An Assessment of an EHR-Assisted Tobacco Treatment Model for GI Patients: Takeaways from ELEVATE
How an outpatient-based smoking cessation model may come to aid other health systems' gastroenterology patients.
Suha Abushamma, MD

Smoking is the most preventable health hazard in the US, responsible for over 480,000 deaths annually. About 19% of US adults reported current use of a commercial tobacco product in 2020, of which cigarette smoking was the most prevalent.
From a gastroenterology (GI) perspective, smoking is a risk factor for esophageal, pancreatic and colon cancer, and adversely affects peptic ulcer disease, pancreatitis and Crohn’s disease. Smoking cessation is strongly encouraged by the American College of Gastroenterology (ACG) guideline for Managing Crohn’s Disease in Adults. Despite key recommendations for the management of smoking in healthcare settings, the degree to which this is implemented in GI clinics is unknown.
In our study that was presented at the recent Digestive Disease Week (DDW) 2023 Annual Meeting’s GI Fellow-Directed Quality Improvement Projects session—and which won an American Gastroenterological Association (AGA) Fellow Abstract Award—we aimed to assess our providers’ practices regarding smoking cessation, identify perceived barriers for administering smoking cessation treatments, and address these barriers by implementing a novel Electronic Health Record (EHR)-assisted tobacco treatment model (ELEVATE) in our GI clinics.
Fig. 1, EHR-Enabled Evidence-Based Cessation Treatment (ELEVATE) Patient Care Workflow using 5A’s.
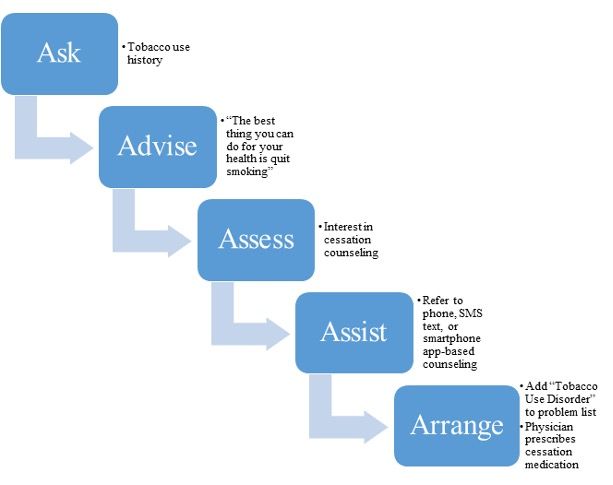
ELEVATE is implemented by the medical assistant during the patient rooming process, and utilizes the “5 A’s” recommended by the US Public Health Service Clinical Practice Guideline Panel, as illustrated in Fig. 1.
A rate of 91% of GI physicians responded to our survey, and nearly half of them stated they always asked patients if they smoked. Although 75% of physicians stated they would assess their patients’ willingness to quit at the time of the visit, less than half consistently advised smokers to quit, and only 20% often assisted patients who smoke with counseling.
Fig. 2, Post-ELEVATE module training tobacco treatment effectiveness.

Lack of a systematic program to offer help to patients was reported by 80% of providers as an extremely/very important barrier limiting their smoking cessation practices. ELEVATE module training was implemented at the beginning of 2021 using Epic Systems EHR. The proportion of smokers receiving cessation treatment increased from pre-ELEVATE to post-ELEVATE (14.36% to 27.47%; RR, 1.90; 95% CI, 1.60 - 2.26, P <.001). Post-ELEVATE, 14.4% (n = 38) of patients with treatment quit smoking, compared to 7.9% (n = 55) of patients without treatment (RR, 1.89; 95% CI 1.26 – 2.82, P = .0021), as depicted in Fig. 2.
This study sheds light on an often under-recognized source of morbidity in our GI patients and identifies an efficient and scalable strategy to combat tobacco use and improve clinical outcomes in our patients. ELEVATE smoking module has been selected by Epic Systems for wide dissemination to other healthcare systems.