The primary care physician's guide to inflammatory arthritis: Treatment
Primary care physicians and rheumatologists may comanage the inflammatory arthritides to effectively control them and their comorbidities.
Rheumatoid arthritis (RA), ankylosing spondylitis (AS), and psoriatic arthritis (PsA) are the most common inflammatory arthritides and present physicians with a major challenge in diagnosis as well as in treatment. Recent advances, particularly the arrival of the biologic agents, may help prevent the joint destruction and physical disability of the comorbidities often associated with these conditions and, possibly, reduce their burden,1,2 but early disease recognition by primary care physicians is needed, along with referral to a rheumatologist for definitive treatment. Primary care physicians and rheumatologists then may work together in comanagement of the inflammatory arthritides for effective control of these diseases and their comorbidities.
This 2-part article provides primary care physicians with practical information about the diagnosis and management of the inflammatory arthritides. In the first part (“The primary care physician's guide to inflammatory arthritis: Diagnosis,” The Journal of Musculoskeletal Medicine, June 2010, page 223), we addressed the clinical presentation and diagnosis of these conditions. This second part describes the latest treatments.
Rheumatoid arthritis
The use of disease-modifying antirheumatic drugs (DMARDs) in the treatment of patients with RA has improved outcomes significantly.3 Methotrexate (MTX), used widely to manage RA since the 1980s, now is considered the cornerstone of DMARD therapy for RA.4 Numerous clinical studies support the use of combination therapy that includes MTX. Other DMARDs used to manage RA are hydroxychloroquine (HCQ), sulfasalazine (SSZ), and leflunomide.
Corticosteroid therapy may be used in the management of RA in a number of ways. Low-dose corticosteroids (10 mg/d or less) are used frequently as adjunctive therapy to DMARDs in RA management. In fact, corticosteroids have some DMARD activity in RA. They also may be used to quickly reduce pain and stiffness and improve function so that a patient can continue to work or care for his or her children. In these situations, corticosteroids act as a “bridge” therapy while slower-acting DMARD therapy is instituted. In addition, corticosteroids may be used locally in the form of joint injections for isolated joints with active disease in an otherwise stable patient with RA.
The American College of Rheumatology recommends a chest radiograph to establish a baseline and a complete blood cell count, a complete metabolic profile, and hepatitis serologies for baseline levels before the start of therapy. An eye examination also is recommended if HCQ is part of the treatment regimen. Combination DMARD therapy using MTX, SSZ, HCQ, and prednisolone was more effective than monotherapy in achieving remission.5 The effectiveness of leflunomide for RA is similar to that of MTX.
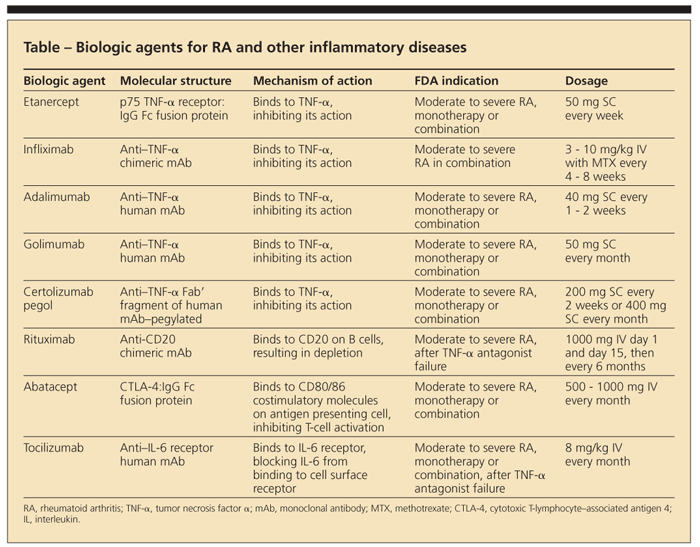
Tumor necrosis factor α (TNF-α) antagonists and other biologic agents have revolutionized the treatment of patients with RA as well as other rheumatologic conditions (Table).3 To date, 5 TNF-α antagonists-etanercept, infliximab, adalimumab, golimumab, and certolizumab pegol-have been approved by the FDA for the management of moderate to severe RA. These agents inhibit the action of TNF-α, a proinflammatory cytokine important in the pathogenesis of RA and other chronic inflammatory diseases.
Combination therapy with a TNF-α antagonist and MTX in patients with early RA was associated with significantly higher rates of remission and less radiographic progression at 54 weeks than was MTX monotherapy.6 Another study showed that initial combination therapy that included either prednisone or infliximab resulted in earlier functional improvement and less radiographic damage after 1 year than did sequential monotherapy or step-up combination therapy.7
Three other biologic agents have FDA approval for the treatment of patients with RA, each with a different mechanism of action.3 They are the following:
•Rituximab, an anti-CD20 monoclonal antibody that depletes blood B cells, is used in patients with RA in whom treatment with TNF-α antagonists has not been successful.
•Abatacept, a costimulation modulator that inhibits T-cell activation, may be used alone or in combination with MTX.
•Tocilizumab, an anti–interleukin-6 receptor monoclonal antibody, is the newest agent approved for the treatment of patients with RA.
All biologic agents are associated with significant toxicity as well as an increased risk of infections. In addition, TNF-α antagonists increase the risk of reactivation of latent tuberculosis and systemic fungal infections. Before treatment with biologic agents is begun, all patients should be screened for latent tuberculosis, hepatitis B and C, and HIV infection.
Ankylosing spondylitis
NSAIDs and cyclooxygenase-2 selective inhibitors are effective in controlling inflammatory symptoms of AS and may have DMARD activity. Other conventional DMARDs, including MTX, SSZ, and leflunomide, are not effective. TNF-α antagonists, including etanercept, infliximab, adalimumab, and golimumab, are FDA-approved for the treatment of patients with AS and indicated for patients in whom NSAID therapy has been unsuccessful.8 These agents may have disease-modifying activity as assessed by serial MRI of the spine.
Low-dose corticosteroids work less well in AS than in RA. Local corticosteroid injections may be helpful in sacroiliac joints or, occasionally, in peripheral joints. Topical corticosteroids are used frequently for ocular involvement, in the form of acute anterior uveitis.
Psoriatic arthritis
NSAIDs are useful in controlling inflammatory symptoms in milder forms of PsA. Unlike AS, PsA may be managed with conventional DMARDs, such as SSZ (no effect on skin disease), MTX, and leflunomide. The TNF-α antagonists, including etanercept, infliximab, adalimumab, and golimumab, are effective and FDA-approved for the management of both dermatological and articular manifestations of PsA and have disease-modifying activity on articular disease.9,10
Low-dose corticosteroids are used occasionally as adjunctive therapy in PsA, but they are not as effective as in RA. Topical corticosteroids are used frequently for ocular involvement, in the form of uveitis, which in PsA often is chronic and bilateral.
References:
References
1. Bergman MJ. Social and economic impact of inflammatory arthritis. Postgrad Med. 2006;Spec No:5-11.
2. Coordinating Center for Health Promotion. Targeting Arthritis: Reducing Disability for 46 Million Americans 2008. Atlanta: Centers for Disease Control and Prevention, US Dept of Health and Human Services; 2008.
3. van Vollenhoven RF. Treatment of rheumatoid arthritis: state of the art 2009. Nat Rev Rheumatol. 2009;5:531-541.
4. Visser K, Katchamart W, Loza E, et al. Multinational evidence-based recommendations for the use of methotrexate in rheumatic disorders with a focus on rheumatoid arthritis: integrating systematic literature research and expert opinion of a broad international panel of rheumatologists in the 3E Initiative. Ann Rheum Dis. 2009;68:1086-1093.
5. Möttönen T, Hannonen P, Leirisalo-Repo M, et al. Comparison of combination therapy with single-drug therapy in early rheumatoid arthritis: a randomised trial. FIN-RACo trial group. Lancet. 1999;353:1568-1573.
6. St Clair EW, van der Heijde DM, Smolen JS, et al; Active-Controlled Study of Patients Receiving Infliximab for the Treatment of Rheumatoid Arthritis of Early Onset Study Group. Combination of infliximab and methotrexate therapy for early rheumatoid arthritis: a randomized, controlled trial. Arthritis Rheum. 2004; 50:3432-3443.
7. Goekoop-Ruiterman YP, de Vries-Bouwstra JK, Allaart CF, et al. Clinical and radiographic outcomes of four different treatment strategies in patients with early rheumatoid arthritis (the BeSt study): a randomized, controlled trial. Arthritis Rheum. 2005;52:3381-3390.
8. Zochling J, van der Heijde D, Burgos-Vargas R, et al; ASsessment in AS international working group; European League Against Rheumatism. ASAS/EULAR recommendations for the management of ankylosing spondylitis. Ann Rheum Dis. 2006;65:442-452.
9. Gladman DD. Psoriatic arthritis. Dermatol Ther. 2009;22:40-55.
10. Ritchlin CT, Kavanaugh A, Gladman DD, et al; Group for Research and Assessment of Psoriasis and Psoriatic Arthritis (GRAPPA). Treatment recommendations for psoriatic arthritis. Ann Rheum Dis. 2009;68:1387-1394.