Osteoporosis Drug Abaloparatide Performs Well in Phase 3 Trial, but Future Research Still Needed
While outperforming placebo, thee was not much separation between the new drug and an existing treatment, teriparatide, and it is unclear whether the two share risks.
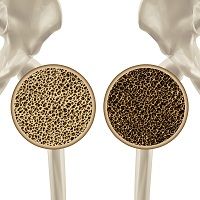
Abaloparatide, an injectable new synthetic peptide designed for the treatment of osteoporosis, performed well against placebo in a recent randomized trial.
Over the course of 18 months, researchers at the Colorado Center for Bone Research administered abaloparatide, teriparatide (FDA approved and sold by Lilly as Forteo), or placebo to over 2,400 female participants with an average age of 69. A total of 1,901 of them completed the study, which was recently published in JAMA.
Osteoporosis is at the root of thousands of fractures in women over the age of 50. The study cited another that estimated about 3.4 million women in the US between the ages of 50 and 69 suffered from the degenerative bone condition.
In the trial, vertebral fractures occurred less frequently in the two treatment groups than in the placebo group. Approximately 4.22% of those receiving the placebo (n=30) suffered a fracture, as opposed to 0.84% (n=6) in the teriparatide group and 0.58% (n=4) in the abaloparatide group. Additionally, hypercalcemia (abnormally high levels of calcium in the blood) was observed in 3% fewer of those on the abaloparatide treatment than on teriparatide (3.4% and 6.4%, respectively).
While certainly more effective than placebo, a difference of two fractures in a study of hundreds does not leave much separation between the new treatment and the existing one. Forteo is accompanied by warnings of a potential link to malignant bone tumors, and the risk differences between its generic form, teriparatide, and this new drug, abaloparatide, will, indeed, be an area for research in the future. Abaloparatide is seeking FDA approval.
The study’s press release included an attached editorial written by Anne R. Cappola, MD, Sc.M., University of Pennsylvania, and Associate Editor of JAMA, and Dolores M. Shoback, MD, University of California, San Francisco. In it, they wrote, “The bar is high for any preventive treatment—in the efforts to prevent a fracture that may or may not ever occur, prescribers do not want to prescribe a therapy that causes a new problem.”