Does Cervical Spine Treatment Reduce Low Back Pain?
Roughly a third of patients with low back pain also have neck pain. This study assessed correcting cervical disk displacements to reduces lower body pain and numbness.
ABSTRACT: Although cervical spine pathology is not recognized as a cause of low back pain (LBP), roughly one-third of patients with LBP also have neck pain. Our study examined whether management of cervical disk displacements reduces the severity and frequency of lower body pain and numbness in patients with lumbar symptoms and cervical spine lesions. Lower body symptoms were recorded before and after a physical therapy program targeted at the cervical spine. There was an overall 44% reduction of lower body pain and numbness; 82% of complaints of severe pain and 74% of complaints described to be constant were no longer made after cervical treatments. Management of cervical lesions improved lower back and lower extremity pain and numbness. (J Musculoskel Med. 2011;28:333-338)
_____________________________________________________________________________________________
Cervical spine pathology is not recognized as a cause of low back pain (LBP), but about one-third of patients with LBP also have neck pain. We conducted a study to examine whether management of cervical disk displacements reduces the severity and frequency of lower body pain and numbness in patients who have lumbar symptoms and cervical spine lesions. In this article, we report our findings.
Background
LBP, which affects 60% to 80% of the adult US population, is the fifth most common reason for visiting a physician.1-3 Textbooks document that the causes of LBP often are very difficult to determine; for up to 85% of patients, no specific cause can be found.4,5 Few or no references suggest a cervical cause or cervical enhancement of low back and lower extremity symptoms. However, 35.4% of persons who reported having LBP also reported having neck pain in a study that analyzed data from the 2002 National Health Interview Survey.6
A pattern has become apparent in this clinical practice. Reassessment of patients who did not show anticipated improvements of lumbar symptoms after treatments focused on the lumbar spine often revealed abnormal upper extremity and upper motor neuron findings indicative of an overlying cervical lesion. Cervical MRI scans of these patients showed single- or multiple-level posterior cervical disk displacements that were indenting the thecal sac; in some of the cases, there was cervical cord contact or compression.
We propose that a portion of patients who present with persistent LBP and lower extremity symptoms are experiencing cervical spine–triggered lumbar symptoms. The anatomy of the cervical spine is such that 75% to 80% of posterior-directed cervical disk protrusions do not result in isolated cervical root compression or radiculopathy.1,7 They instead cause central compressive forces on the thecal sac, central canal, or cervical cord that result in cervical cord dysfunction or a mild myelopathy.
The patients are not aware of the resulting upper extremity dysfunction and do not complain of neck pain or upper extremity symptoms. However, physical examination reveals both upper and lower extremity weakness, hyperreflexia, and sensory alterations at and below the level of the cervical lesions.8,9
We think that the cervical lesion triggers the more bothersome lumbar and lower extremity symptoms, resulting in mild weakness and dysfunction at and below the cervical level, causing weakness, imbalance, and neural processing problems of crucial core and lumbar paraspinal muscles. The resulting torso dysfunction leads to lumbar segmental instability, dysfunction of the lumbar “3-joint complex,” and faster progression of the Kirkaldy-Willis degenerative cascade. The lumbar segmental instability and degenerative cascade then trigger low back and radicular leg symptoms.10,11
We hypothesize that in patients who have displaced cervical disks, physical therapy and nonsurgical decompression result in a reduction of lower body pain and numbness. Our study objective was to determine whether low back and lower extremity pain and numbness can be improved with management of the cervical spine.
Methodology
A total of 62 patients evaluated and treated at the office of a physician board-certified in physical medicine and rehabilitation and neuromuscular medicine were studied. The mean patient age was 60 ± 14.8 years. To participate, patients had to present with primary complaints of low back and lower extremity symptoms. On physical examination, the selected patients had abnormal cervical and upper extremity neurological findings that were indicative of an overlying cervical lesion.
FIGURE 1
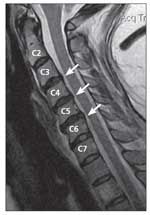
C3-4, C4-5, and C5-6 cervical disk protrusions are seen in this MRI scan (arrows). The radiologist described the C5-6 disk as a broad-based disk bulge with cord contact
For all patients, closed MRI scans above 1.5 tesla were obtained (Figures 1 and 2). Every patient's cervical MRI scan revealed single- or multiple-level posterior cervical disk displacements that were indenting the thecal sac. Patients had disks contacting the dural sac with and without abutment of the cervical cord. The MRI findings correlated with the abnormal upper and lower extremity neurological findings. Statements made throughout the study about cord contact, compression, and number of displaced disks were based on the MRI readings.
For patients to qualify, their workup could not reveal other significant medical conditions that would contribute to the symptoms of concern. The patient had to consent to treatment and study, be compliant with treatment, and complete the therapy as recommended by the physician. This was a sample of convenience gathered from December 2008 to December 2009. This study was conducted without any institutional affiliations and therefore did not use an ethics review board. However, all procedures were in accordance with the Declaration of the World Medical Association.
FIGURE 2
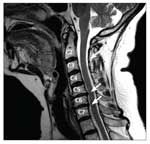
Cervical disk displacements are seen at C5-6 and C6-7 (arrows). The C5-6 disk displacement was described by the radiologist as a broad-based mixed spondylotic protrusion eccentric to the right, indenting the thecal sac and resulting in mild ventral cord flattening and mild central canal stenosis, and moderate right and severe left foraminal narrowing.
Patients' relevant past medical histories were gathered, including all past lumbar treatments and any current neuropathies that could be contributing to lumbar symptoms. Fifty-one of the 62 patients had already received conservative treatment for lumbar symptoms, including rest, NSAIDs, analgesics, heat and ice, traditional physical therapy, and chiropractic treatments. However, alleviation of symptoms achieved with past treatments to the lumbar spine was little or nonexistent. All patients discontinued other treatments on admittance to this study.
Treatment included traction. Applied traction reduces irritation and improves circulation by decreasing pressure between intervertebral disks, facets, and posterior structures.12 Traction also halts progression of the Kirkaldy-Willis degenerative cascade by reducing the degenerative forces on the 3-joint complex.4
Intermittent computer-generated cervical traction was delivered while the patient was supine using an Accu-SPINA Intervertebral Disc Decompression therapy device. The traction pull was progressed gradually by 0 to 3 lb each treatment session, and the treatment angle was adjusted as needed for optimal patient improvements.
Patients initially received physical therapy 3 to 5 times a week, with gradual tapering over a 5- to 12-week period as symptoms improved or plateaued. Nonsurgical decompression was combined with interferential stimulation, ultrasonography, heat, and ice as indicated. Therapeutic exercises and neuromuscular education were used to improve patients' cervical range of motion, strength, and endurance, as well as shoulder and scapular stability and strength.
Patients' symptoms (pain and numbness) and response to therapy were monitored at each treatment session. Pain severity was scored by the patient using a standard 0 to 10 scale (0 equals “no pain” to 10 equals “hurts as much as you can imagine”). Frequency of pain and numbness was obtained by having the patient indicate the percentage of the 24-hour day when the symptoms were present. Patients completed a form describing their pain and numbness location, severity, and frequency during each week of treatment, and the details of these reported symptoms were reviewed and verified with them. Patients reported outcomes directly to the practicing physician.
A comprehensive reevaluation appointment with the physician was scheduled for each patient after every 2 weeks of treatment. The above symptoms-tracking protocol was used at each reevaluation, which included a neurological examination. Patients' responses to treatments were monitored and modified as indicated to maximize improvements.
Reported low back and lower extremity pain and numbness were coded in location, frequency, and severity categories. The locations used were lower back, hip or buttocks, proximal leg, distal leg, and foot. The pain level and percentage of the day symptoms were present were collected for each part of the lower body. Pain severity was coded on a 0 to 10 scale as severe (10 - 7), moderate (6 - 4), or mild (3 - 1), depending on the pain level the patient provided. The percentage of day was coded as constant (present more than 69% of a 24-hour day) or intermittent (present less than 70% of a 24-hour day).
Severity, frequency, and location were then compiled. With this system, patients could present with “severe intermittent proximal leg pain,” “constant mild lower back pain,” etc. Numbness had only 1 level of severity but could vary in location and be constant or intermittent.
Each patient received an improvement score based on the changes in his or her low back and lower extremity pain and numbness. Symptom severity and frequency collected at initial evaluation and at the end of the physical therapy program were compared. Points were awarded according to the amount of changes in symptoms: 1 point was awarded for shifting from constant to intermittent symptoms, intermittent to no symptoms, severe to moderate pain, moderate to mild pain, or mild to no pain, and 1 point was subtracted for any shift in the opposite direction.
Points were awarded for each location where symptoms were reported. For example, a patient with severe constant LBP who shifted to moderate intermittent LBP would be awarded 2 points (constant to intermittent and severe to moderate). If this patient experienced complete alleviation of his severe constant LBP (severe to moderate, moderate to mild, mild to none, constant to intermittent, intermittent to no symptoms), he was awarded 5 points, the highest possible score.
Numbness was treated as moderate pain (2 points). However, if a patient presented with constant severe pain and constant numbness and experienced resolution of all symptoms, he was still given only a 5.
For patients with symptoms in multiple locations, their points from each location were averaged. For example, if a patient had complete alleviation of severe constant foot pain (5 points) and no change in symptoms of severe constant LBP (0 points), he was awarded 2.5 points.
In a more complex example, a patient has severe constant LBP, moderate constant hip pain, severe intermittent proximal leg pain, mild constant distal leg pain, and constant foot numbness at the start of treatment and mild intermittent LBP, mild intermittent hip pain, complete alleviation of proximal leg pain, mild intermittent distal leg pain, and complete alleviation of foot numbness at its completion. The breakdown is 3 points for LBP (severe to moderate, moderate to mild, constant to intermittent), 2 points for hip pain (moderate to mild, constant to intermittent), 4 points for proximal leg pain (severe to moderate, moderate to mild, mild to no pain, intermittent to none), 1 point for distal leg pain (constant to intermittent), and 4 points for foot numbness (2 points for resolution of foot numbness-constant to intermittent, intermittent to none); the patient received 2.8 points.
We used this point system because it directly tracked the changes in patients' reported symptoms. It quantified the amount of change in symptoms reported and showed that change was occurring. Future studies can build on this one by using other tests that measure physical function, such as the Roland-Morris Disability Questionnaire and Oswestry Disability Index. For this study, however, we focused directly on the changes in reported symptoms with the described point system. Calculated percentages and the point system were the only statistical techniques used in this study.
Results
TABLE 1
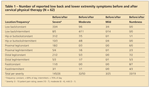
Number of reported low back and lower extremity symptoms before and after cervical physical therapy (N = 62).
Patient pain and numbness results are shown in Table 1. Total low back and lower extremity symptoms reported before and after completion of the physical therapy program were 213 and 120, respectively, calculating to an overall 44% reduction. Reports of constant symptoms shifted from 160 before physical therapy to 42 after physical therapy, calculating to 74% of them improving. The numbers of total intermittent symptoms before and after physical therapy were 53 and 78, respectively, suggesting that constant symptoms shifted to intermittent symptoms; in 93 reported complaints, constant or intermittent symptoms were completely alleviated.
Before therapy, there were 145, 32, and 3 complaints of severe, moderate, and mild pain, respectively, and 33 reports of numbness. After treatment, the numbers of severe, moderate, and mild pain were 26, 50, and 25, respectively, with 19 reports of numbness; 82% of severe complaints were alleviated.
Overall, pain severity was reduced or resolved. The number of complaints with total alleviation for each location was lower back, 13 (23%); hip/buttocks, 29 (55%); proximal leg, 13 (41%), distal leg, 23 (52%); and feet 15 (56%).
TABLE 2

Number of patients with 1, 2, 3, or 4 cervical disks displaced and mean improvement scores (N = 62).
The mean improvement score for all 62 patients was 3.12 ± 1.30. The mean scores for patients with and without spinal cord contact were 3.19 ± 1.27 and 2.91 ± 1.29, respectively, and for patients with and without spinal cord compression, 3.13 ± 1.32 and 3.11 ± 1.36, respectively.
The number of cervical disks displaced and mean improvement score of the studied patients are shown in Table 2. The mean score for the 51 patients who had previously received treatments for their lower body symptoms was 3.05 ± 1.29.
Discussion
Patients reported improvement of their low back and lower extremity pain and numbness after completion of a conservative physical therapy program targeted at the cervical spine. On average, low back and lower extremity pain and numbness decreased multiple times in frequency or severity, as indicated by the mean improvement score of 3.12.
Total low back and lower extremity symptoms were reduced by 44% and severe pain complaints by 82%, although reports of moderate and mild symptoms both increased. Some patients with incomplete alleviation of symptoms shifted from severe pain to moderate or mild pain. There were 74% fewer complaints of constant pain or numbness after physical therapy. Intermittent complaints increased by 25, leaving 93 constant or intermittent complaints with complete alleviation. Numbness complaints were reduced by 58%.
A physical therapy program designed to reduce symptomatic cervical disk displacements improved low back and lower extremity symptoms. Precisely 23% of low back symptoms were alleviated; the percentages of alleviation in the lower extremities were higher than 52%, other than in the proximal leg, with 41% alleviation. The pattern of improvement being greater in the distal lower extremities than in the proximal lower extremities and greater in the lower extremities than in the low back suggests that the treatment program resulted in centralization of lower body symptoms.
The physical therapy program was effective in improving lumbar symptoms for patients with and without actual spinal cord contact or compression. Lumbar symptoms were triggered by cervical disk displacements described to indent only the thecal sac without cord contact while the patient was resting supine. We think that when patients are erect and active, a combination of dynamic stressors, vascular insufficiency, and ischemia occur frequently and result in the pathophysiology of the cervical cord.
Similar improvements in lumbar symptoms occurred in patients with 1, 2, 3, and 4 displaced disks. The mean improvement score was highest for patients with 3 displaced disks, implying that multilevel involvement of the cervical spine does not result in less response to cervical treatments. Past studies have documented patients with displaced disks having their disks reabsorbed after cervical bracing, cervical traction, and other treatments.13,14 All patients had lumbar MRI findings of disk displacement, disk herniations, lumbar spondylotic changes, and lumbar spinal stenosis that contributed to the low back and lumbar symptoms that remained after treatments of the cervical spine.
The concept of cervical triggers preventing improvements in low back and lower extremity symptoms is suggested by 51 of the 62 patients having already received lumbar treatments without improvements. Each patient experienced improvements of his lumbar symptoms after a physical therapy program that was focused on the cervical spine. We recommend that patients with low back and lower extremity symptoms be examined for cervical lesions to manage the cervical trigger that may be present.
Conclusions
When a patient presents with a chief complaint of radicular low back and lower extremity symptoms, the natural focus of diagnosis and treatment is on the presenting lumbar symptoms and lumbar imaging findings. With this narrow focus, the complexity of presenting symptoms resulting from involvement of the cervical spine is not acknowledged. Posterior cervical disk displacements may be the trigger of low back and lower extremity symptoms in patients who have both. The cervical lesion results in dysfunction of the torso, which leads to lumbar pathology.
The data from this study showed that management of the cervical spine can result in reduction of lower body pain and numbness. Examination for an overlying cervical lesion is indicated when patients with low back and lower extremity symptoms are evaluated, especially if symptoms are persistent and recurrent. Workup of the cervical spine with imaging studies is recommended to isolate symptomatic overlying cervical lesions. If cervical lesions or pathology is found, the cervical spine should be managed accordingly to ensure full recovery from lumbar symptoms.
This study has limitations, and the results are not conclusive. We acknowledge that patients may have disk abnormalities but be asymptomatic. All patients in this study population had abnormal upper and lower extremity neurological findings. However, the primary complaints of all patients were low back and lower extremity symptoms. Cervical traction is recognized in the current texts as a treatment for patients with cervical disk displacements and herniations. However, the paucity of well-designed, randomized, controlled, prospective studies and the abundance of literature showing a lack of effectiveness of traction are acknowledged.4,15
In patients with lower body symptoms, the cause may be cervical disk displacements. There has been success both clinically and in this study with management of cervical disks to reduce lumbar symptoms. Our goal is to instigate more studies that examine cervical spine–triggered lumbar symptoms.
Comments about/problems with this article? Sendfeedback.
References:
References
1.
Low back pain. In: Green WB, DeHaven KE, Pfeffer GB, et al, eds.
Essentials of Musculoskeletal Care.
2nd ed. Rosemont, IL: American Academy of Orthopaedic Surgeons; 2001:553-555.
2.
Hart LG, Deyo RA, Cherkin DC. Physician office visits for low back pain: frequency, clinical evaluation, and treatment patterns from a U.S. national survey.
Spine (Phila Pa 1976).
1995;20:11-19.
3.
Deyo RA, Tsui-Wu YJ. Descriptive epidemiology of low-back pain and its related medical care in the United States.
Spine (Phila Pa 1976).
1987;12:264-268.
4.
Barr KP, Harrast MA. Low back pain. In: Braddom RL, Buschbacher RM, Chan L, et al, eds.
Physical Medicine and Rehabilitation.
3rd ed. Philadelphia: WB Saunders Company; 2007:883-929.
5.
Deyo RA, Rainville J, Kent DL. What can the history and physical examination tell us about back pain?
JAMA.
1992;268:760-765.
6.
Strine TW, Hootman JM. US national prevalence and correlates of low back and neck pain among adults.
Arthritis Rheum.
2007;57:656-665.
7.
Carette S, Fehlings MG. Clinical practice: cervical radiculopathy.
N Engl J Med.
2005;353:392-399.
8.
Cervical disc disease. In: Praemer A, Furnes S, Rice DP, et al, eds.
Musculoskeletal Conditions in the United States.
Rosemont, IL: American Academy of Orthopaedic Surgeons; 1992:22-23.
9.
Lipetz SJ, Lipetz DL. Disorders of the cervical spine. In: DeLisa JA, Gans BM, Walsh NE, et al, eds.
Physical Medicine and Rehabilitation.
4th ed. Philadelphia: Lippincott Williams and Wilkins; 2005:631-652.
10.
McGill SM. Developing the exercise program.
Low Back Disorders: Evidence-Based Prevention and Rehabilitation.
Champaign, IL: Human Kinetics; 2002:239-257.
11.
Kirkaldy-Willis WH, Wedge JH, Yong-Hing K, Reilly J. Pathology and pathogenesis of lumbar spondylosis and stenosis.
Spine (Phila Pa 1976).
1978;3:319-328.
12.
Saunders HD. Use of spinal traction in the treatment of neck and back conditions.
Clin Orthop Relat Res.
1983;179:31-38.
13.
Matsumoto M, Chiba K, Ishikawa M, et al. Relationships between outcomes of conservative treatment and magnetic resonance imaging findings in patients with mild cervical myelopathy caused by soft disc herniations.
Spine (Phila Pa 1976).
2001;26:1592-1598.
14.
Cervical myelopathy. In: Borenstein DG, Wiesel SW, Boden SD, eds.
Low Back and Neck Pain: Medical Diagnosis and Comprehensive Management.
3rd ed. Philadelphia: WB Saunders Company; 2004:278-282.
15.
Coheen I, Jouve C. Cervical radiculopathy. In: Frontera WR, Silver JK, Rizzo TD, eds.
Essentials of Physical Medicine and Rehabilitation.
2nd ed. Philadelphia: Saunders Elsevier; 2008:20-21.