What Pay for Performance Means for Musculoskeletal Medicine
ABSTRACT: Pay for performance (P4P) is causing physicians to examine how they provide care individually and collectively within local health systems. It is the most recent attempt by Medicare and commercial payers to reduce the cost and improve the outcomes of health care. Understanding P4P and deciding how to manage the multiple programs being implemented by payers will challenge physicians' ethics and practice resources. Improving health care for musculoskeletal diseases will require cooperation among the specialties that share responsibility for this care and improved methods for coordinating and documenting it. (J Musculoskel Med. 2009;26:207-212)
Pay for performance (P4P)-the most recent attempt by Medicare and commercial payers to reduce the cost of health care and, perhaps, improve outcomes-is causing physicians to examine how care is provided individually and collectively within local health systems. They will need to understand P4P and decide how to manage the multiple programs that payers are implementing without sacrificing their ethics. Cooperation among the specialties that share responsibility for musculoskeletal care and improved methods for coordinating and documenting it will be required to enhance management of musculoskeletal diseases.
The Centers for Medicare & Medicaid Services (CMS) has been implementing its Physician Quality Reporting Initiative (PQRI) since 2007, and private insurance companies are using P4P programs increasingly to adjust payments to providers. These P4P initiatives are using a growing list of consensus performance measures approved by various organizations that apply to virtually every aspect of health care and every medical and surgical specialty.1
In September 2008, Dr Allan Gibofsky and I explored ". . . whether P4P programs will be designed to provide benefits to patients and reward providers for improving efficiency and outcomes, or will they be aimed exclusively at controlling payer costs . . ." in an Arthritis Care and Research editorial, "Pay for performance in rheumatology: Will we get the carrot or the stick?"2 We provided a background about P4P, issues involved in implementing P4P programs, and the possible benefits of well-designed programs. Many medical specialty societies have developed Web sites that explain the PQRI for their members.3-6
In this article, I provide a perspective on quality measures development, the implications of P4P for musculoskeletal disease management, and thoughts about how physicians might prepare for and respond to this growing reality. My opinions are based on my recent work on the American College of Rheumatology (ACR) Quality Measures Subcommittee, my long-term musculoskeletal disease practice improvement research, and experiences from my own and my colleagues' practices. Although primary care physicians and orthopedic surgeons, rheumatologists, and other specialists who manage musculoskeletal diseases will have access to information from their own specialty societies, in reality we will share common disease-based performance measures and accountability for treatment of shared patients, as my discussion will illustrate.
Will it be the carrot or the stick?
The answer is still up in the air, but CMS and commercial insurers are going forward with largely untested P4P programs that suggest the latter and are changing them annually or more often. Payer-based P4P may be joining the growing list of initiatives that have failed to slow the growth of US health care spending: managed care; precertifications for treatments, diagnostic testing, and procedures; and patient copayments.7
Important problems with P4P have not been resolved, such as which physicians will be held accountable for which measures for which patients ("attribution"). In addition, programs are being implemented without clear benchmarks for performance, cost accountability, or feasibility testing. The similarities among multiple payers' precertification and P4P programs are not coincidental, and any delay in approving care or P4P payment penalty is money in the payers' pockets at the patients' and providers' expense.
Private insurers also are using their P4P programs to compete against one another for purchasers' business and, more recently, for gaining a role in managing national health care reform. Their interests go beyond reducing health care payments to deciding what is paid for, and they are asserting a responsibility for ensuring the quality and safety of their clients' care independent of those who provide it. Pharmacy benefit organizations demanding pretreatment tuberculosis skin test results before filling or renewing biologic drug prescriptions is but one example of this trend. In addition, a competition is emerging over who will be paid to gather practices' clinical data into large data repositories to assess provider performance. In all these respects, P4P is becoming one more aspect of the health system's "zero sum game" competition in which stakeholders are competing against one another for money, while physicians and patients are being reduced to pawns in this high-stakes game.8
Health care quality is a rapidly growing industry
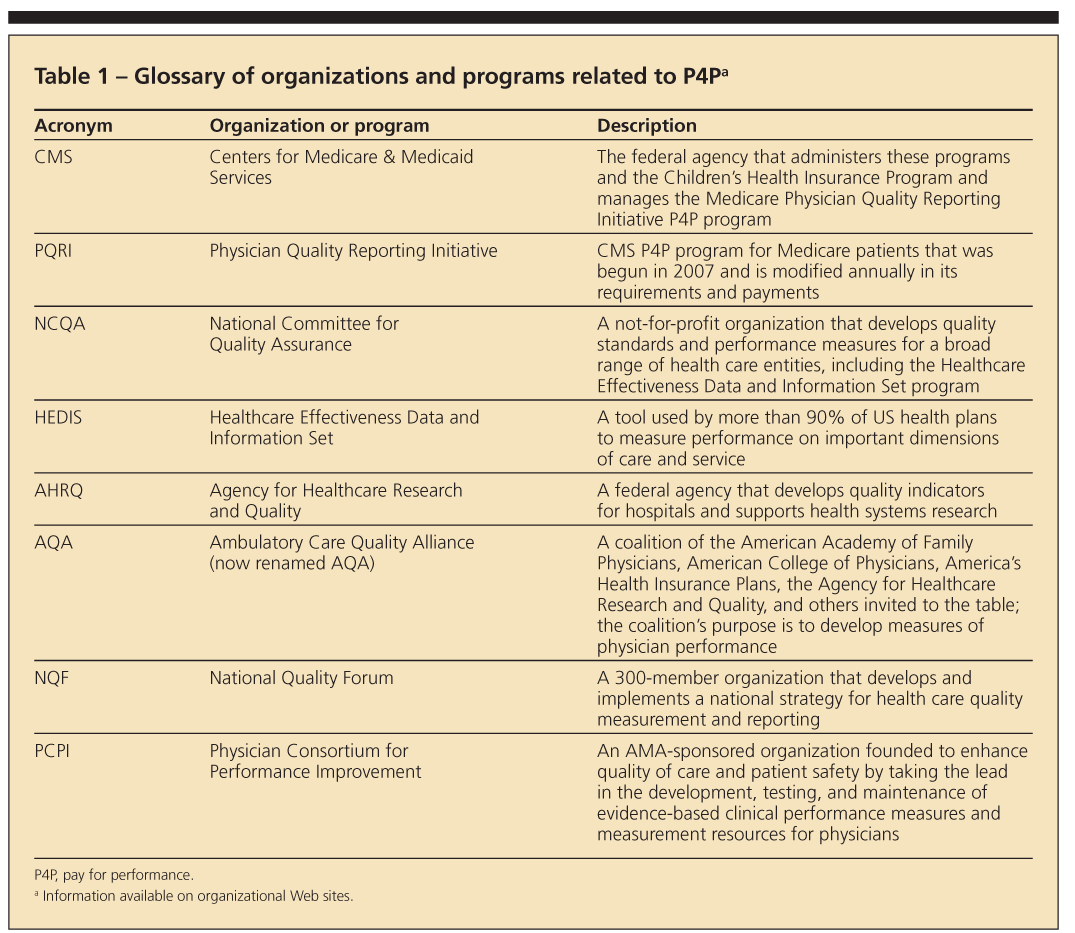
A complex fabric of organizations is involved in proposing, finalizing, and certifying quality measures. Any discussion of this topic rapidly degenerates into an alphanumerical code that empowers bureaucrats and befuddles physicians. A glossary of P4P organizations and programs is provided in Table 1.
These organizations' stated goals are to publish consensus measures for a wide spectrum of diseases. How the measures are then used to evaluate physician performance and modify reimbursement is left to whoever chooses to use them for whatever purpose.
The players are consortia of all imaginable health care stakeholders-medical societies, specialty organizations, insurers, licensing and certification boards, purchasers, patient advocates, the federal government, and others. Their roles are evolving and in many cases appear to be duplicative or competitive, creating an off-budget burden of additional health care costs. Of greatest concern, from my perspective, is that most of them include CMS and the insurance industry, which seem to have secured greater influence in the process than those who provide and receive care.
An example will illustrate why physicians should be concerned. The ACR Quality Measures Subcommittee I serve on agreed on criteria for developing rheumatic disease measures, including that they be evidence-based, focused on improving quality of care, and possible for clinical practices to implement. Our strategy was to start simple with the expectation that all could and would participate and then to grow the scope of the process.

Our proposed rheumatoid arthritis (RA) measures were posted on the ACR Web site (Table 2).9 They were then reviewed and modified by other committees within the ACR before being whisked through the alphabet soup of organizations and published to meet the PQRI deadline for 2009 (Table 3).1
The final product included more measures and different ones with purposes different from what the ACR subcommittee had envisioned. A few appear to be difficult to document in real-world health care. Most disturbing to us, our third measure, which recommended treatment acceleration for uncontrolled RA, was replaced with one requiring assessment of disease prognosis, a recognized aspect of insurers' biologic drug precertification requirements. These and other measures related to other diseases are being incorporated into private payer–based P4P programs rapidly without feasibility testing.

P4P in musculoskeletal disease care
Chronic diseases, including musculoskeletal conditions, consume 70% of US health care dollars.10 They often are being managed inefficiently and ineffectively, making them prime targets for P4P.
Some chronic disease measures apply to one specialty and may be satisfied by individual physicians and specialty practices. More often, however, providing and documenting high-value care for patients with these diseases-eg, RA, gout, osteoporosis, osteoarthritis, and back pain-has been shown to require cooperation and communication among multiple physicians over time, because primary care physicians and specialists manage various aspects of each patient's disease and comorbidities. In health systems that lack these synergies, attribution is a problem for P4P-which physician treating each patient with each disease is to be held responsible for meeting that patient's quality measures.
Osteoporosis management provides a good example. Quality measures that have been certified for Medicare's P4P program mandate bone density measurement for women older than 65 years and for patients with fragility fractures.1 Primary care physicians, medical specialists, and orthopedic surgeons all are likely to be held accountable; however, none can do the job alone, in contrast to system-level osteoporosis care programs.11,12 In many health systems, competition among specialties for dual-energy x-ray absorptiometry revenues and control of treatment precludes this level of care13; single specialty programs, such as the ACR's, the American Orthopaedic Association's "Own the Bone," and the primary care "Patient Centered Medical Home," are well-intentioned but not up to the task at hand.
The inflammatory arthritides present equally daunting but different challenges. Early RA diagnosis and treatment often is compromised within primary care by insufficient evaluation, inappropriate laboratory testing, and delayed referral to rheumatology.14 Reactive arthritis often is misdiagnosed because primary care physicians or orthopedic surgeons did not perform synovial fluid analysis on joint effusions before providing expensive MRI scanning and arthroscopic surgery for presumptive internal derangements. Ankylosing spondylitis diagnosis is similarly delayed by failure across primary care to ask a few simple but specific questions that distinguish patients with inflammatory, infectious, and malignant diseases from the thundering herd presenting with mechanical back pain. At the same time, orthopedic surgeons are flooded with unnecessary referrals for self-limited back pain.
So who will be held accountable for improving the quality and cost of care for patients with these diseases? Access to the best specialty care for each patient must be achieved through defining each specialty's roles within health systems, ensuring that the skills to perform them are learned, and then using specialty preappointment management or musculoskeletal disease triage or both to facilitate timely and effective care by the best-qualified providers.15
Emerging P4P realities, as I see them
•The demands from government and private purchasers on CMS and commercial payers to slow escalating health insurance premiums have made cost control their highest priority. P4P is driven by the consensus that further cost increases are unacceptable and that rewarding physicians for volume of services independent of value cannot continue. Physicians must respect this but also recognize that there are fundamental differences between their goals and ours and that P4P is being implemented with too little concern about its impact on practice work and patient care.16
•Ignoring P4P will not be an option for physicians, practices, and health systems because incentives and penalties simply will be ratcheted up until the gains or pains command a response. Physicians must recognize their contributions to health care ineffectiveness, cost overruns, and waste.10,17 Taking back leadership of P4P is required to address improving care and reducing costs in their patients', society's, and their own interests. Physicians need to change fundamentally how they provide care and do business. If they fail to do this, the door will stay open for others to assert their entitlement to do so, contrary to physicians' best interests and professional ethics.
•Physicians do not have the time or practice resources to service the growing number of complex, variable payer-initiated precertification and P4P programs. They divert our attention from providing necessary care. CMS has acknowledged this in its 2009 program by limiting quality measurement reporting to retrospective chart review of small samples of consecutive patients and by providing several reporting options.1 This and other insurers' approaches are not scalable in the context of traditional delivery of care and medical recordkeeping. Much of the information being requested is not routinely collected or requires time-consuming record review, and the variance among programs' expectations precludes meeting them efficiently, if at all.
Where to turn for help?
Specialty societies are the best hope for developing quality measures and uniform reporting processes that balance improving patient care and reducing cost. However, they must recognize that the quality movement is off the track and move to represent patients' and practicing physicians' interests. Those whose members specialize in musculoskeletal diseases must coordinate their efforts in support of system-level care and P4P reporting.
Quality measures programs in practices, in systems, and on the national level initially must focus on implementing a few important feasible measures, while longer-term goals need to target fundamental process redesigns and outcomes improvements-an approach that is consistent with proven change management methods.18-20 Physicians must support their specialty society programs and be prepared to tell insurers when they cannot meet unreasonable precertification and P4P expectations. Insurers must be convinced to use uniform specialty P4P reports rather than insist that individual physicians provide variable patient and disease population data to each of their programs that often relate to only a small portion of patients being treated.
Most important for musculoskeletal care, in my opinion, is physician cooperation at the local health system level to integrate care and reduce costs. Without this, there will be nothing to report but more bad news. Critical aspects will include adopting evidence-based guidelines and clinically important measures of quality, shifting to standardized clinical data collection by disease that documents performance measures proactively, and implementing the needed practice and system process changes to reduce variance across practices and specialties. Again, physicians must share attribution at the system level by reporting their disease populations' quality measures rather than agreeing to insurance companies assigning them to individual providers.
Where should we start?
•Become engaged. Recent community practice members' comments on the ACR advocacy Web site about payer influence on the ACR's quality program produced a change in the ACR leadership's views. This critical input from the trenches needs to continue. Rheumatologists need to implement the ACR's Rheumatology Clinical Registry, which will be released this year, and other specialists need to adopt their own societies' P4P reporting programs.
•Make a commitment to measurement in your practice. Physicians seldom measure their clinical processes and patient outcomes. What they do not measure, they do not know and cannot improve. The absence of clinical data monitoring causes physicians to consistently overestimate their performance and their patients' disease status.21
•Develop and maintain disease registries. The term "registry" means different things to different health care stakeholders, but in the P4P context, registries are lists of patients a practice is treating currently for each disease. This information will be needed to counter payers' billing-derived incorrect attributions of patients who are others' responsibility.
•Learn the Plan-Do-Study-Act (PDSA) improvement methods.19 PDSA methods are an approach to achieving continuous improvement of complex processes, such as delivery of health care, that depend on multiple small tests of change. They are used widely in other industries and have produced dramatic improvements in practices and health systems as well. These methods will be needed to change practice processes without compromising productivity or effectiveness.
•Begin focusing on practice value (quality + access/cost) in addition to profitability. Physicians cannot allow near-term revenues to trump their making changes required for longer-term success. They must improve measurable quality and access to care and lower their cost or others will lower cost without regard for quality. Physicians need to shift coordination of care from physician office visits to computer-assisted team approaches that increase patient throughput at a lower cost and focus physicians' efforts more on problem solving. Standardizing clinical data collection, organization, and analysis for established patients also is critical.19,22 Preappointment management by consultants is another requirement, given that many re-ferrals are inappropriate, unnecessary, or duplicative.15
•Define what your practice is able and ethically willing to do in response to payers' demands. Be willing to say no. Servicing unreasonable and abusive requests is "death by a thousand cuts." Now I am more frequently responding, "I have the information, but I do not have the time or resources to supply it."
Conclusions
P4P must reward documented quality and efficiency rather than impose unrealistic expectations that delay necessary care and reduce provider reimbursement. Specialty societies need to develop measures and reporting processes, cooperatively when necessary, and advocate for all payers using this standardized information for their P4P programs. Specialties providing musculoskeletal disease care need to work together within health systems to provide and document effectiveness and efficiency. Compensation plans within physician organizations need to include performance measures. Business as usual is no longer an option.
References:
References1. Centers for Medicare & Medicaid Services. Physician Quality Reporting Initiative. 2009. http://www.cms.hhs.gov/pqri/. Accessed May 11, 2009.
2. Gibofsky A, Harrington JT Jr. Pay for performance in rheumatology: will we get the carrot or the stick? Arthritis Rheum. 2008;59:1203-1206.
3. American Academy of Orthopaedic Surgeons. Physician Quality Reporting Initiative (PQRI) Information. 2009. http://www.aaos.org/research/committee/
evidence/PQRI_info.asp. Accessed May 11, 2009.
4. American Board of Family Medicine. ABFM Continues as PQRI Registry Participant. 2009. http://www.annfammed.org/cgi/content/full/7/2/185/. Accessed May 11, 2009.
5. American College of Physicians. PQRI Coding Tool Instructions. 2009. http://www.acponline.org/running_practice/quality_improvement/performance_measurement/pqri/. Accessed May 11, 2009.
6. American College of Rheumatology. PQRI. 2009. http://www.rheumatology.org/practice/pqri/measures_index.asp/. Accessed May 11, 2009.
7. Rosenthal MB, Dudley RA. Pay-for-performance: will the latest payment trend improve care? JAMA. 2007;297:740-744.
8. Porter ME, Teisberg EO. Redefining Health Care: Creating Value-Based Competition on Results. Boston: Harvard Business School Press; 2006.
9. American College of Rheumatology. Quality Measures, Quality of Care, Rheumatoid Arthritis. 2009. http://www.rheumatology.org/practice/qmc/RA.asp. Accessed April 24, 2009.
10. Institute of Medicine. Committee on Quality of Health Care in America. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, DC: National Academy Press; 2001.
11. Harrington JT, Lease J. Osteoporosis disease management for fragility fracture patients: new understandings based on three years' experience with an osteoporosis care service. Arthritis Rheum. 2007;57:1502-1506.
12. Dell R, Greene D, Schelkun SR, Williams K. Osteoporosis disease management: the role of the orthopaedic surgeon. J Bone Joint Surg. 2008;90A(suppl 4):S188-S194.
13. Porter ME, Teisberg EO. How physicians can change the future of health care. JAMA. 2007;297:1103-1111.
14. Graydon SL, Thompson AE. Triage of referrals to an outpatient rheumatology clinic: analysis of referral information and triage. J Rheumatol. 2008;35:1378-1383.
15. Harrington JT, Walsh MB. Pre-appointment management of new patient referrals in rheumatology: a key strategy for improving health care delivery. Arthritis Rheum. 2001;45:295-300.
16. Wharam JF, Sulmasy D. Improving the quality of health care: who is responsible for what? JAMA. 2009;301:215-217.
17. McGlynn EA, Asch SM, Adams J, et al. The quality of health care delivered to adults in the United States. N Engl J Med. 2003;348:2635-2645.
18. Berwick DM. Developing and testing changes in delivery of care. Ann Intern Med. 1998;128:651-656.
19. Harrington JT, Newman ED. Redesigning the care of rheumatic diseases at the practice and system levels, part 1: practice level process improvement (Redesign 101). Clin Exp Rheumatol. 2007;25(suppl 47):S55-S63.
20. Newman ED, Harrington JT. Redesigning the care of rheumatic diseases at the practice and system levels, part 2: system level process improvement (Redesign 201). Clin Exp Rheumatol. 2007;25(suppl 47):S64-S68.
21. Phillips LS, Twombly JG. It's time to overcome clinical inertia. Ann Intern Med. 2008;148:783-785.
22. Morris AH. Developing and implementing computerized protocols for standardization of clinical decisions. Ann Intern Med. 2000;132:373-383.