Growing Evidence that Insulin Plays a Role in Etiology and Severity of Acne Vulgaris
A study in Postᶒpy adds to the growing evidence of a link between insulin and carbohydrate metabolism in the etiology and severity of acne vulgaris. While the clinical evidence on this connection is still disputed, the majority of recent studies has pointed to a significant connection between the condition and insulin levels.
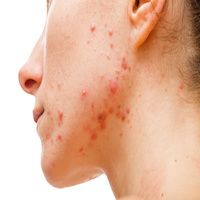
A study in Postᶒpy adds to the growing evidence of a link between insulin and carbohydrate metabolism in the etiology and severity of acne vulgaris. While the clinical evidence on this connection is still disputed, the majority of recent studies has pointed to a significant connection between the condition and insulin levels.
Acne isn’t just tough for patients to deal with, it’s a bit of a tough clinical nut; researchers know that some combination of hyperseborrhea, follicular hyperkeratinization, and propionibacterium are involved in pathogenesis, but the exact mechanism isn’t clearly known. Several studies have shown a link between diet and the pathogenesis of acne, and a few have demonstrated that a low glycemic index diet introduced an improvement in acne severity and a parallel improvement in insulin sensitivity in males with acne vulgaris.
The latest analysis looked at 243 patients clinically diagnosed with severe acne vulgaris and 156 healthy controls. A detailed history was taken from each participant and physical examinations were performed. The participants were excluded if they reported medications known to affect insulin metabolism, previous treatment with oral retinoids, hormone treatment for any reason in the previous three months, cigarette smoking, thyroid dysfunction, or a history of diabetes mellitus, hypertension, atherosclerotic vascular disease, malignancy, pregnancy or any other systemic inflammatory diseases.
The severity of the patients’ acne was evaluated using the Global Acne Grading System and the study included only patients with moderate to severe cases of acne vulgaris. There was no significant difference between the patient and control groups with respect to sex, age, or body mass index. While fasting blood glucose levels were not different between the groups (p > 0.05, 82.91 ±9.76 vs. 80.26 ±8.33), the fasting insulin levels were significantly higher in the patient group than in the control group (p < 0.001, 14.01 ±11.94 vs. 9.12 ±3.53). Additionally, there was a highly significant difference between the patient and control groups in terms of Homeostatic model assessment (HOMA) values, which indicate insulin resistance (p < 0.001, 2.87 ±2.56 vs. 1.63 ±0.65).
The study considered the usual suspects in acne development, including milk and chocolate, as well as other factors influencing insulin levels — including puberty – to account for their potential impact on the insulin levels of the study participants.
“These findings suggest that treatments prescribed for insulin resistance are worth investigating for treatment of severe acne vulgaris,” the authors concluded.