Correlation Identified Between ABO Blood Types, Acne Severity
Recent data highlighted the relationship between different blood types and acne severity, identifying correlations between specific groups.
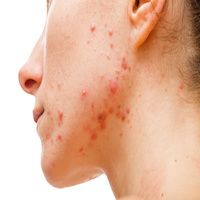
Researchers identified a significant correlation between ABO blood-type groups and severity of acne, according to recent findings.1
The genetic transfer of blood groups may impact development of some conditions, and the ABO antigenic system is widely believed to play a role in disease pathogenesis, along with TNF-α and other kinds of pro-inflammatory molecules.
Elevated TNF-α levels have been associated with inflammation, which is considered an etiopathogenic factor in the development of acne vulgaris, and some studies have examined the connection between blood group and acne vulgaris.2
The findings of prior studies have been conflicting, however, hence the purpose of this study. The research was authored by Neşe Göçer Gürok, MD, from Fethi Sekin City Hospital in Turkey.
“Possible correlations were investigated in diseases such as rosacea, lichen planus, skin cancer, vitiligo, pemphigus, and psoriasis in dermatology,” Gürok and colleagues wrote. “Also recently, the correlation between acne vulgaris and blood group was investigated but contradictory findings were reported. In this study aimed to investigate the correlation between acne vulgaris severity and ABO blood groups.”
Background and Findings
The investigators carried out their research with 380 participants aged between the ages of 18 and 65 who had been diagnosed with acne vulgaris through clinical examination at the Dermatology Clinic at Health Sciences University, Elazig Fethi Sekin City Hospital between 2019 and 2022.
The research team also used a healthy control group made up of 1000 participants in the same age bracket who had been to the hospital for check-up appointments or health reports.
The researchers found that 263 of 380 in the former group reported mild acne vulgaris and 117 reported the more severe condition of acne vulgaris. The participants included did not have dermatological comorbidities or systemic diseases such as cardiovascular diseases, drug abuse history, or cancers.
The investigators also analyzed severity of acne vulgaris through the global acne-grading system (GAGS)—a tool used routinely in this particular clinic—measuring severity based upon both the blood group and Rh factor values visible through patient files.
Overall, the team concluded that the acne vulgaris arm showed a higher proportion of females and a lower mean age compared to the control arm. Additionally, the data showed that participants with severe acne were younger on average than those reporting mild acne.
The investigators noted that among participants with blood type A, severe acne incidence was found to be higher compared to both those with mild acne and those in the control group. That being said, they added that mild acne was more common in the other blood type groups compared to the control arm.
Lastly, they concluded that there was not a substantial difference for the Rh blood groups between participants with either type of acne or those in the control arm.
“The expression of A blood type antigens, which was reported to be significantly higher in the present study, especially in severe acne patients, could contribute to the etiopathogenesis of acne vulgaris and alleviate acne severity via follicular hyperkeratinization,” they wrote. “Further studies that would be conducted with larger samples in different centers could confirm the current study findings.”
References
- Gürok, NG. The correlation between ABO blood types and acne vulgaris severity. J Cosmet Dermatol. 2023; 00: 1- 6. doi:10.1111/jocd.15698.
- Terzi E, Türsen B, Dursun P, Erdem T, Türsen Ü. The Relationship between ABO Blood Groups and Acne Vulgaris. Saudi J Med Med Sci. 2016 Jan-Apr;4(1):26-28. doi: 10.4103/1658-631X.170886. Epub 2015 Dec 2. PMID: 30787691; PMCID: PMC6298270.