International Federation of Psoriasis Associations Publishes Issue Brief to Raise Awareness of Psoriatic Arthritis
Early diagnosis and treatment is the key to preventing long-term joint damage in patients with psoriatic arthritis.
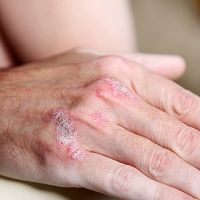
The International Federation of Psoriasis Associations (IFPA) recently published an issue brief to “raise attention to the need for global awareness of psoriatic arthritis and its impact on individuals and society.”
A news release announcing the publication noted that “Despite being the second most common inflammatory joint disease, causing stiffness, swelling and pain in and around the joints and can lead to extensive erosive and deforming joint damage, many are unaware of the burden psoriatic arthritis puts on both the individual and society. Many people who suffer from psoriatic arthritis are unable to work due to this disabling condition and require frequent and expensive treatments. If nothing changes, the burden that psoriatic arthritis puts on both the individual and society will remain high in terms of healthcare costs, lost productivity and inability to participate fully and equally in society.”
A copy of the 4-page document can be downloaded here.
According to the issue brief, psoriatic arthritis (PsA) imposes a heavy burden on patients and their families. More than 50 percent of people with psoriatic arthritis develop additional comorbid conditions “that can have a significant negative impact on health and quality of life,” including cardiovascular disease, metabolic syndrome, obesity, diabetes, fatty liver disease, Crohn’s disease, ophthalmic disease, depression and anxiety.
Despite this, nearly 50 percent of psoriasis patients have undiagnosed psoriatic arthritis, and nearly 60 percent of those who have been diagnosed with psoriatic arthritis do not receive treatment. According to the IFPA, “A lack of diagnosis and treatment can have tremendous negative effects, as studies show that as short a delay as six months from symptom onset to the first visit with a rheumatologist can result in irreversible joint damage and a poor prognosis.”
To improve early diagnosis and reduce the undertreatment of PsA, dermatologists and primary care physicians should be able to recognize PsA and its symptoms, “as they are most likely to meet patients with PsA early in the course of the disease.”
The IFPA issue brief concludes by calling on patients, providers, advocacy groups, and the community to:
- Recognize that psoriatic arthritis is a serious disabling disease with a major impact on the individual as well as on society
- Include psoriatic arthritis in health policies and disability forums
- Support awareness campaigns to educate patients and health care professionals about psoriatic arthritis to ensure early diagnosis and effective treatment