Image IQ: Tender, Swollen, Joint Pain
A 62-year-old woman complained to her doctor about joint pain in her fingers. The joints in her fingers were warm, tender, and slightly swollen. Can you diagnose this patient?
(©VisualDx)
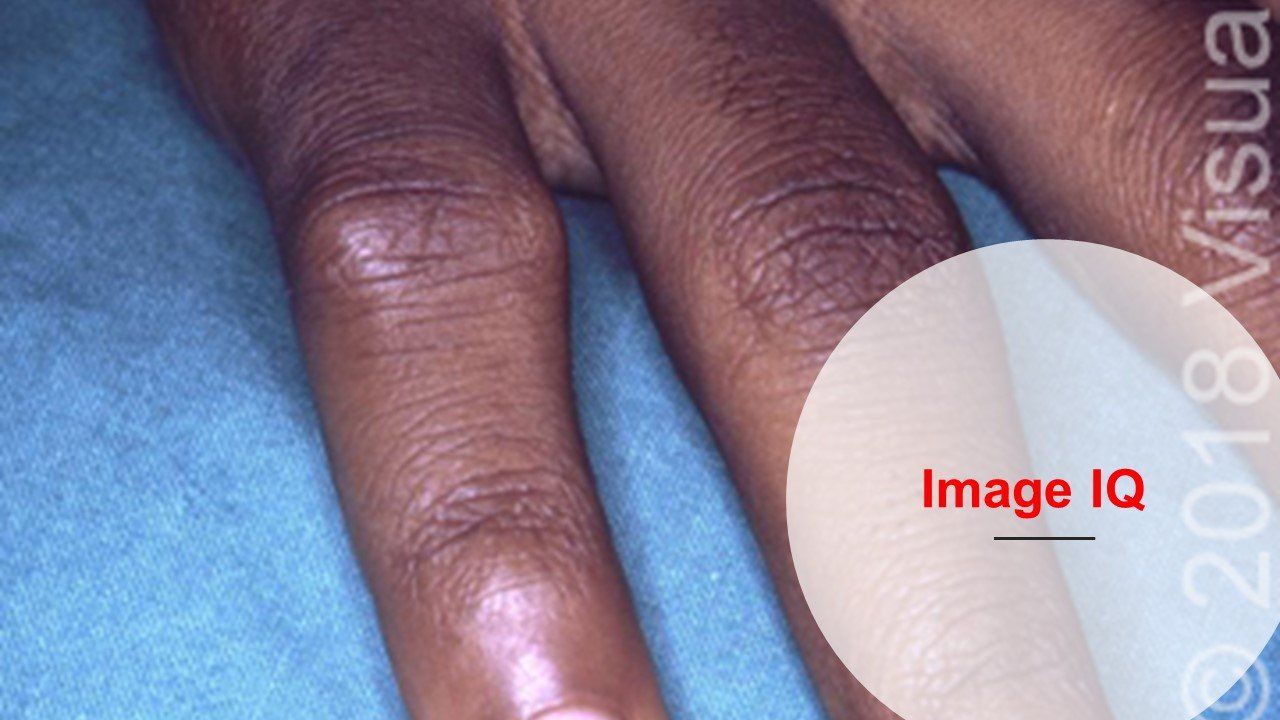
A 62-year-old woman complained to her doctor about joint pain in her fingers. The joints in her fingers were warm, tender, and slightly swollen. The discomfort started a few months ago and now it took about an hour every morning for the stiffness to decrease. Activity seemed to help the stiffness. If she was inactive for a long period, while reading a book or watching TV, the stiffness would return. She had been taking NSAIDs, which relieved the pain for a period of time.
Can you diagnose the patient? Use the differential builder in VisualDx as a guide.
A. Osteoarthritis
B. Rheumatoid arthritis
C. Adult-onset Still disease
D. Fibromyalgia
See the next page for the correct diagnosis.
The correct diagnosis is: B) Rheumatoid Arthritis
Synopsis: Rheumatoid arthritis (RA) is a chronic inflammatory joint and systemic disease that affects 1% of the adult population. It can occur in adults of all ages (peak onset 50-75) and is 3 times more common in women than men.
RA involves inflammation in the joint synovium, causing an inflammatory state that leads to articular cartilage loss and bony erosion, resulting in irreversible damage and functional impairment. The onset of disease is insidious, most typically presenting with symmetric polyarthritis described as pain, swelling, and inflammation of joints leading to stiffness after a period of inactivity. Some patients present with constitutional symptoms of malaise, fatigue, low-grade fevers, weight loss, and depressed mood. Patients may be anemic. Classically, this symmetrically distributed polyarthritis affects the small joints of the metacarpophalangeal (MCP), proximal interphalangeal (PIP), and metatarsophalangeal joints (MTP) early in disease. Other synovial joints may be involved including the elbows, shoulders, ankles, and knees. Of note, the C1-C2 joints of the spine and temporomandibular, sternoclavicular, or cricoarytenoid joints may be involved. Less common initial presentations include a monarticular or oligoarticular arthritis.
RA is labeled "seropositive" when rheumatoid factor (RF) and/or anti-citrullinated protein antibodies (ACPAs) are present. Seropositive disease tends to be more severe and associated with increased risk of systemic involvement. Rheumatoid nodules occur in up to 20% of RA patients and more frequently among patients with seropositive disease.
Initial evaluation of the patient presenting with joint pain should focus on determining whether the presenting arthritis pain is inflammatory vs. noninflammatory in nature. For example, inflammatory joint symptoms include a joint stiffness that occurs after inactivity – including in the morning after waking (>30 minutes of stiffness) – and improves with activity. Signs of inflammation such as redness, swelling, and warmth should prompt consideration of inflammatory and infectious arthritides.
Felty syndrome is an uncommon presentation of severe RA with splenomegaly, neutropenia, and sometimes lower extremity ulcerations. A diagnosis of large granular lymphocytic leukemia should be considered in any patient with a Felty-like presentation.
Patients with interstitial lung disease and RA have a genetic promotor variant MUC5B.
Palindromic RA is episodic RA with intervening symptom-free periods. It is not RF seropositive.
It has been reported that exposure to moderate to high levels of silica increases the risk for rheumatoid arthritis. This association is more common in males due to occupational exposure.
Advances in medical therapy have greatly improved prognosis, decreased functional impairment, and increased quality of life for patients with RA.
To learn more about RA, including ICD10 codes, visit VisualDx.
Learn more about this diagnosis on the VisualDx site: http://bit.ly/2GvikLn