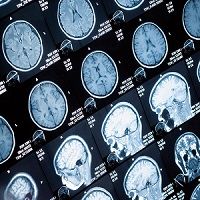
It was back in April that researchers from Georgetown University reported the first case of Alzheimer’s disease in a person living with the human immunodeficiency virus (HIV). Now the case report will be presented at the Alzheimer’s Association International Conference (AAIC) 2016 in Toronto, Canada on July 27.
“This patient may be a sentinel case that disputes what we thought we knew about dementia in HIV-positive individuals,” R. Scott Turner, MD, PhD, a neurologist at Georgetown University Medical Center (GUMC), said in a news release.
Turner had diagnosed the HIV-positive 71-year-old man with Alzheimer’s after a PET scan showed deposition of amyloid in the brain. Since HIV causes inflammation in the brain, and may prevent amyloid clumps from forming, it was believed that people with the condition may not develop Alzheimer’s.
>>> Continue reading this story

Baby Boomers face unique risks when it comes to the human immunodeficiency virus (HIV) infection—ones due more to attitudes and behavior than medical issues.
Older people are more likely than younger people to be diagnosed with HIV late in the course of infection. That means they start treatment later and likely incur more damage to their immune systems, putting them at greater risk of death.
>>> Continue reading this story

Researchers say a billion-dollar US government program that used abstinence-only education to fight the spread of human immunodeficiency virus (HIV) succeeded in one sense: It proved abstinence-focused programs don’t work.
Former President George W. Bush announced the US President’s Emergency Fund for AIDS Relief (PEPFAR) in 2003 and it launched the following year. The goal was to reduce the risk of HIV through education, specifically with programs focusing on abstinence, marital fidelity, and limiting the amount of sexual partners. But even a hefty price tag couldn’t spell success for certain messages, as described in Health Affairs.
>>> Continue reading this story

Previous studies have shown that as the human immunodeficiency virus (HIV) develops, the virus does not target macrophages. However, new research conducted in mouse models show evidence that indicate that may not be the case.
Jenna Bone Honeycutt, PhD, from the University of North Carolina (UNC) discussed the new HIV research with MD Magazine. Honeycutt and colleagues looked at the virus in relation with macrophages and found results that contradict previous beliefs. It was thought that macrophages become infected by absorbing T-cells in the body, but the UNC research involved animal models that were devoid of T-cells.
>>> Continue reading this story

Pre-exposure prophylaxis (PrEP), a daily human immunodeficiency virus (HIV) prevention pill, became a game-changer when it was approved by the US Food and Drug Administration (FDA) in 2012. If physicians and patients follow prescription guidelines, it’s predicted to cut new HIV infections by one-third within 10 years.
Branded under the name Truvada, PrEP is a combination of tenofovir disoproxil fumarate and emtricitabine. Studies have shown that the drug can prevent more than 90% of HIV cases if used consistently; however, only about 5% of men who have sex with men (MSM) are actually using PrEP now. In 2014, officials from the Centers for Disease Control and Prevention (CDC) released guidelines on using PrEP in clinical practice. Now researchers from Emory University, the CDC, and the University of Washington analyzed the impact the drug could make in a decade.
>>> Continue reading this story
Although men who have sex with men make up the majority of cases of existing and new human immunodeficiency virus (HIV) infections, heterosexual partners are still at risk. Studies have long determined that a woman is more likely to contract HIV from a man than vice versa, so finding an effective prevention method is crucial for high-risk women.
The National Institute of Allergy and Infectious Diseases (NIAID), part of the National Institutes of Health (NIH), funded a phase 3 trial in order to assess an experimental vaginal ring for HIV prevention. The study, known as ASPIRE or MTN-020, was presented at the HIV Research for Prevention (HIVR4P) meeting in Chicago, Illinois.
>>> Continue reading this story

Investigators from Columbia University and the US Centers for Disease Control and Prevention (CDC) went from house-to-house earlier this year to collect information on the human immunodeficiency virus (HIV) in three countries in Africa.
Surveys of more than 80,000 adults and children in Zimbabwe, Malawi, and Zambia indicate a sharp decline in the incidence of HIV infection, a sharp increase in the treatment of diagnosed cases and a plateau in the prevalence of the disease.
>>> Continue reading this story
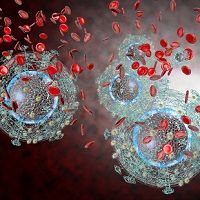
At the 20th United States Conference on AIDS, Carlos Rodriguez Diaz, PhD, University of Puerto Rico, explained that the vast majority of his work focuses on exploring the various social inequities present in the grand scheme of the HIV/AIDS movement: poverty, unemployment, education, and access to healthcare. Diaz believed these social inequities are major structural factors that influences the ability that people might have to stay healthy.
>>> Continue reading this story here
The human immunodeficiency virus (HIV) is no longer the death sentence it was when the virus was first discovered in 1983. Although patients are living better, longer lives, finding a cure to the disease remains a top priority.
Researchers at the University of North Carolina (UNC) are actively on the hunt for an HIV cure and, for the first time, they identified how antiretroviral therapy (ART) affects the infection in the female reproductive tract. MD Magazine spoke with Angela Wahl, PhD, an assistant professor of infectious diseases at UNC, to dive deeper into the clinical implications and what this means for a condition that affects nearly 35 million people worldwide.