Platelet-Rich Plasma Update: Clinical Use in Musculoskeletal Care
Platelet-rich plasma (PRP) initially was used in 1987 as a means of decreasing homologous blood product transfusions during open heart surgery.1
ABSTRACT: Platelet-rich plasma (PRP) therapy has been evaluated for its effect on acute and chronic tendinopathies, ligament rupture, acute fracture healing, bone nonunions, muscle injuries, and degenerative joint disease, as well as surgical outcomes. The concept of using PRP to enhance local tissue healing is based on several growth factors. Once the platelet-rich graft has been prepared, it is administered directly to the injury site. The associated risks mimic those of any traditional percutaneous injection. The most common patient complaint is pain at the treatment site. PRP therapy offers great promise in musculoskeletal medicine, but an abundance of level 1 data to support its efficacy is still lacking. PRP therapy seems to show its greatest potential in chronic tendinopathy conditions. (J Musculoskel Med. 2012;29:96-101)
Platelet-rich plasma (PRP) initially was used in 1987 as a means of decreasing homologous blood product transfusions during open heart surgery.1 Since then, clinicians have been using elevated concentrations of autologous growth factors to enhance healing in such areas as oral and maxillofacial surgery, plastic and reconstructive surgery, cardiovascular medicine, ophthalmology, otolaryngology, and wound management.
About a decade ago, PRP became a hot topic in orthopedic surgery and musculoskeletal medicine. The therapy has been evaluated with regard to its effect on acute and chronic tendinopathies, ligament rupture, acute fracture healing, bone nonunions, muscle injuries, degenerative joint disease, and other disorders, as well as surgical outcomes.
Until a few years ago, the investigational use of PRP therapy was far from mainstream as researchers and clinicians were busy trying to sort out just how and when to use growth factors to provide better patient care and enhanced outcomes. Then things changed. PRP was thrust into the public spotlight when a growing population of professional athletes-such as golf superstar Tiger Woods, baseball Cy Young award winner Cliff Lee, football Super Bowl MVP Hines Ward, and tennis ace Rafael Nadal-began using PRP therapy to return to play faster after soft tissue injuries, such as ligament sprains, muscle strains, and chronic tendinitis. As a result of the ensuing media coverage surrounding the purported success that these athletes experienced, PRP therapy has seen a tremendous increase in demand from the general patient population.
An increase in public awareness of PRP therapy, along with the promise of what it may offer in clinical medicine, has placed it front and center as an orthobiologic debate topic. In this article, I offer information about PRP therapy, explore its current use in orthopedic medicine, define the many questions that still surround its use, and investigate future considerations for the use of PRP therapy in musculoskeletal care.
WHAT IS PRP?
Although platelets most frequently are associated with hemostasis, the responsibilities of these discoid, anucleated cells extend far beyond platelet plug formation. In fact, they also play a reparative role. Among other contents, platelets carry storage organelles-known as granules (dense and α)-that spill their contents on activation. The dense granules contain adenosine triphosphate, adenosine diphosphate, serotonin, and calcium; they are chiefly responsible for the coagulation cascade.
The α granules contain, among other things, multiple growth factors and cytokines that in response to platelet activation are released via exocytosis to play a vital role in initiating and supporting the 3 stages of healing-inflammation, proliferation, and remodeling. The known growth factors on which the concept of using PRP to enhance local tissue healing are based include the following:
• Platelet-derived growth factor.
• Vascular endothelial growth factor.
• Transforming growth factor 1.
• Fibroblast growth factor.
• Epidermal growth factor.
• Hepatocyte growth factor.
• Insulin-like growth factor 1.
From stimulating angiogenesis to regenerating myocytes to enhancing the proliferation and migration of mesenchymal stem cells to the site of damage, growth factors exert a heavy influence on the biology of their surroundings. Therefore, they may have a positive influence in clinical situations that require rapid healing and tissue regeneration.
PRP consists of a supraphysiological concentration of platelets that on activation secrete a supraphysiological concentration of growth factors. Although the average concentration of platelets in whole blood is 200,000/μL, PRP preparations may contain anywhere between 2 and 8 times baseline values, depending on certain patient variables and the PRP preparation system used.
There is debate as to what the ideal platelet concentration of PRP should be. According to Marx,2 a “therapeutic PRP” should have a platelet concentration 300% to 400% greater than that of whole blood. It has been postulated that lower concentrations do not enhance tissue healing and that higher concentrations may be of no benefit.3
GRAFT PREPARATION AND ADMINISTRATION
Preparation
PRP often is prepared and administered in the orthopedic clinic with one of a variety of FDA-approved, closed-system commercial products. Whole blood is obtained from the patient by venipuncture through a large-bore needle to prevent lysis and premature platelet activation. An anticoagulant (eg, anticoagulant citrate dextrose solution formula A) may be added. Although filtration and plasmapheresis techniques are available,3 most often the blood is then centrifuged to isolate the platelets in their highly concentrated state.
Traditionally, a double centrifugation process was used; however, many commercially available PRP preparation kits now use single centrifugation to separate red blood cells from the buffy coat and serum layers. The buffy coat contains a small volume of plasma with a high concentration of platelets along with white blood cells (WBCs), making it the platelet-rich component. The overlying serum layer, the “platelet-poor” component, is discarded. This adjustment in graft preparation may have been made because research suggests that a double centrifugation technique tends to alter platelet morphology and requires more time and larger volumes of blood.3,4
An alternative method of PRP graft preparation involves leukocyte-poor PRP. This is produced through a shorter single centrifugation process that concentrates platelets in a small volume of plasma while excluding the majority of WBCs. Some authors define PRP as only platelets, whereas others note that PRP may also have increased concentrations of WBCs. The WBCs within some forms of PRP contain important cytokines and enzymes.
Once the platelet-rich product is obtained, it can be activated exogenously or endogenously to initiate degranulation and growth factor release. Exogenous platelet activation occurs ex vivo and requires the provider to add thrombin or calcium chloride to the PRP graft. Endogenous activation occurs in vivo and involves injecting the platelet-rich product directly into the target tissue and relying on contact with collagen or other biochemical mediators for clot formation and growth factor release. Some authors propose that endogenous activation results in a more sustained release of growth factors that may mimic a natural healing response more closely. Either way, 95% of a platelet’s growth factors are released within 10 minutes of activation.2
Administration
Once the platelet-rich graft has been prepared, it is administered directly to the site of injury, usually with image-guided injection using fluoroscopy, CT, or ultrasonography (US) for real-time visualization to ensure accurate placement. If the graft is activated exogenously, the addition of thrombin or calcium chloride to the PRP results in polymerization of fibrin from fibrinogen, which creates a gelatinous or putty-like structure that can be placed directly into the region of injury or sutured at the surgical site. Another route of administration often used intraoperatively includes topical application that combines the PRP with thrombin via a dual spraying device.
PRP generally is thought to be an inherently safe management modality. Because it is autogenous, there is no concern about transmissible diseases or rejection-related issues (eg, graft versus host disease) such as are seen with allogeneic transplants. Because all commercially available PRP preparation kits are closed systems, the potential for contamination is limited.
PRP itself has been found to possess antimicrobial characteristics that further limit the potential for infection.5 In addition, there is no known danger of carcinogenesis or tumor growth with platelet-rich products as has been associated with some stem cell therapies.
The risks associated with PRP therapy mimic those of any traditional percutaneous injection. They include bleeding, damage to nearby neurological or vascular anatomy, hollow organ puncture, and infection. If bovine thrombin is used to activate the PRP exogenously before in vivo application, there is potential for allergic reaction. Activation with calcium chloride or endogenous thrombin eliminates that risk.
TABLE 1
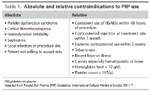
Absolute and relative contraindications to PRP use
The most common patient complaint is pain at the treatment site resulting from the injection and the ensuing acute inflammatory response, a result of the desired effect.6 Among other things, PRP use is contraindicated in patients who have thrombocytopenia or a condition of platelet dysfunction. Recent use of anti-inflammatories and other factors also are considered during patient selection. There are several absolute and relative contraindications to PRP use (Table 1).
ORTHOPEDIC APPLICATIONS
A healthy amount of evidence suggests that PRP therapy offers great promise in musculoskeletal medicine. In vitro laboratory research and clinical studies have investigated its merit in both soft tissue conditions and osseous healing. However, an abundance of level 1 data to support the efficacy of PRP therapy is still lacking.
Currently, much of what is guiding the use of PRP in orthopedic medicine is cohort data, conclusions drawn from case studies, and theory generated by in vitro and animal studies. Still, much of that information is undeniably compelling. Several recent clinical studies have involved the use of PRP therapy in the field of orthopedics.
Tendon and Muscle Healing
PRP therapy seems to show its greatest potential when used for chronic tendinopathy conditions, such as epicondylitis. Mishra and Pavelko7 prospectively evaluated recalcitrant cohort cases of medial and lateral epicondylitis after injection of buffy coat PRP or bupivacaine. They noted greater clinical improvement in the PRP group by 8 weeks postinjection, with continued improvement at just over 2 years.
In what probably are the most convincing findings available thus far, Peerbooms and associates8 provided level 1 evidence by comparing unactivated PRP with corticosteroid injection for chronic lateral epicondylitis. The PRP group eventually exhibited a greater reduction of symptoms than did the corticosteroid group, as well as better functioning by Visual Analog Scale and self-report questionnaire, with sustained improvement over time.
Kon and colleagues9 conducted a prospective cohort study to examine PRP effects on chronic patellar tendinitis in which conservative means of treatment had not been successful. They observed less pain and statistically significant improvement from pretreatment levels after 3 injections of activated PRP administered every 15 days.
There also have been PRP trials in patients with plantar fasciitis. Barrett and Erredge10 retrospectively studied 9 patients treated with US-guided PRP injections. After 1 year, 7 of 9 patients had experienced a complete resolution of symptoms.
A large, multicenter, level 1 trial that investigated PRP use for chronic plantar fasciitis is under way in Europe.11 The results should further contribute to the body of evidence for or against PRP therapy for this common malady.
PRP therapy has not always produced promising results in the setting of chronic tendinopathy. In a randomized, blinded, controlled trial that looked at chronic Achilles tendinopathy, de Vos and associates12 saw no benefit from PRP versus saline placebo with regard to resolution of pain or improved function at 6, 12, and 24 weeks posttreatment. Both groups improved significantly over 6 months compared with baseline, but there was no statistically significant difference between the groups with regard to the score on VISA-A (a questionnaire that assesses clinical severity of Achilles tendinopathy), patient satisfaction, or return to sports activity. A follow-up study recently reported that the lack of significant difference between the treatment groups continued through 1 year.13
The use of platelet-rich products for muscle injury has seen significantly less research than use for tendinopathic conditions. In studies of Sprague-Dawley rats with high-repetition injury of the tibialis anterior muscles, PRP treatment resulted in a faster return to full muscle contraction than did sham treatment or no treatment.14 To date, there have been no randomized human trials to investigate the merits of PRP injection for muscle injury. However, in a prospective study by Sanchez and coworkers,15 20 professional athletes with hamstring injuries experienced full recovery in half the expected recovery time without a single instance of fibrosis or reinjury.
Platelet-rich concentrates also have been studied as adjuncts to surgical procedures. Randelli and colleagues16 prospectively evaluated 14 patients undergoing rotator cuff repair who also received intraoperative PRP in combination with an autologous thrombin component after repair. In this uncontrolled study, the patients reported significant decreases in pain scores and increases in functional scores at 24 months postsurgery compared with their preoperative scores.
This pilot study set the stage for Randelli and associates17 to then develop a level 1 trial comparing activated PRP augmentation of rotator cuff repair with standard surgical repair. The PRP group experienced less early postoperative pain and better early postoperative function than the control group. However, follow-up MRI at 2 years showed no significant difference in the healing rate of the 2 groups despite a sustained significant functional improvement in PRP-treated low-grade tears.
In a separate, prospective, randomized study, Rodeo and colleagues18 used US evaluation at 6 and 12 weeks postsurgery, strength testing, and clinical rating scales to compare repair alone with repair plus platelet-rich fibrin matrix. They observed no positive effect from the fibrin matrix with regard to biological repair, function, or clinical rating.
The use of PRP during anterior cruciate ligament (ACL) reconstruction also has been evaluated. In a prospective, randomized, double-blind study, Nin and coworkers19 compared bone-patellar tendon-bone allograft reconstruction with and without the addition of a platelet-enriched gel. At 2 years, they found no clinical, radiological, or biomechanical benefit in the PRP-treated group.
In 2010, Vogrin and associates20 conducted a level 1 trial to investigate ACL reconstruction using hamstring graft and platelet gel. This study seemed to demonstrate improved anteroposterior stability in the study group at 6 months postsurgery.
Cervellin and colleagues21 cited fewer subjective reports of pain during activity at 1 year in 20 young athletes who underwent bone-patellar tendon-bone autograft and were randomized to also receive PRP gel applied to harvest sites at both proximal tibial and inferior patellar locations (sites of donor-site discomfort). They did not discover any significant differences between groups in osseous healing at either donor site.
Bone Healing
The effects of platelet concentrate in skeletal trauma management have been studied with the knowledge that in the fracture hematoma, platelets aggregate and release growth factors. Most of that research has been performed in vitro or with the animal model in an effort to simply determine whether platelet-rich products have any osteopromotive effects. There has been surprisingly little clinical research to investigate this.
In 1994, Slater and coworkers22 provided in vitro evidence that human growth factors seem to stimulate the proliferation of human osteoblast-like cells and that the cells remain differentiated as such in long-term culture. In addition, Butcher and colleagues23 showed an increased proliferation of human bone marrow stromal cells when activated PRP was combined with demineralized bone matrix and human trabecular allograft, both of which are osteoconductive graft materials.
Animal studies have demonstrated rapid healing of bone defects in PRP-treated rabbits with alloxan-induced diabetes mellitus24 and superior quality of bone healing of nonunion defects in rabbits treated with PRP and bone graft.25 In human studies, Jenis and associates26 prospectively compared PRP plus allograft with autograft in 1- and 2-level interbody spinal fusions with supplemental posterior fixation. They found the groups to be essentially equal with regard to radiographic and clinical outcomes.
In contrast, a double-blind randomized study conducted by Feiz-Erfan and colleagues27 showed no significant difference in fusion rates of PRP-augmented anterior cervical fusions using allograft bone compared with using allograft bone alone. Without supplemental bone grafting material, Mariconda and coworkers28 could not show any benefit from PRP injected into atrophic long-bone nonunions compared with a retrospective control.
Articular Cartilage
PRP has shown encouraging results as a potential conservative treatment for patients with osteoarthritis (OA). In an in vitro laboratory study, van Buul and associates29 cultured human osteoarthritic chondrocytes in the presence of interleukin-1 β (IL-1β), a potent inflammatory factor in arthritis, then introduced various concentrations of PRP supernatant. In doing so, they were able to show that PRP decreased many of the IL-1β–mediated inflammatory effects that exert themselves on human osteoarthritic chondrocytes.
In clinical studies, Sampson and colleagues30 injected osteoarthritic knees with PRP 3 separate times at 4-week intervals. Their findings demonstrated significant resolution of pain and restoration of function compared with baseline for up to 1 year after treatment in a majority of patients.
In 2009, Kon and coworkers31 injected PRP into 115 arthritic knees 3 times at 21-day intervals. Statistically significant objective and subjective improvements were noted at the end of treatment and at 6- and 12-month follow-up compared with pretreatment.
In a more recent prospective, comparative study conducted by Kon and associates,32 PRP was pitted against low- and high-molecular-weight hyaluronic acid viscosupplementation in knees that exhibited degenerative lesions, early OA, and severe OA. Improvement was noted in all treatment groups, but PRP was more effective than viscosupplemention in improving clinical and functional outcomes at 6 months postinjection in patients aged 50 years or younger. In patients older than 50 years, PRP and low-molecular-weight viscosupplementation produced equivalent beneficial results and high-molecular-weight viscosupplementation produced the worst results. The authors concluded that PRP may be a safe, viable alternative to hyaluronic acid injections.
LOOMING QUESTIONS ABOUT PRP
Perhaps the only factor to rival the potential usefulness of PRP in the orthopedic setting is the number of unknowns associated with the therapy. To date, there still is a considerable lack of high-level studies free of bias and confounding variables that produce reliable and reproducible effects of PRP on a variety of musculoskeletal conditions.
Until the basic science of PRP is better understood, engineering clinical studies to test its application will be difficult. For example, every study out-lined in this article differs with regard to such factors as centrifugation protocol, method of platelet activation, mode of delivery, number of treatments, and postapplication protocol. In addition, a lack of standardization in outcome measures causes difficulty in comparing similar trials and somewhat convolutes meta-analysis. A better understanding of the fundamentals and physiology of PRP ultimately may allow for more uniform experimental designs.
Until more progress is made, the following questions will persist:
• What exactly is the optimum PRP concentration and composition?
• Does a higher platelet concentration equal a better product or is there an inhibitory concentration that may
be counterproductive as some have proposed?33
• Is a leukocyte-rich or leukocyte-poor PRP more effective or is one better than another for specific conditions?
• What are the specific orthopedic conditions best managed with PRP and what are the proper dose, frequency, and timing of application for those conditions?
• Is endogenous or exogenous activation preferable?
• What is the best process by which to centrifuge whole blood and concentrate platelets?
• What is the most effective delivery medium and how should patients be managed or rehabilitated after treatment?
TABLE 2

Potential uses of PRP in musculoskeletal medicine
Answers to questions such as these will shed light on this potentially important treatment option. That assumes, of course, that platelet-rich products are indeed useful in managing musculoskeletal conditions.
CONCLUSION
Platelet-rich products have demonstrated great potential for use in orthopedic medicine in recent years, albeit mostly through anecdotal accounts, case reports, and lower-level studies. PRP therapy certainly may be an effective, safe, and simple solution to problems that have dogged orthopedists for years (Table 2). However, until an abundance of high-level studies can demonstrate the treatment’s effect-positive or otherwise-platelet-rich concentrates for healing should be used with a healthy level of scrutiny.
References:
REFERENCES
1. Ferrari M, Zia S, Valbonesi M, et al. A new technique for hemodilution, preparation of autologous platelet-rich plasma and intraoperative blood salvage in cardiac surgery. Int J Artif Organs. 1987;10:47-50.
2. Marx RE. Platelet-rich plasma: evidence to support its use. J Oral Maxillofac Surg. 2004;62:489-496.
3. Tamimi FM, Montalvo S, Tresguerres I, Blanco Jerez L. A comparative study of 2 methods for obtaining platelet-rich plasma. J Oral Maxillofac Surg. 2007;65:1084-1093.
4. Nagata MJ, Messora MR, Furlaneto FA, et al. Effectiveness of two methods for preparation of autologous platelet-rich plasma: an experimental study in rabbits. Eur J Dent. 2010;4:395-402.
5. Bielecki TM, Gazdzik TS, Arendt J, et al. Antibacterial effect of autologous platelet gel enriched with growth factors and other active substances: an in vitro study. J Bone Joint Surg. 2007;89B:417-420.
6. Tate KS, Crane DM. Platelet rich plasma grafts in musculoskeletal medicine. J Prolother. 2010;2:371-376.
7. Mishra A, Pavelko T. Treatment of chronic elbow tendinosis with buffered platelet-rich plasma. Am J Sports Med. 2006;34:1774-1778.
8. Peerbooms JC, Sluimer J, Bruijn DJ, Gosens T. Positive effect of an autologous platelet concentrate in lateral epicondylitis in a double-blind randomized controlled trial: platelet-rich plasma versus corticosteroid injection with a 1-year follow-up. Am J Sports Med. 2010;38:255-262.
9. Kon E, Filardo G, Delcogliano M, et al. Platelet-rich plasma: new clinical application: a pilot study for treatment of jumper’s knee. Injury. 2009;40:598-603.
10. Barrett SL, Erredge SE. Growth factors for chronic plantar fasciitis. Podiatry Today. 2004;17(11):37-42.
11. Peerbooms JC, van Laar W, Faber F, et al. Use of platelet rich plasma to treat plantar fasciitis: design of a multi centre randomized controlled trial. BMC Musculoskelet Disord. 2010;11:69.
12. de Vos RJ, Weir A, van Schie TM, et al. Platelet-rich plasma injection for chronic Achilles tendinopathy: a randomized controlled trial. JAMA. 2010;303:144-149.
13. de Jonge S, de Vos RJ, Weir A, et al. One-year follow-up of platelet-rich plasma treatment in chronic Achilles tendinopathy: a double-blind randomized placebo-controlled trial. Am J Sports Med. 2011;39:1623-1629.
14. Hammond JW, Hinton RY, Curl LA, et al. Use of autologous platelet-rich plasma to treat muscle strain injuries. Am J Sports Med. 2009;37:1135-1142.
15. Sanchez M, Anitua E, Andia I. Application of autologous growth factors on skeletal muscle healing. Presented at: 2nd World Congress on Regenerative Medicine Podium Presentations; May 2005; Leipzig, Germany.
16. Randelli PS, Arrigoni P, Cabitza P, et al. Autologous platelet rich plasma for arthroscopic rotator cuff repair: a pilot study. Disabil Rehabil. 2008;30:1584-1589.
17. Randelli P, Arrigoni P, Ragone V, et al. Platelet rich plasma in arthroscopic rotator cuff repair: a prospective RCT study, 2-year follow-up. J Shoulder Elbow Surg. 2011;20:518-528.
18. Rodeo SA, Delos D, Williams RJ 3rd, et al. The effect of platelet-rich fibrin matrix on rotator cuff tendon healing: a prospective, randomized clinical study. Presented at: American Orthopaedic Society for Sports Medicine 2011 Specialty Day; February 2011; San Diego. Paper 9624.
19. Nin JR, Gasque GM, Azcárate AV, et al. Has platelet-rich plasma any role in anterior cruciate ligament allograft healing? Arthroscopy. 2009;25:1206-1213.
20. Vogrin M, Rupreht M, Crnjac A, et al. The effect of platelet-derived growth factors on knee stability after anterior cruciate ligament reconstruction: a prospective randomized clinical study. Wien Klin Wochenschr. 2010;122(suppl 2):91-95.
21. Cervellin M, de Girolamo L, Bait C, et al. Autologous platelet-rich plasma gel to reduce donor-site morbidity after patellar tendon graft harvesting for anterior cruciate ligament reconstruction: a randomized, controlled clinical study. Knee Surg Sports Traumatol Arthrosc. 2012;20:114-120.
22. Slater M, Patava J, Kingham K, Mason RS. InvolveÂment of platelets in stimulating osteogenic activity. J Orthop Res. 1995;13:655-663.
23. Butcher A, Milner R, Ellis K, et al. Interaction of platelet-rich concentrate with bone graft materials: an in vitro study. J Orthop Trauma. 2009;23:195-202.
24. Rezaie A, Mousavi G, Mohajeri D, et al. Effect of autogenous platelet-rich plasma (PRP) on femoral cancellous bone defect healing in Alloxan-induced diabetic rabbits. Aust J Basic Appl Sci. 2011;5:800-808.
25. Kanthan SR, Kavitha G, Addi S, et al. Platelet-rich plasma (PRP) enhances bone healing in non-united critical-sized defects: a preliminary study involving rabbit models. Injury. 2011;42:782-789.
26. Jenis LG, Banco RJ, Kwon B. A prospective study of Autologous Growth Factors (AGF) in lumbar interbody fusion. Spine J. 2006;6:14-20.
27. Feiz-Erfan I, Harrigan M, Sonntag VK, Harrington TR. Effect of autologous platelet gel on early and late graft fusion in anterior cervical spine surgery. J NeuroÂsurg Spine. 2007;7:496-502.
28. Mariconda M, Cozzolino F, Cozzolino A, et al. Platelet gel supplementation in long bone nonunions treated by external fixation. J Orthop Trauma. 2008;22:342-345.
29. van Buul GM, Koevoet WL, Kops N, et al. Platelet-rich plasma releasate inhibits inflammatory processes in osteoarthritic chondrocytes. Am J Sports Med. 2011;39:2362-2370.
30. Sampson S, Reed M, Silvers H, et al. Injection of platelet-rich plasma in patients with primary and secondary knee osteoarthritis: a pilot study. Am J Phys Med Rehabil. 2010;89:961-969.
31. Kon E, Buda R, Filardo G, et al. Platelet-rich plasma: intra-articular knee injections produced favorable results on degenerative cartilage lesions. Knee Surg Sports Traumatol Arthrosc. 2010;18:472-479.
32. Kon E, Mandelbaum B, Buda R, et al. Platelet-rich plasma intra-articular injection versus hyaluronic acid viscosupplementation as treatments for cartilage pathology: from early degeneration to osteoarthritis. Arthroscopy. 2011;27:1490-1501.
33. Weibrich G, Hansen T, Kleis W, et al. Effect of platelet concentration in platelet-rich plasma on peri-implant bone regeneration. Bone. 2004;34:665-671.
34. Platelet Rich Plasma (PRP) Guidelines. International Cellular Medicine Society. 2011. http://www.cellmedicinesociety.org/attachments/370_Section%2010%20-%20Platelet%20Rich%20Plasma%20%28PRP%29%20Guidelines.pdf. Accessed April 12, 2012.