Complex Regional Pain Syndrome: A Guide for Recognition and Treatment
Like so many inflammatory conditions, complex regional pain syndrome (yes, there's growing evidence it's inflammatory) demands early treatment. Yet it is devilishly difficult to recognize its initial stages. Here are the signs, and an algorithm for management.
Complex regional pain syndrome (CRPS) is a difficult and vexing condition that arises at least in part after some 30% of fractures, and may also occur after orthopedic surgery. Recent evidence suggests that inflammatory processes and a pattern of disuse may be more important than previously thought.
At the recent American Academy of Orthopedic Surgeons conference, Nicolai Baecher MD and his colleagues Thomas Sanders MD and Michael Kessler MD presented a new algorithm for management of CRPS. Here we present the details in brief, and Dr. Baecher’s responses to some questions addressed to the interests of rheumatologists.
Dr. Kessler is an assistant professor and Dr. Baecher is a resident in the Department of Orthopaedic Surgery at Medstar Georgetown University Hospital. Dr. Sanders is an orthopaedic surgeon at Inova-Fairfax Hospital in Falls Church VA.
Stages of CRPS:
I. Radiographs are normal, and symptoms arise that are subjective in nature: pain, hyperesthesia, increased sweating, and cold-heat intolerance.
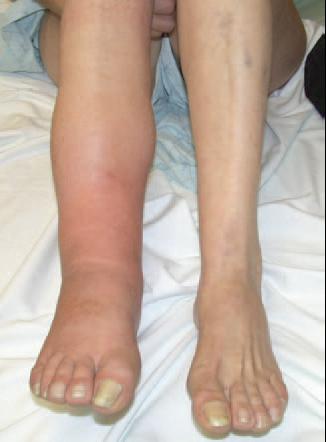
II. Around months 3 to 6, symptoms are marked by edema, cold glossy skin, loss of motion, and hair loss. Osteopenia begins to appear on x-rays.
III. Muscles and skin begin to atrophy. Other symptoms are hair loss, brittle nails, severe contracture, and advanced demineralization on x-ray.
Early diagnosis and aggressive treatment are important. The hallmarks of management are:
Prevention: Patients at high risk or with a history of CRPS should begin taking oral vitamin C for prophylaxis at the time of injury or surgery.
Stage I: The task is to break the cycle of disuse and desensitize the limb early in the disease process. Begin aggressive physical therapy before contractures develop. Oral corticosteroids or NSAIDs may help if inflammation is involved.
Stage II: Patients may benefit from added bisphosphonate and continued physical therapy. Stellate ganglion blockade may be warranted in more intractable cases where other modalities have failed.
Stage III: Patients with trophic changes and contractures are very difficult to treat. Surgery may be required to restore function, although it should be approached warily as it may reinitiate the disease process.
Q. Is there dispute in the field about whether CRPS actually exists (as there was with fibromyalgia for so long)?
The diagnosis and recognition of CRPS is certainly a difficult and debated issue. I think it is safe to say that, much like many other syndromes that are largely subjective in nature (and with little objective testing available to help establish a diagnosis), its existence is controversial. Much like any other syndrome that has no diagnostic test and must be established by concordance with a predefined list of symptoms, it can be unsatisfying to a practitioner who is more at home with deductive and physically discoverable etiologies.
I have certainly met some surgeons who feel skeptical about its existence as a real disorder. However most clinicians, if they are honest with themselves, will admit to having patients towards whom they cannot offer a routine or anatomic explanation of their symptoms. It is in these patients that a diagnosis of CRPS should be reasonably considered.
Q. Can you say a bit more about how to recognize the earliest symptoms?
As to the details one should focus on in the clinic, the first sign to watch for is a postoperative or post-injury course that is atypical. It is tempting to dismiss a slow recovery or atypical pain as simply being on the tail end of the bell curve. At the same time, these are the same patients in whom the diagnosis is most important to be made, because the earlier intervention can be started, hopefully the better the outcome.
Clinicians should be aware of disproportionate pain, of symptoms that are not confined to a specific nerve distribution, hyperesthesia, trophic changes, and restricted motion. The art of medicine is important, as the more common causes of any of these symptoms need to be ruled-out.
Unfortunately many of the diagnostic studies appear later in the course of the disease. You may see periarticular osteopenia, which is common in simple disuse as well and is particularly common in the orthopaedic setting with casting. Although bone scans may show a characteristic uptake pattern, in this day of practicing more cost-conscious medicine, that probably is not a worthwhile study to pursue.
Q. What dosage of vitamin C do you recommend for prophylaxis in patients with a history of CRPS?
Luckily, the early interventions carry little morbidity with them. Both vitamin C and physical therapy are well tolerated and are evidence-based early interventions. Vitamin C may be given as 500 mg PO BID for 4 to 6 weeks. It is probably best to start vitamin C therapy as early as possible. In patients in whom a history of CRPS is documented, vitamin C therapy ought to be started at the time of injury or surgery. Although some have criticized the efficacy of vitamin C, it is our opinion that given its safety profile, it is worth trying. Similarly physical therapy should be focused on as much motion as is tolerable given the injury or surgery, as well as modalities to break the hyperesthetic loop.
Q. How did you derive the treatment algorithm?
By necessity, the algorithm is a combination of clinical evidence and personal thought and practice. The interventions we have recommended at various stages of CRPS have been selected based on the evidence available for the efficacy, balanced with both their potential side effects and safety profile.
Hence, vitamin C and physical therapy, which have some good data for their use but also a known safety profile, can be recommended early and with little hesitancy for all patients. A later intervention we recommended, bisphosphonate therapy, needs to be balanced with the risks involved with its use, namely osteonecrosis and pathological fracture.
In later stages, a psychiatric consult may be warranted to help with multimodal treatment and to act as adjuvant therapy. However, this may be burdensome and patients with less severe sympmtoms may perceive it as "labeling." Hence we do not recommend it early, nor for all patients.
References:
REFERENCES:
1. Galer BS, Bruehl S, Harden RN.
IASP Diagnostic criteria for complex regional pain syndrome: a preliminary empirical validation study. International Association for the Study of Pain. Clin J Pain (1998) 14:48-54.2. Harden RN, Bruehl S, Galer BS, et al. Complex regional pain syndrome: are the IASP diagnostic criteria valid and sufficiently comprehensive?
Pain
(1999) 83:211-219.
3. Nelson DV, Novy DM.
Psychological characteristics of reflex sympathetic dystrophy versus myofascial pain syndromes.
Reg Anesth
(1996) 21:202-208.
4. Woolf CJ, Mannion RJ.
Neuropathic pain: aetilology, symptoms, mechanism, and management.
Lancet
(1999) 353:1959-1964.
5. Zollinger PE, Tuinebreijer WE, Breederveld RS,
et al.
Can vitamin C prevent complex regional pain syndrome in patients with wrist fractures? A randomized, controlled, multicenter dose-response study.
JBJS Am
(2007) 89A:1424-1431.
6. Kozin F, McCarty DJ, Sims J, and Genant H.
The reflex sympathetic dystrophy syndrome: I. Clinical and histologic studies: Evidence of bilaterality, response to corticosteroids and articular involvement.
Am J Med
(1976) 60:321-331.
7. Jadad AR, Carroll D, Glynn CJ.
Intravenous regional sympathetic blockade for pain relief in reflex sympathetic dystrophy: a systematic review and a randomized, double-blind crossover study.
J Pain and Symptom Mgmt
(1995) 10:13-20.
8. Eckmann MS, Ramamurthy S, Griffin JG.
Intravenous regional ketorolac and lidocaine in the treatment of complex regional pain syndrome of the lower extremity: a randomized double-blinded, crossover study.
Clin J Pain
(2011) 27:203-206.
9. Ritz BW, Alexander GM, Nogusa S
et al.
Elevated blood levels of inflammatory monocytes (CD14+ CD 16+) in patients with complex regional pain syndrome.
Clin Exp Immunol
2011;164:108-117.
9. Kramer HH, Eberle T, Uceyler N,
et al.
TNF-alpha in CRPS and ‘normal’ trauma â significant differences between tissue and serum.
Pain
(2011) 152:285-290.
10. Van Eijs F, Stanton-Hicks M, Van Zundert J,
et al.
Evidence-based interventional pain medicine according to clinical diagnoses. 16. Complex regional pain syndrome.
Pain Pract
(2011) 11:70-87
11. Kalita J, Vajpayee A, Misra UK.
Comparison of prednisolone with piroxicam in complex regional pain syndrome following stroke: a randomized controlled trial.
QJM
(2006) 99: 89-95.
12. Tran DQH, Duong S, Bertini P, Finlayson RJ.
Treatment of complex regional pain syndrome: a review of the evidence.
Can J Anaesth
(2010) 57(2):149-166.
13. Adami S, Fossaluzza V, Gatti D, Fracassi E, Braga V.
Bisphosphonate therapy of reflex sympathetic dystrophy syndrome.
Ann Rheum Dis
(1997) 56: 201-204.
14. Varenna M, Zucchi F, Ghiringhelli D,
et al.
Intravenous clodronate in the treatment of reflex sympathetic dystrophy syndrome. A randomized, double blind, placebo controlled study.
J Rheumatol
(2000) 27: 1477-1483.
15. Chelimsky TC, Low PA, Naessens JM
et al
.
Value of autonomic testing in reflex sympathetic dystrophy.
Mayo Clin Proc
(1995) 70:1029-1040.
16. van de Vusse AC, Stomp-van den Berg SG, Kessels AH, Weber WE
et al
.
Randomised controlled trial of gabapentin in complex regional pain syndrome type 1.
BMC Neurol
(2004) 4:13.
17. Kemler MA, Barendse GAM, Van Kleef M.
Spinal Cord stimulation in patients with chronic reflex sympathetic dystrophy.
NEJM
(2000) 343:618-624. (See also
Spinal cord stimulation for chronic reflex sympathetic dystrophy--five-year follow-up
18. Dielissen PW, Claassen AT, Veldman PH,
et al.
Amputation for reflex sympathetic dystrophy.
JBJS Br
(1995) 77B:270-273.
19. Van Eijs F, Stanton-Hicks M, van Zundert J
et al.
Evidence-based interventional pain medicine according to clinical diagnoses. 16. Complex regional pain syndrome.
Pain Pract
(2011) 11:70-87
20. Linson MA, Leffert R, Todd DP.
The treatment of upper extremity reflex sympathetic dystrophy with prolonged continuous stellate ganglion blockade.
J Hand Surg Am.
(1983) 8:153â159.
21. Cameron HU, Park YS, Krestow M.
Reflex sympathetic dystrophy following total knee replacement.
Contemp Orthop.
(1994) 29:279â281.