Elevated Blood Biomarker Levels Can Detect Suicide Risk
Though patients may not disclose suicidal thoughts and behaviors to their physicians, their blood test results can be dead giveaways.

Though patients may not disclose suicidal thoughts and behaviors to their physicians, their blood test results can be dead giveaways, according to new research findings published in the Aug. 20 advance online edition of Molecular Psychiatry.
For their “Discovery and Validation of Blood Biomarkers for Suicidality” study, Alexander B. Niculescu III, MD, PhD, an associate professor of psychiatry and medical neuroscience at the Indiana University School of Medicine in Indianapolis, and colleagues conducted analyses on blood samples from male patients with bipolar disorder — one in three of whom will attempt to commit suicide during his lifetime, according to previous research. The investigators then derived and studied blood biomarker data from participants who reported dramatic changes from no suicidal ideation to strong suicidal ideation between blood testing visits.
After those genetic and genomic evaluations, the authors identified spermidine/spermine N1—acetyltransferase 1 (SAT1), phosphatase and tensin homolog (PTEN), myristoylated alanine-rich protein kinase C substrate (MARCKS), and mitogen-activated protein kinase kinase kinase 3 (MAP3K3) as the strongest blood biomarkers associated with suicidal thoughts. (Figure)
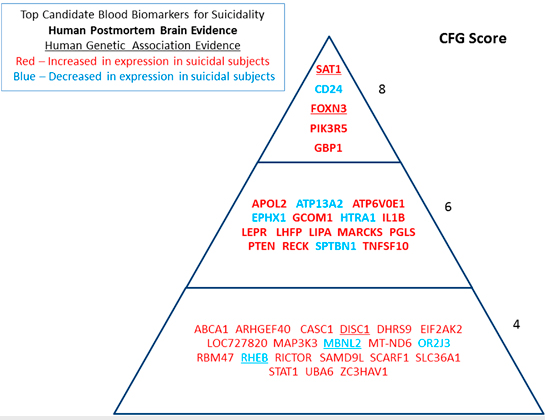
To validate that correlation, the researchers compared the bipolar patients’ gene expression data to live cohorts of bipolar and schizophrenic subjects and blood samples collected from a postmortem cohort of male patients who had committed suicide. At the conclusion of those follow-up analyses, the investigators found that all of the suicide completers had elevated SAT1 gene expression levels. Additionally, high blood levels of SAT1, PTEN, MARCKS, and MAP3K3 were linked to past and future hospitalizations related to suicide in the bipolar and schizophrenic groups — suggesting the four biomarkers “might be not only state markers, but perhaps trait markers, as well,” the authors wrote.
“Taken together, our results have implications for the understanding of suicide, as well as for the development of objective laboratory tests and tools to track suicidal risk and response to treatment,” the authors concluded. “Given the fact that approximately 1 million people die of suicide worldwide each year — and this is a potentially preventable cause of death — the need for, urgency, and importance of efforts such as ours cannot be overstated.”
To learn more about the researchers’ findings, watch Niculescu discuss the study in this video clip from the IU School of Medicine.