Cost of Insulin Pens Justified with Better Safety, Improved Health in Elderly Diabetics
Although pen devices are perceived to be more costly than vialed insulin, new study results indicate that elderly diabetic patients are more likely to accept pen devices and adhere to therapy, which decreases long-term complications and associated healthcare costs.
Nearly a quarter of American elderly patients have diabetes mellitus, which represents half of all diabetics. When those patients initially present with hemoglobin greater than 8.5 percent or unresponsiveness to metformin and lifestyle changes, the consensus algorithm of the American Diabetes Associations suggests that insulin is a reasonable treatment option.
As diabetic elders are highly likely to have vision loss, neuropathies, poor mobility, poor manual dexterity, and multiple comorbidities such as early dementia, they face specific challenges related to the self-administration of insulin. Consequently, those patients are at a high risk of life-threatening hypoglycemia compared to the general adult population.
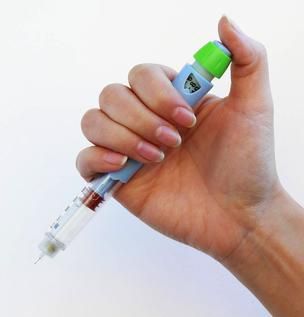
Self-injection can be difficult, but when it comes to insulin, it can also be dangerous. Fortunately, insulin pen devices have become safer alternatives to drawing insulin doses from vials for many geriatric patients. Insulin pens have greatly evolved since their market entry in the 1980s, and many types are available today. However, cost is still a concern, though most insurance plans — including Medicare Part D — charge the same amount for a month supply of insulin in pen devices as they do for vialed insulin.
To help prescribers understand each device's unique mix of characteristics, researchers from Auburn University in Alabama have assembled a review of available insulin pen devices, including reusable durable pens and disposable prefilled ones.
Acknowledging that vision loss is a ubiquitous concern among the elderly, the review authors described the conveniences of each product, such as audible clicks and large dosing windows. Where dexterity is a concern, the products’ size and overall ease of use may aid patients.
The authors also highlighted patient perceptions about insulin delivery and how negative perceptions — even if they are incorrect — impede patients’ readiness to accept the drug. Nevertheless, pen devices are accepted more often than the traditional vial and syringe.
In terms of limitations, some patients dislike having to leave the pen device in their subcutaneous tissues for 5 to 10 seconds after dose release, which isn’t necessary for traditional vialed insulin. Additionally, regular human insulin and NPH insulin are not available in pen form.
Although pen devices are often perceived to be more costly than vialed insulin, the study results indicated that elderly diabetic patients are more likely to accept pen devices and adhere to therapy, which leads to better glycemic control that decreases long-term complications and associated healthcare costs. The significantly improved safety profiles of pen devices also avert costly episodes of hypoglycemia.
Thus, the authors concluded that insulin pen devices are reasonable alternatives to traditional vial and syringe methods for elderly patients.