Melanoma Patients Experience Delays in Surgery
A recent study looked specifically at patients on Medicare who require surgery for their melanoma and their wait time before going under the knife.
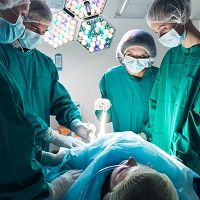
A recent study looked specifically at patients on Medicare who require surgery for their melanoma and their wait time before going under the knife.
According to results published in the Journal of the American Medical Association, nearly one quarter of Medicare patients experience delayed procedures of more than a month and a half due to several factors.
The study looked at Medicare patients who were diagnosed with melanoma between January 2000 and December 31, 2009. The data was collected using Medicare’s Surveillance, Epidemiology, and End Results database and included “all patients undergoing surgical excision of melanoma diagnosed by means of results of skin biopsy.”
The total patient pool included 32,501 cases of melanoma. An overwhelming 95.4% were Caucasian and 63.1% were male. Of the total group, 47.9% were married and 60.8% were at least 75-years-old. The authors also noted at 93.7% had no prior history of melanoma. Just over 40% of the patients were diagnosed with melanomas located on their head and neck area, and 48.2% were staged as in situ disease.
The authors also found 77% had excision surgery performed within the first month and a half after diagnosis. Just over 8% of all patients observed exhibited a delay longer than 3 months during their course of treatment. They also reported the delay of longer than a month and a half, “was significantly increased among patients 85 years or older compared with those younger than 65 years (odds ratio [OR], 1.28 [95% CL, 1.05-1.55]; P - .02).”
Another contributing factor, according to the authors, was the actual excision administrator. They reported the lowest likelihood of delay with a probability of just 16% when dermatologists treated patients. Whereas, when someone other than a dermatologist performed the biopsy and a primary care doctor performed the excision, the likelihood of delay increased to a probability closer to 31%.
When looking at the treatment of melanoma, the authors realized delaying excision could contribute to other issues for patients. In addition to increasing concerns about morbidity and mortality and the development of other more serious conditions, the authors said delays could also be psychologically taxing. “Surgical delay may cause anxiety, stress, and psychological harm,” they said.
“In addition, surgical delay may reflect limited access to health care and/or inefficient delivery of health care,” they said.
“Our results show that a delay of surgery for melanoma may be relatively common among Medicare beneficiaries,” the authors added. “Although no gold standard exists to judge appropriate vs. inappropriate surgical delay, minimization of delay is an important patient centered objective of high-quality dermatologic care, especially given the potential harms of psychological stress associated with untreated malignant neoplasms.”
