Researchers Discover Molecular Changes Responsible for Skin Discoloration in Psoriasis
Many control psoriasis-ridden skin only to find traces of discolored patches in its wake. A study by the Milstein Medical Research Program at The Rockefeller University has uncovered the correlation between skin discoloration and psoriasis, providing opportunities of treatment for pigmentation changes within eczema and acne as well.
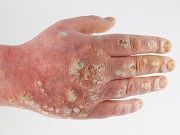
Many control psoriasis-ridden skin only to find traces of discolored patches in its wake. A study by the Milstein Medical Research Program at The Rockefeller University has uncovered the correlation between skin discoloration and psoriasis, providing opportunities of treatment for pigmentation changes within eczema and acne as well.
Research has demonstrated that a class of immune system molecules known as cytokines is associated with a variety of inflammatory skin processes. Cytokines are integral in a signaling process passing immune cells to fight off an infection. However, two cytokines — interleukin-17 (IL-17) and tumor necrosis factor (TNF) — are abundant in psoriasis, causing the immune system to attack the patient’s own skin cells. Although several studies have shown that IL-17 and TNF are behind the rash-like symptoms of psoriasis, Clair Q. Wang, PhD, a research associate in the Laboratory of Investigative Dermatology at the Rockefeller University in New York, and colleagues wanted to investigate whether these two molecules were responsible for the skin discoloration commonly observed in patients with psoriasis.
Light therapy is a common treatment for this persistent, chronic disease. Wang said in a news release that “Patients will receive artificial UVA and UVB light as a way to reduce inflammation, and although the light doesn’t cause sunburn, it was still commonly assumed that this was causing the pigmentation changes. Our research showed that this was not the case.”
IL-17 and TNF reportedly interfere with the production of melanocytes — cells that produce the pigment for skin colors. According to Wang, "Melanocytes are believed to only replicate in the initial growth stage of melanocyte tumors, including melanomas. Here, in psoriasis, their numbers were doubled, sometimes tripled, but this was noncancerous skin. This shows us that these cells are not as dormant in healthy individuals as scientists believe."
This discovery has provided scientists with a better grasp on what can happen to a patient’s skin following a psoriasis flare-up. “During a flare-up, there can be parts of skin with hypopigmentation — white spots,” said Wang. But findings indicate when the flare-up subsides, cells are then pushed toward the surface causing dark marks to appear. Wang noted, “We think the increase in IL-17 and TNF induces this build-up of melanocytes, but prevents them from expressing the melanin until the inflammation settles down. Then the build-up is released, and the skin shows hyperpigmentation — dark spots.”
“Knowing that immune cytokines can change pigment production in melanocytes, while also knowing that chronic inflammation has the potential to increase the number of melanocytes, has clear implications for the design of future therapies to address a set of common skin disorders,” said James Krueger, MD, PhD, director of the Milstein Medical Research Program at the Rockefeller University.