Article
Plaque Psoriasis Treated With Tildrakizumab Shown to be Effective in Real-World Settings
Author(s):
Research suggests that tildrakizumab may be useful in real-life settings against moderate-to-severe plaque psoriasis.
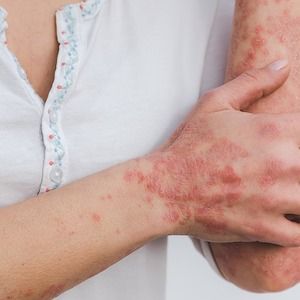
A recent study found that treatment of moderate-to-severe plaque psoriasis with tildrakizumab was effective up to 36 weeks in a real-world setting.
While several effective biological therapies have been developed to treat plaque psoriasis, few have shown to be well-tolerated. When tildrakizumab—a monoclonal antibody—was assessed in two phase 3 trials prior to this study, it was shown to be safe and effective.
This study, led by Alessio Gambardella, MD, and Gaetano Licata, MD, of the University of Campania Luigi Vanvitelli’s Department of Mental and Physical Health and Preventive Medicine, expanded upon these previous studies by allowing the treatment of patients with other comorbidities and varying other clinical characteristics.
“In this retrospective study we evaluated the efficacy of tildrakizumab in 30 patients with moderate to severe plaque [psoriasis] up to 36 weeks in a real-world setting,” Gambardella and colleagues wrote. “The majority of patients were currently employed, had little time to travel to a hospital and therefore suitable for treatment every 12 weeks.”
Research and Methods
The investigators used a retrospective study of 30 total participants with moderate-to-severe plaque psoriasis (PsO). The study involved the participants being treated with 100 mg of tildrakizumab and then observed for 36 weeks in a real-world setting.
Most of the participants in the study were employed and, consequently, were only able to visit the hospital every 12 weeks. The primary exclusion criteria for the recruited participants was that they were required to have moderate-to-severe PsO, with body surface area involvement being ≥10%, a Physician's Global Assessment (PGA) score of ≥ 3, and a Psoriasis Area and Severity Index (PASI) score of ≥ 12.
Additionally, the participants had to have either failed to respond or have side effects or contraindications to a minimum of 2 conventional psoriasis treatments. The investigators treated the participants with 100 mg of tildrakizumab through subcutaneous injection at weeks 0, 4, and every 12 of the following weeks.
The investigators assessed the clinical efficacy of the treatment by using participants’ PASI scores at weeks 4, 12, 24, and 36. In addition, they used the PGA scores, Dermatology Life Quality Index (DLQI) scores, and Health-Related Quality of Life (HRQoL) scores.
Study Results
The investigators found that participants’ PASI scores of less than 3 were reported following 12, 24, and 36 weeks in 86.7%, 100%, and 100% patients, respectively, treated with tildrakizumab.
They also found that PASI scores substantially decreased from 17.6 ± 4.7 at baseline to 4.7 ± 4.7 and 1.1 ± 3.9 at 4 and 12 weeks, remaining less than 1 up to 36 weeks (P < 0.001 versus baseline). Furthermore, PASI −75,–90, and −100 responses were achieved in 100%, 96.7%, and 60% of participants respectively at 36 weeks.
The research team reported that DLQI also decreased significantly from baseline (13.8 ± 2.9) to 3.6 ± 1.6 by 4 weeks, 1.4 ± 0.6 by 12 weeks, and 0 at weeks 24 and 36 (P < 0.001 versus baseline).
Additionally, a multivariate regression demonstrated that tildrakizumab treatment’s effect on DLQI and PASI scores by 4 weeks was independent from the variables of gender, age, disease duration, BMI, previous biologic, or the existence of comorbidities.
“Tildrakizumab was found to be effective and safe in moderate-to-severe plaque PsO in real-life clinical practice up to 36 weeks,” they wrote. “This benefit was independent of other predictor variables, therefore allowing it to be administered to patients with a range of clinical characteristics (including previous biological treatment) and the presence of comorbidities.”
This study, “Treatment of moderate-to-severe plaque psoriasis with tildrakizumab in the real-life setting,” was published on Wiley Online Library.




