Article
Novel Anti-Interleukin-23 Therapy Outperformed Current Treatment in Patients with Plaque Psoriasis
Author(s):
Successful preliminary trials revealed that treatment with a novel anti–interleukin-23 monoclonal antibody, guselkumab, (CNTO 1959/Janssen) was more effective at reducing the symptoms of plaque psoriasis than adalimumab.
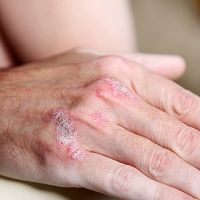
Successful preliminary trials revealed that treatment with a novel anti—interleukin-23 monoclonal antibody, guselkumab, (CNTO 1959/Janssen) was more effective at reducing the symptoms of plaque psoriasis than adalimumab.
Published in The New England Journal of Medicine, the study results from the latest phase 2b X-PLORE trial compared the safety and efficacy of guselkumab to adalimumab and placebo in nearly 300 patients with plaque psoriasis.
Patients in the guselkumab arm were randomized to receive one of 5 doses of the medication:
- 5 mg at weeks 0 and 4 and every 12 weeks thereafter
- 15 mg every 8 weeks
- 50 mg at weeks 0 and 4 and every 12 weeks thereafter
- 100 mg every 8 weeks
- 200 mg at weeks 0 and 4 and every 12 weeks thereafter
Patients in the adalimumab arm received the standard dosage for psoriasis. At week 16, patients in the placebo group were switched to guselkumab 100 mg every 8 weeks.
The study found that nearly 86% of patients afflicted with moderate-to-severe plaque psoriasis who were administered guselkumab (100mg) attained a Physician’s Global Assessment (PGA) score of 0 (cleared psoriasis) or 1 (minimal psoriasis) at the 16-week mark.
Treatment with other doses of guselkumab was also effective: 34% of patients in the 5-mg group, 61% in the 15-mg group, 79% in the 50-mg group, and 83% in the 200-mg achieved a PGA score of 0 or 1.
By comparison, only 7% of patients in the placebo group and 58% of the adalimumab group achived PGA scores of 0 or 1.
Guselkumab works by blocking the protein interleukin-23 (IL23), which significantly cleared the skin of treated patients.
Adalimumab is an established treatment for this condition, so the study authors believed, “It’s particularly promising that the higher doses of guselkumab were even more effective than adalimumab”.
Kristian Reich, MD, lead researcher and partner at Dermatologikum, Hamburg, Germany, said, “These findings provide important insights into the role of IL23 in psoriasis and the potential therapeutic benefit of guselkumab. My patients specifically like the long injection intervals.”
Katy Burris, MD, dermatology, North Shore-LIJ Health System in Manhasset, NY, concluded, “It should be kept in mind, though, that this is an early study with somewhat preliminary results, and more work needs to be done before one can fully assess the drug’s safety and efficacy.”




