Nonpharmacological treatment for low back pain
A serious underlying condition rarely is present in patients with low back pain (LBP), but the pain can be intense and severely limit home and work activities. For most patients with LBP, the cause is a nonspecific mechanical process; for those with acute symptoms, the course is self-limited. Initial treatments include activity modification, nonnarcotic analgesic agents, and patient education. For patients whose symptoms are not improving, referral for physical treatments is appropriate.
Low back pain (LBP)-pain experienced in the lumbosacral spinal and paraspinal regions, including the buttocks and upper thigh-is a common patient complaint. Although rarely the result of a serious condition, LBP can result in significant limitations in home and work activities and is a major cause of disability. Most patients with acute pain who are seen in a primary care setting improve within a month.1 However, persistent low-grade symptoms and recurrence are common.2 Although chronic symptoms develop in only 6% to 10% of patients, the high incidence of LBP makes the societal burden great.2,3
When evaluating patients who have LBP, the clinician's goal is to classify the symptoms into broad categories4:
•Back pain potentially associated with radiculopathy (radiating leg pain typically posteriorly localized to the knee or below) or neurogenic claudication (pain encompassing the buttock, groin, and anterior thigh that can radiate into the lower leg).
•Back pain potentially associated with another specific cause.
•Nonspecific LBP.
Primary care physicians most often give patients a diagnosis of nonspecific mechanical LBP, because reliably identifying the exact structure that gives rise to the local pain is difficult.5 Even when LBP is associated with specific imaging findings, such as degenerative disk disease or spondylolisthesis (anterior displacement, most often of the L5 vertebra over the S1), determining whether the patient's symptoms are caused by the finding can be challenging. A precise cause is more likely to be identified in patients who have radicular leg symptoms or nonmechanical disorders, such as cancer or infection. The duration of symptoms (acute, less than 4 weeks; subacute, 4 to 12 weeks; and chronic, more than 12 weeks) is a key determinant that influences the initial management of LBP.
A wide variety of therapies provided by various health care professionals are available for patients with LBP (Table 1). Given the abundance of available options and limited information about their relative benefits, primary care physicians may feel uncomfortable in devising a treatment plan tailored to a patient's
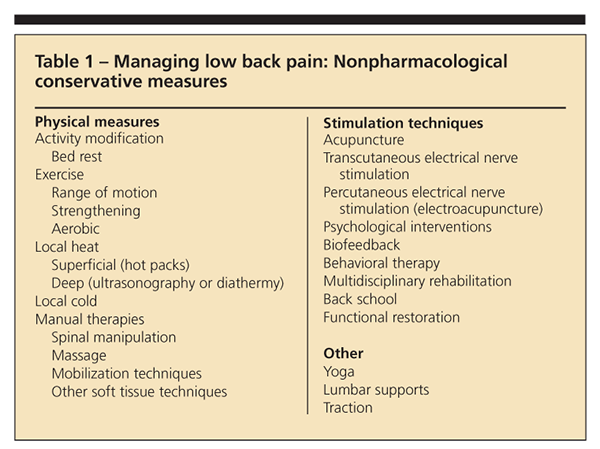
situation. Many patients turn to other care providers, such as complementary and alternative medicine (CAM) practitioners, often without informing their physician; a lack of satisfaction with "traditional" medical approaches may be a reason why.6 Diversity among back pain care providers is reflected in wide variations in the nature and frequency of testing, treatments, and referrals.7 As a result, large differences in costs are seen that appear to have little relationship with symptomatic and functional improvements.7,8
For most patients who have acute nonspecific LBP, initial treatment should focus on self-care with activity modification, use of medications or local heat for pain relief, and avoidance of factors that worsen symptoms (Figure 2).4,9 For patients who do not improve after 2 to 3 weeks, adding physical
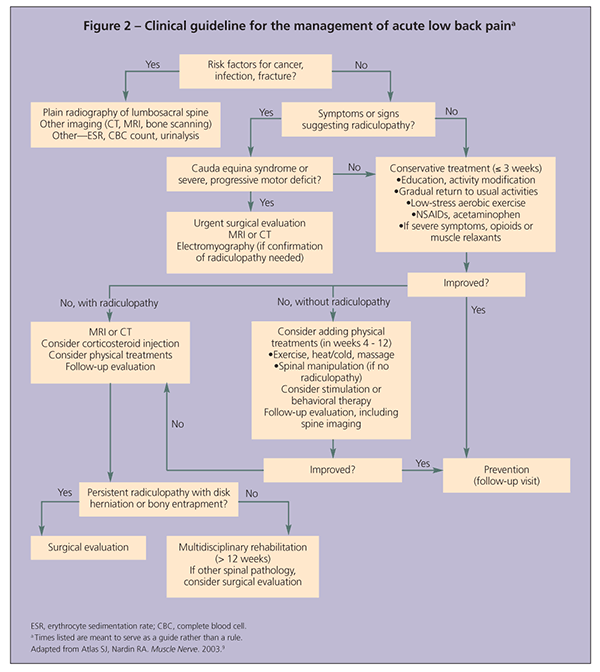
treatments often is recommended. For patients who have subacute or chronic LBP but no known cause that would guide treatment, physical treatments should include exercise.10
In this article, I highlight key management points that can guide primary care physicians in conservative treatment or referral of patients who have LBP. I focus on patients who have nonspecific LBP and who have had symptoms for more than a few weeks.
Patients need to know
what to expect
A key role of the primary care physician is to educate patients about reasonable expectations, starting at the first visit (Table 2). Reassure patients who have acute symptoms that the cause of their pain rarely is serious (so-called hurt does not mean harm); recommend treatments that control symptoms while healing takes place or that accelerate healing. For patients who have subacute or chronic symptoms, emphasize that decreasing pain and allowing for return to work and usual activities requires hard work from the patient and help from a health care professional (patient perceptions about receiving treatments passively should be discouraged).
Points to focus on include uncertainty in determining the precise cause of the pain and why it does
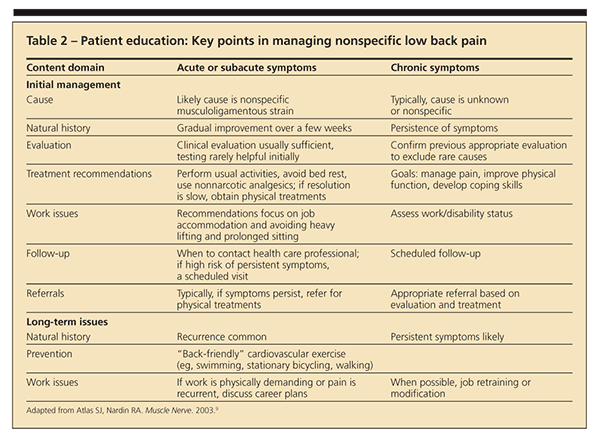
not negatively influence initial treatment; in most patients, the natural history of gradual pain resolution over a few weeks; why testing usually is not needed at first and how it can cause confusion by identifying problems that may not be related to the patient's symptoms; what physical treatments are available and when to obtain them; and when to check in with the primary care physician for an update. Given the time constraints of most office visits, written material should be used to help reinforce verbal communication.
If the patient is being referred to a CAM provider, especially if it is at the patient's request, inform the patient that this provider may have different views about the cause of pain, certainty of the diagnosis, and the specific benefits of his or her treatment. Because many treatments probably are effective for a number of different causes and identifying which treatments are more effective in which patients is difficult, downplay these different perspectives and instead focus on identifying what helps the pain.
Ask about previous episodes of
care and treatment preferences
If a patient currently has LBP that is similar in nature and intensity to past episodes, use past treatment experience when devising a management plan because it may help identify treatments that are more or less likely to be effective this time around.11 Even if the current episode differs from past ones, ask what treatment made the condition better or worse. Whether earlier treatment actually relieved pain or simply was given while pain relief was taking place, that treatment may be more likely to be effective again than treatments that have not been effective previously or have not been tried.
A growing consensus suggests that a range of acute and subacute LBP treatments are associated with similar outcomes.12,13 Therefore, patient preferences should be solicited when a plan is being devised.
When to refer
for physical treatments
The optimal timing of referral for physical treatments, as well as their frequency and duration, is unknown. In most patients with acute LBP, symptoms resolve within 2 to 4 weeks and higher costs and similar long-term outcomes are associated with various physical treatments. Therefore, treatments should be reserved for patients who do not respond adequately to initial conservative treatment, generally after 2 to 3 weeks, or sooner if symptoms are incapacitating.14 If a visit cannot be scheduled for a week or two, earlier referral may be considered so that the patient is seen in an appropriate time frame (3 to 4 weeks of symptoms).
Some patients who have risk factors for delayed recovery may benefit from earlier referral, but there is little evidence to indicate that doing so improves outcomes.15 Risk factors for persistent symptoms include previous LBP that required time off from work or resulted in disability, an expectation that passive treatments are effective, a belief that back pain is harmful or disabling, fear avoidance behaviors (such as incapacitating fear that any movement will increase pain), reduced activity out of proportion to symptoms, and depression or anxiety symptoms.
Which physical treatments?
Providers of physical treatments include chiropractors, osteopathic physicians, physical therapists, and massage therapists. Common therapies include a variety of back exercises; local heat therapies; manual treatments, such as spinal manipulation, massage, and other tissue mobilization techniques; and other modalities, such as back supports and traction. Manual therapy for LBP is the most common reason why patients seek care from CAM providers.6 Because therapeutic plans sometimes involve more than one physical treatment, it often is difficult to know their relative impact.
When LBP is acute and severe, specific back stretching and strengthening therapies generally do not help and can worsen symptoms. Therefore, early referral for physical treatments often focuses on passive therapies performed by the provider. For patients with subacute or chronic symptoms, however, there is good evidence to suggest that physical measures that actively involve the patient are more effective.12 How manual and other passive therapies may add to an active exercise program for persons with chronic pain is still unclear. However, primary care physicians should inform patients who are interested in trying manual therapies that active exercise should be an integral part of any management plan.
Recommend activity and
discourage bed rest
From the 1950s through the 1980s, bed rest was a cornerstone of treatment for LBP, largely because of expert opinion and physiological studies that showed lower disk pressure when a person is supine. Since then, studies have shown that continuation of usual activity with no recommendation for a defined period of bed rest results in better outcomes, even in those patients who have leg pain resulting from radiculopathy.4
When pain is severe and incapacitating, limited periods of bed rest are reasonable; early ambulation should be encouraged, but activities that provoke severe pain should be avoided. The latter include prolonged sitting and standing-patients should be instructed to walk and move their backs at regular intervals. Patients who have severe pain should also avoid strenuous activity, such as heavy lifting, climbing, or jogging, until symptoms diminish.
The role of physical therapy
Physical therapy exercises for treatment of LBP include specific back stretching and strengthening therapies (eg, Williams flexion exercises or McKenzie extension exercises) in various combinations, as well as aerobic exercises. Various physical therapy exercises have been shown to speed recovery, but the relative benefit of specific programs remains uncertain. Although back exercises may worsen symptoms when the pain is acute and severe, performance of low-stress aerobic activities early in the course, especially walking, is superior to bed rest or inactivity.4
When a patient is referred to a physical therapist early on, treatment should involve patient instruction about self-care and positioning, although this has not been shown to be associated with better outcomes.4 Hot or cold packs applied locally to the skin and heat applied with ultrasonography or diathermy often are used for LBP. Local heat may provide short-term relief of acute LBP.4 However, whether these treatments have a meaningful impact on improving recovery is unclear, partly because thermal therapies rarely are applied as the sole treatment but are included with other treatments, such as exercise or manual therapy.16
Although specific back exercises may not help during the acute phase, exercise is useful in preventing future episodes and improving symptoms in those patients who have persistent LBP.12,16 Ideally, a regular exercise routine should combine stretching and strength-building with endurance training. Physical therapy referral is common for patients who have radicular leg pain, but whether exercise therapy speeds recovery is unclear.16
Consider spinal
manipulation therapy
Spinal manipulation most often is associated with chiropractic care, but it also is provided by others, including osteopathic physicians and some physical therapists. Chiropractors are the most frequent providers of CAM care for persons with LBP. Often, patient satisfaction with care obtained from CAM providers is higher than satisfaction with physician-directed care.7,8 Regardless of whether referral for spinal manipulation is patient- or provider-initiated, primary care physicians should communicate to patients information about what they should expect in timing of improvement and treatment duration.
Spinal manipulation is thought to hasten symptom recovery modestly compared with placebo treatments, but outcomes are similar to those of other active treatments. Therefore, primary care physicians can include spinal manipulation as a reasonable treatment option for acute LBP not controlled with self-care options, especially if the patient asks about such treatments and they are covered by the patient's health insurance or he has other means to cover the costs.
Spinal manipulation and other manual therapies often are provided for patients who have chronic LBP; they have been shown to have moderate but short-term benefits.12 There is no evidence to indicate that spinal manipulation or other manual therapies offer long-term benefit for chronic pain or prevent acute recurrences.17,18 Although spinal manipulation and other manual therapies may be offered as a "preventive" treatment, primary care physicians should advise patients that exercise works better. Because spinal manipulation has not been shown to help patients with radicular leg symptoms, generally it should not be recommended.
The role of massage and other
soft tissue treatments
There are many forms of massage and other soft tissue and mobilization techniques. Whether certain techniques provide better outcomes than others do remains to be proved.
Although patients generally associate massage with CAM providers, physical therapists often use massage. Nonspinal manipulation therapies have been evaluated in fewer studies, especially therapies for patients with acute symptoms.12 For patients with chronic LBP, massage shows results similar to those for spinal manipulation and acupuncture.12,18-20 The long-term benefit of massage for chronic LBP is unclear.
Are other physical modalities effective?
Yoga can be considered an exercise-based therapy, but it also includes other components, such as relaxation techniques. Some forms of yoga may be helpful for patients with chronic LBP,21 but no systematic reviews are yet available.12 Lumbar supports, such as braces and corsets, sometimes are used to prevent or manage LBP. Evidence does not support their use in preventing LBP, and it is unclear whether they help patients with LBP.12,22 Spinal traction has not been shown to be effective for acute LBP with or without radicular leg pain,12,23 and there is no evidence of benefit in patients with chronic pain.
Acupuncture and other stimulation techniques
Acupuncture has been shown to provide moderate, short-term benefit for those with chronic LBP.12 However, some studies that compared acupuncture with sham acupuncture have shown similar results.12,18,24 Few studies have evaluated acupuncture in patients who have acute symptoms with or without radiculopathy.12,18
Transcutaneous electrical nerve stimulation (TENS) generally has not been shown to be effective in patients who have chronic LBP.12,25 The benefit of percutaneous electrical nerve stimulation, which combines features of TENS and electroacupuncture, is uncertain for LBP.26
Managing patients who are not improving
For patients who are not improving after a course of physical therapy, the primary care physician should review the course of the symptoms, the treatments received, and the patient's reported response. Specific questions should address activity limitation, work issues, and what improves or worsens the pain. The primary care physician should reinforce the key educational points previously described.
Patients who have subacute or chronic pain should be asked about personal treatment goals, both short- and long-term, that go beyond pain relief, especially because a "cure" cannot be guaranteed. If the patient is not working because of his symptoms, does he want to go back to work? To the same job? What activities cannot be performed that he wants to perform? How active does he want to be in finding alternatives that meet his goals? Referrals for further evaluation and treatment should be based on the patient's stated goals and preferences using shared decision-making techniques.27
Psychological treatment of chronic pain
A variety of psychological therapies have been used to treat patients who have LBP, typically those with chronic symptoms.12 Biofeedback involves giving external feedback to translate the physiological activity of muscular response (often using electromyography) into visual or auditory signals that help patients reduce their muscle tension and pain. However, the results of studies have been mixed and biofeedback generally is not considered to be effective in patients who have chronic LBP.28
A variety of behavioral approaches are used to reduce impairment by decreasing maladaptive pain thoughts, feelings, and beliefs. These include operant conditioning (using positive reinforcement of healthy behaviors and time-contingent pain management), cognitive therapy (using cognitive restructuring methods, such as imagery and attention diversion), and respondent techniques (using relaxation to modify physiological responses). The cognitive-behavioral therapy technique has been shown to be moderately effective for chronic LBP and demonstrates better evidence than progressive relaxation.12,28
Depression and anxiety symptoms are common in patients who have chronic LBP. Regardless of whether such symptoms precede or are a result of the back problem, antidepressant therapy is appropriate for patients who have depressive symptoms and chronic pain.29 Serotonergic-noradrenergic agents, such as tricyclic antidepressants, may have more consistent effects than serotonergic agents.13
Multidisciplinary rehabilitation programs
for work-related or chronic pain
These programs combine psychological, behavioral, and educational interventions with physical rehabilitation. Multidisciplinary components often are found in functional restoration programs that often are work-based but may be confused with "back schools," which generally provide only a structured educational program in a group setting. Results of educational programs alone have been modest at best.
For patients who have occupational or chronic LBP, intensive multidisciplinary rehabilitations reduce pain and improve function compared with alternative treatments.12,30 However, work-related outcomes have been mixed.
When to consider an aggressive
rehabilitation program
Although exercise has been shown to improve outcomes in patients who have chronic LBP, many physical treatments are passive in nature. Combined with recommendations to avoid activities that worsen symptoms, such treatments may lead to less active patients, not more active ones.
An alternative concept of care focuses on programs of aggressive physical therapy-a "no pain, no gain" perspective that emphasizes active rather than passive therapies. These exercise-based programs provide intensive, graded physical activity during longer sessions that occur 2 or 3 times a week for 1 or 2 months, generally under the supervision of a physical medicine physician.31
Unlike comprehensive programs that generally combine multiple standard treatments into 1 program, aggressive rehabilitation focuses on physical activity. Mental preparation and coping, key aspects of managing pain associated with such exertion, are incorporated into the exercise regimen rather than taught in group-learning sessions. There is little evidence to compare these programs with other treatment modalities or programs.4 Success requires highly motivated patients who can cope with increased pain that often occurs early on.
References:
References1. Coste J, Delecoeuillerie G, Cohen de Lara A, et al. Clinical course and prognostic factors in acute low back pain: an inception cohort study in primary care practice. BMJ. 1994;308:577-580.
2. Henschke N, Maher CG, Refshauge KM, et al. Prognosis in patients with recent onset low back pain in Australian primary care: inception cohort study. BMJ. 2008;337:a171.
3. Carey TS, Garrett JM, Jackman AM. Beyond the good prognosis: examination of an inception cohort of patients with chronic low back pain. Spine (Phila Pa 1976). 2000;25:115-120.
4. Chou R, Qaseem A, Snow V, et al. Diagnosis and treatment of low back pain: a joint clinical practice guideline from the American College of Physicians and the American Pain Society. Ann Intern Med. 2007;147:478-491.
5. Atlas SJ, Deyo RA. Evaluating and managing acute low back pain in the primary care setting. J Gen Intern Med. 2001;16:120-131.
6. Eisenberg DM, Davis RB, Ettner SL, et al. Trends in alternative medicine use in the United States, 1990-1997: results of a follow-up national survey. JAMA. 1998;280:1569-1575.
7. Carey TS, Garrett J, Jackman A, et al. The outcomes and costs of care for acute low back pain among patients seen by primary care practitioners, chiropractors, and orthopedic surgeons. The North Carolina Back Pain Project. N Engl J Med. 1995;333:913-917.
8. Cherkin DC, Deyo RA, Battié M, et al. A comparison of physical therapy, chiropractic manipulation, and provision of an educational booklet for the treatment of patients with low back pain. N Engl J Med. 1998;339:1021-1029.
9. Atlas SJ, Nardin RA. Evaluation and treatment of low back pain: an evidence-based approach to clinical care. Muscle Nerve. 2003;27:265-284.
10. UK BEAM Trial Team. United Kingdom back pain exercise and manipulation (UK BEAM) randomised trial: effectiveness of physical treatments for back pain in primary care. BMJ. 2004;329:1377.
11. Lutz GK, Butzlaff ME, Atlas SJ, et al. The relation between expectations and outcomes in surgery for sciatica. J Gen Intern Med. 1999;14:740-744.
12. Chou R, Huffman LH; American Pain Society; American College of Physicians. Nonpharmacologic therapies for acute and chronic low back pain: a review of the evidence for an American Pain Society/American College of Physicians clinical practice guideline [published correction appears in Ann Intern Med. 2008;148:247-248]. Ann Intern Med. 2007;147:492-504.
13. Chou R, Huffman LH; American Pain Society; American College of Physicians. Medications for acute and chronic low back pain: a review of the evidence for an American Pain Society/American College of Physicians clinical practice guideline [published correction appears in Ann Intern Med. 2008;148:247-248]. Ann Intern Med.2007;147:505-514.
14. Deyo RA, Weinstein JN. Low back pain. N Engl J Med. 2001;344:363-370.
15. Linton SJ, Halldén K. Can we screen for problematic back pain? A screening questionnaire for predicting outcomes in acute and subacute back pain. Clin J Pain. 1998;14:209-215.
16. van Tulder M, Malmivaara A, Esmail R, Koes B. Exercise therapy for low back pain: a systematic review within the framework of the Cochrane Collaboration Back Review Group. Spine (Phila Pa 1976). 2000;25: 2784-2796.
17. Assendelft WJ, Morton SC, Yu EI, et al. Spinal manipulative therapy for low back pain: a meta-analysis of effectiveness relative to other therapies. Ann Intern Med. 2003;138:871-881.
18. Cherkin DC, Sherman KJ, Deyo RA, Shekelle PG. A review of the evidence for the effectiveness, safety, and cost of acupuncture, massage therapy, and spinal manipulation for back pain. Ann Intern Med. 2003;138:898-906.
19. Cherkin DC, Eisenberg D, Sherman KJ, et al. Randomized trial comparing traditional Chinese medical acupuncture, therapeutic massage, and self-care education for chronic low back pain. Arch Intern Med. 2001;161:1081-1088.
20. Furlan AD, Brosseau L, Imamura M, Irvin E. Massage for low-back pain: a systematic review within the framework of the Cochrane Collaboration Back Review Group. Spine (Phila Pa 1976). 2002; 27:1896-1910.
21. Williams K, Abildso C, Steinberg L, et al. Evaluation of the effectiveness and efficacy of Iyengar yoga therapy on chronic low back pain. Spine (Phila Pa 1976). 2009;34:2066-2076.
22. Jellema P, van Tulder MW, van Poppel MN, et al. Lumbar supports for prevention and treatment of low back pain: a systematic review within the framework of the Cochrane Back Review Group. Spine (Phila Pa 1976). 2001;26:377-386.
23. Bigos SJ, Bowyer OR, Braen GR, et al. Acute Low Back Problems in Adults. Clinical Practice Guideline No. 14. Rockville, MD: US Dept of Health and Human Services; 1994. AHCPR publication 95-0642.
24. NIH Consensus Development Conference. Acupuncture. JAMA. 1998;280:1518-1524.
25. Khadilkar A, Odebiyi DO, Brosseau L, Wells GA. Transcutaneous electrical nerve stimulation (TENS) versus placebo for chronic low-back pain. Cochrane Database Syst Rev. 2008;(4):CD003008.
26. Ghoname EA, Craig WF, White PF, et al. Percutaneous electrical nerve stimulation for low back pain: a randomized crossover study [published correction appears in JAMA. 1999;281:1795]. JAMA. 1999;281:818-823.
27. Deyo RA, Cherkin DC, Weinstein J, et al. Involving patients in clinical decisions: impact of an interactive video program on use of back surgery. Med Care. 2000;38:959-969.
28. Ostelo RW, van Tulder MW, Vlaeyen JW, et al. Behavioural treatment for chronic low-back pain. Cochrane Database Syst Rev. 2005;(1):CD002014.
29. Urquhart DM, Hoving JL, Assendelft WW, et al. Antidepressants for non-specific low back pain. Cochrane Database Syst Rev. 2008;(1):CD001703.
30. Karjalainen K, Malmivaara A, van Tulder M, et al. Multidisciplinary biopsychosocial rehabilitation for subacute low back pain among working age adults. Cochrane Database Syst Rev. 2003;(2):CD002193.
31. Cohen I, Rainville J. Aggressive exercise as treatment for chronic low back pain. Sports Med. 2002;32:75-82.