Auto-Injectors: Doctors, Patients, Need More Instruction in Use
People most at risk of needing adrenaline auto-injectors tend not to know how to use them properly, studies have found. Physicians are blamed for the lapses.
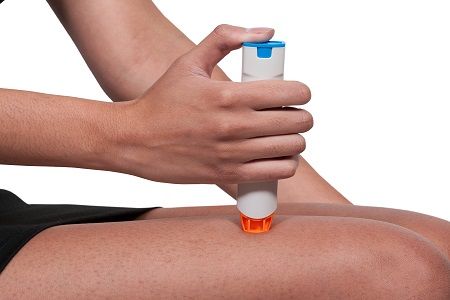
There are lots of reasons people do not use their adrenaline auto-injectors properly, a new meta-analysis concluded. Lack of instruction leads the list.
Writing in the journal Allergy researchers in Germany said they found that certain barriers work together to systematically impede the proper use of adrenaline auto-injectors (AAIs) by people at risk of anaphylaxis.
“Although recommended by international guidelines and expert groups, the use of AAIs for emergency first-line treatment of anaphylaxis is not often performed,” wrote the authors of the study, a trio of researchers from the universities of Washington and Tennessee as well as Universitätsmedizin in Berlin.
“There is a need to educate clinicians and patients on the life-saving potential of self-injectable adrenaline,” they wrote.
Unfortunately, the doctors who treat anaphylaxis most frequently have proven very resistant to education about the need for AAIs, the study authors noted.
In the United States, one cohort study published in the Annals of Allergy Asthma and Immunology found that only 36.6% patients who went to emergency departments with anaphylaxis left the hospital with prescriptions for AAIs. Other studies have found similar figures.
Even when patients do receive AAI prescriptions, they often fail to carry the devices with them. A number of studies conducted in both the US and Europe have consistently found that less than half of all people who are prescribed AAIs actually have them at all times. Some put the number below 30%.
Patients who carry their AAIs, moreover, struggle to remember when and how to use them.
Indeed, a pair of studies published in the Journal of Clinical Immunology found that only 22% of patients who had suffered anaphylaxis from bee stings knew to use their AAI if they sustained another sting and that only 44% of people with AAIs could demonstrate their proper use.
The authors of the meta-study also noted that research has consistently found an alarming shortage of AAIs in public places, devices needed to treat people who had never suffered a severe allergy before and thus have no reason to carry a personal AAI.
Studies from the US do show improvements at schools, an important venue, but most districts have yet to buy enough devices or train enough people to use them properly, recent research concludes.
As for guidelines that encourage restaurants and large gathering spots (such as concert venues and sports arenas) to stock AAIs, studies find that they are generally ignored.
The meta-study team found a serious need for improvement across the board, especially among emergency treatment providers and patients who know themselves to be at risk.
“There is a particular need for clinicians to learn to recognize at-risk patients, in order to provide them with AAIs and for patients to appreciate the vital importance of always carrying AAIs with them and being prepared to use them without delay at the first sign of anaphylaxis,” they wrote.
And that need increases every day, the study authors noted, because the incidence of anaphylaxis appears to be rising rapidly.
In the US, a nationwide survey of emergency department visits between 1993 and 2004 found that cases of anaphylaxis requiring hospitalization jumped more than four-fold during the study period, from one per 100,000 people per year to 4.7 per 100,000 people per year.
The study, "Anaphylaxis treatment: current barriers to adrenalineauto-injector use," appeared in Allergy.
Related Coverage:
Needles Are Dangerously Long in Kids' Auto-Injectors, Study Finds
Auto Injectors Using New Technology to Help Allergy Patients
Epinephrine Autoinjector Needles May Be Too Short to Be Effective in Obese Patients