Kids Develop Allergies as Poor Lifestyle Bystanders
Whether it's food or environment-related, there are all different types of allergies. The latest developments in pediatric allergy research highlights peanut allergy, skin prick test measures, and tobacco-induced allergy.
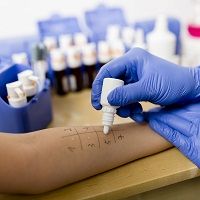
Whether it’s food or environment-related, there are all different types of allergies. The latest developments in pediatric allergy research highlights peanut allergy, skin prick test measures, and tobacco-induced allergy.
John M. Kelso, MD, FACAAI, from Scripps Clinic in San Diego, California, illustrated the clinical implications during a presentation at the 2015 American College of Allergy, Asthma, and Immunology Annual Scientific Meeting (ACAAI 2015) in San Antonio, Texas.
It’s been determined that there is an association between atopic dermatitis and food allergy during infancy. But what is that relationship exactly and which one causes the other? As it turns out, exposure to peanut antigen in dust can trigger a peanut allergy. Kelso referenced a study which included 359 infants less than 15 months of age without a known peanut allergy. They all either had a milk or egg allergy, or, moderate to severe atopic dermatitis and positive skin test to milk, eggs, or both.
Environmental peanut exposure (EPE) was quantified from dust collected from the families’ living room floors (yes, seriously). The practice proved to be adequate because it revealed some interesting outcomes. For each 4-unit logâ‚‚ (16-fold) increase in EPE, there is an increased risk of peanut skin prick test (SPT) sensitization — defined as 3 mm or greater. There was also an increased likelihood of a peanut allergy which indicated that the children were sensitized by household exposure. However, the association does not stand true in children without atopic dermatitis, only in those with a history of condition. Therefore, eczema in infancy “clearly increases the risk of developing peanut sensitization and allergy,” as Kelso explained. He noted that there was no connection between filaggrin (FLG) mutations and peanut allergy. Aggressive treatment of atopic dermatitis may help prevent the food allergy.
Another part of Kelso’s presentation brought focus to the importance of adjusting for histamine activity in SPT. For the most part, SPT results are reported as mean wheal diameter — with a larger skin test meaning a higher level of allergy. However, there are two methods for SPT where one includes histamine response as a reference and the other does not.
So two trials from Berlin and Sweden, including 39 patients ages 15 to 50, set out to get to the bottom of histamine activity. All of the participants were clinically allergic to grass and were not taking antihistamines. The team estimated the biological activity of the same batch of a reference Timothy Grass Pollen Extract. The estimated amount of allergen in the extract was 15 times higher in the Berlin study than in the Swedish one. However, the histamine wheal sizes were smaller in the Berlin cohort.
The outcomes revealed some important clinical implications. A similar sized wheal on two individuals does not mean that they have the same level of allergy. This understanding carries over to say that two people with different wheal sizes could still have the same level of allergy. Therefore, histamine control size should be taken into consideration when interpreting a skin prick test.
Lifestyle choices have the power to greatly influence our health. Tobacco smoke has been associated with asthma, however, its influence on allergies have not be studied well. It’s estimated that 11% of all children in the United States are exposed to environmental tobacco smoke (ETS) on a regular basis, and a new analysis found that those children are more likely to develop allergies.
The researchers reviewed eight studies totaling 2,603 children and another 9,230 participants from six different studies (all ages 0 to 18) to determine the effects of ETS exposure on immunoglobulin E (IgE) and allergen specific IgE. IgE is a type of antibody that plays a major role in allergic diseases. In the study, childhood ETS exposure proved to raise total serum IgE (tIgE) concentration by 27.7 IU/mL. Tobacco exposure also increased the risk of showing a positive SPT for allergy. So add this to the list of why tobacco is better thrown in the garbage.
Developments on the treatment side of allergies are crucial, but identifying the factors that play a role in the onset serve as key points of prevention.