New Diabetic "Sugar Sponges" Could Replace Insulin Injections
Sugar Sponges could absorb and expel sugar in blood as needed.
A trio of scientists from Tongji University in Shanghai, China are testing a diabetes treatment that has the potential to eliminate the need for insulin injections and antidiabetic drugs.
The new treatment is all about “controlling sugar levels with sugar,” and centers on the use of nano-sized “sugar sponges” — lectin-bound glycopolymersomes that are capable of regulating glucose through dynamic recognition of lectin and different carbohydrates, according to the study’s lead author Du Jianzhong.
Jianzhong’s sugar sponge has the potential to replace manually administered treatments like insulin injections and pills, because if successful, it would dually function as a glucose storage unit when levels are too high and a glucose distributor when levels are too low.
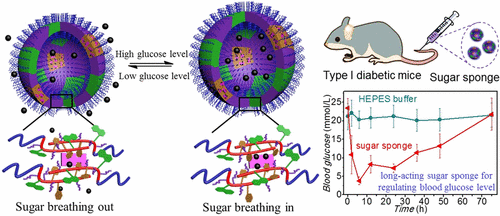
This is because, as the study’s abstract reads, the lectin bound in the glycopolymersome has a different affinity for the glucose in the blood and the glucosyl group in the glycopolymersome. Therefore, the sugar sponge can function as a glucose storage unit by dynamic sugar replacement — when glucose concentrations are too high, the lectin in the sugar sponge will bind and store the glucose from its surrounding solution, and when glucose concentration is too low, they can release the glucose as well.
Researchers were able to witness this process in vitro.
“This sugar-breathing behavior is characterized by a remarkable size change of the sugar sponge due to the swelling/shrinkage at high/low glucose levels, which can be used for blood sugar monitoring,” the study read.
The same process was witnessed in vivo in diabetic mice.
“In vivo, this sugar sponge showed an excellent antidiabetic effect for type I diabetic mice within 2 days upon one dose, which is much longer than traditional long-acting insulin,” researchers wrote.
If successful in future studies, sugar sponges could represent a profound transformation in diabetes treatment, which can be painful, difficult to manage, and increase risk of side effects like nerve damage, infections and insulin resistance.
Diabetes is “a long-term pain for those who are affected and must regulate their blood glucose level by frequent subcutaneous injection of insulin every day,” researchers wrote. “We propose a noninsulin and anti-diabetic drug-free strategy for regulating blood glucose level.”
In 2015, around 415 million people across the globe had diabetes, with an estimated total cost of $612 billion, and $245 billion in the United States. 90% of those affected had type II diabetes. While rates are expected to increase, management tacticts have improved significantly, according to the National Institutes of Health.
You can read the full study here.