Iron, Skin, and Wound Healing
In the future, topical chelators and novel agents will be available to improve wound healing in patients with iron aberrations or inflammatory states.
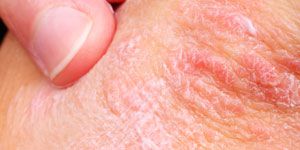
Healthy skin, mucous membranes, hair, and nails need adequate iron. When patients are iron-deficient, their pallor, fragile or concave nails, and brittle hair are clinical clues. They also tend to suffer as the deficiency magnifies with itching, skin infection (impetigo, boils and candidiasis), and inflammation at the corners of the mouth, according to a new article discussing iron’s role in the skin in Frontiers in Pharmacology.
Iron is the most common element on Earth, and iron proteins are found in all living organisms. Regardless of its abundance, iron’s physiologic role in human health is still not clearly understood. Elevated iron levels in macrophages can induce unrestrained proinflammatory macrophage activation.
Within the epidermis and dermis, iron concentrations vary considerably as do its oxidative states (Fe2+, Fe3+). We know that the skin is critical to iron homeostatis because iron is not excreted actively in physiologic processes, but rather lost primarily through skin desquamation. Iron is more heavily concentrated in sun-exposed areas, and some of its oxidative states interact with reactive oxygen species to slow free radical damage.
This article highlights iron’s role as a potential therapeutic target in the skin. In the future, topical chelators and novel agents will be available to improve wound healing in patients with iron aberrations or inflammatory states.
The authors cover iron’s known roles in several processes, as well as recent experimental findings concerning anemia and blood volume’s impact on wound healing. They also discuss 2 conditions — rheumatoid arthritis and lupus erythematosus — that are associated with dysregulation of local cutaneous iron homeostasis.
In terms of wound healing, both inadequate and overabundant iron affects the process. Older studies looked at iron with a focus on wound-strengths. More recent work looks more closely at macroscopic health and re-epithelialization. Iron deficiency without inflammation probably undermines skin remodeling. Iron deficiency with inflammation can increase macrophage iron and serve as an inflammatory galvanizer. In both cases, it’s critical to treat the underlying causes of iron dysfunction.
No article on iron would be complete without a discussion of local cutaneous depositions, and the authors cover iron overload in good detail. In patients who have hereditary hemochromatosis, skin iron levels rise as iron overload increases. The authors note that clinically, some physicians are using quantitative nuclear microscopy to decide when to start, change or stop phlebotomy therapy.
