What Is the Best Technique for Total Hip Replacement?
Most surgeons agree that recovery and survivorship after total hip replacement may be linked to various implant's characteristics, especially fixation technique and bearing surface type.
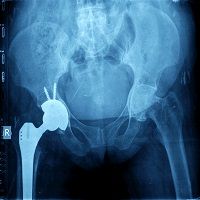
Surgeons perform more than 300,000 total hip replacement (THR) surgeries annually and most are wildly successful. Patients report greater mobility and improved quality of life. Surgical approaches are constantly changing to improve outcomes. Most surgeons agree that survivorship may be linked to various implant's characteristics, especially THR fixation technique and bearing surface type.
JAMA Surgery published a study in its October 2015 issue that looks at THR in France's entire population and compares THR short-term survivorship according to cement type and bearing surface.
The researchers used data from the French national health insurance system to identify 100,191 patients aged 40 years or older who had THR surgery between April 1, 2010 and December 31, 2011 for arthritis. They noted cement type and bearing surface employed in the surgery. They followed this patient through December 31, 2013. They looked for indications that patients had required revision, including any surgical reintervention to change or remove the implant or any of its components.
The average patient age was about 70, and 57% of patients were women. During the median 33-month follow-up period, 3142 individuals underwent prosthetic revision.
Patients who had THR with antibiotic-impregnated cement experienced significantly better early prognosis in than those who had uncemented THR. Cumulative revision rates were 2.4% and 3.3%, respectively. This held true regardless of bearing surface and prosthetic revision risk factors, particularly in women.
Patients who had both-sides cemented and hybrid THRs had similar survivorship patterns, a finding the authors attributed to cementing of the femoral stem.
The authors found that younger patients had shorter THR survivorship.
Although no overall association between bearing surface and THR revision was found, patients who had metal-on-metal THRs had slightly higher revision risk than those who had metal-on-polyethylene THRs.
The authors conclude that these findings can help surgeons select a THR fixation technique and may inform the decision-making process for patients and surgeons.