IBD Drugs Stay in Infants' Bodies If Given to Pregnant Mothers
Mothers’ inflammatory bowel disease (IBD) therapies may impact their newborns, according to findings published in Gastroenterology.
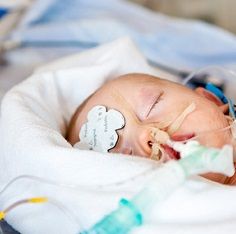
Mothers’ inflammatory bowel disease (IBD) therapies may impact their newborns, according to findings published in Gastroenterology.
Researchers from the University of Aarhus in Denmark investigated the concentrations of adalimumab and infliximab in the umbilical cord blood of 80 newborn infants and the rates of clearance after birth born to mothers with IBD. The researchers also examined how these rates were linked to drug concentrations in the mothers at birth and the risk of infection during the first year of the infants’ lives.
The study authors noted that not much is understood about in utero exposure and postnatal clearance of anti tumor necrosis factors (anti TNF) agents in neonates, so they chose to explore further.
Of these 80 women who gave birth at hospitals in Denmark, Australia, and New Zealand between March 2012 and November 2014, 36 received adalimumab and 44 received infliximab. There were 39 mothers who received concomitant thiopurines during their pregnancies. The researchers recorded data from medical files on IBD disease activity and tracked treatments before, during, and after pregnancy including measuring anti TNF agents from blood samples in umbilical cord and the infants for every three months until the drug was no longer detected.
Antibodies for anti TNF remained in the infants until they reached 12 months of age, the researchers reported. Adalimumab took an average of four months to clear the infants’ bodies, while infliximab took an average of 7.33 months.
“This prospective observational study shows that infant clearance of infliximab after exposure during pregnancy is slower than previously reported,” the study authors wrote. “More rapid clearance was seen with adalimumab”.
The researchers added that the relative risk for infection was 2.7 in infants if their mothers received the combination of an anti TNF agent and thiopurine, compared to the anti TNF monotherapy.
“Based on these results, we suggest that no live virus vaccine should be given during the first year of life in offspring of women treated with anti TNF during pregnancy,” the authors concluded.
“Pregnant women treated with combination therapy should receive counseling regarding potential risk of postnatal infections in their infant, which should be promptly assessed.”