Persistent Thumb Lesion in a Middle-aged Man
A 57-year-old man presented to clinic with this persistent skin lesion on his thumb. Three months ago, he lanced the lesion, producing some purulence and blood. Since then, it has bled almost daily and has not healed. He was treated with silver nitrate by another clinician after one month, but the lesion persists. His past medical history is significant for diabetes and his family history is significant for 2 cousins with melanoma.
a) Amelanotic melanoma
b) Hematoma
c) Cherry angioma
d) Janeway lesion
e) Pyogenic granuloma
Diagnosis
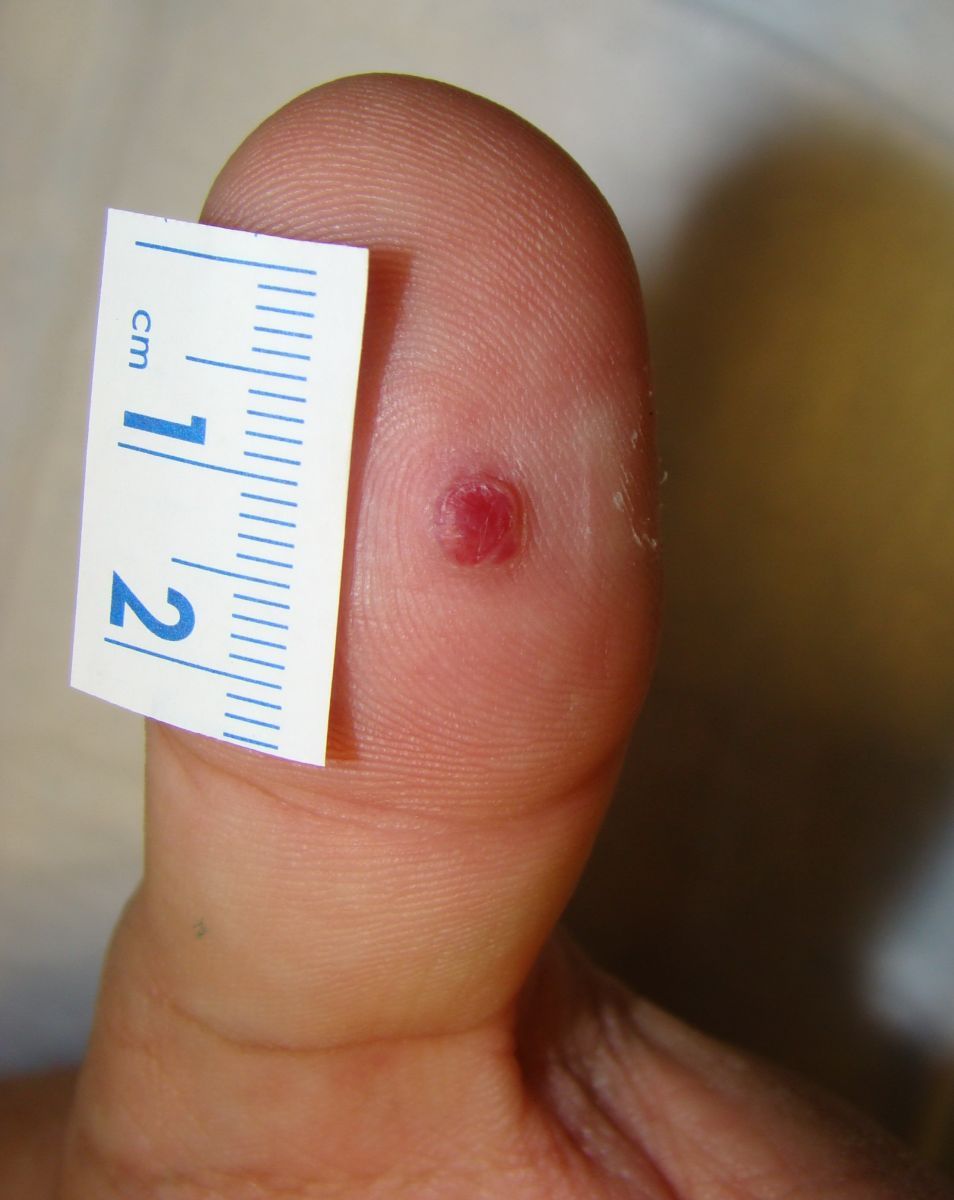
This man has a pyogenic granuloma, also known as a lobular capillary hemangioma. This relatively common lesion occurs as a result of injury or inflammation consistent with this patient's history. It typically presents as a non-healing, easily bleeding, moist, fleshy lesion. Histologically, there is a lobular proliferation of capillaries, and frequently, there is a circumferential epidermal collaret around the lesion.
Some clinicians consider excision with suture closure to be the gold standard in treatment when it is clinically appropriate, with a lesion recurrence rate of 5%. On the other hand, locally destructive treatment may be less invasive and has a recurrence rate of 10%, although there is wide variation in study results.1
This man's lesion was shaved off to confirm the pathology, and the base was treated with 2 cycles of curettage and electrocautery. It was healing well at follow-up by phone one week later.
Amelanotic melanoma, or skin cancer without the typical hyperpigmentation, can present with similar findings of a non-healing, bleeding, erythematous lesion. Thus, it is prudent to send tissue for pathology when treating a pyogenic granuloma, because a positive family history of melanoma increases the risk and consideration of melanoma.
A hematoma, which is also called a blood blister, can occur with pinch injuries on the digits. The initial presentation would appear similar to this man's lesion, but over time, it would darken and spontaneously resolve.
Janeway lesions present as erythematous, non-blanching lesions of the hands and feet due to the showering of bacterial emboli in endocarditis.2 However, this patient had no fevers, chills, or other systemic symptoms that are usually present in endocarditis.
References
1. Giblin AV, Clover AJ, Athanassopoulos A, Budny PG. Pyogenic granuloma - the quest for optimum treatment: audit of treatment of 408 cases. J Plast Reconstr Aesthet Surg. 2007 May 2;60(9):1030-5. http://www.sciencedirect.com/science/article/pii/S1748681507001088.
2. Patel LM, Lambert PJ, Gagna CE, Maghari A, Lambert WC. Cutaneous signs of systemic disease. Clin Dermatol. 2011 Sep-Oct;29(5):511-22. http://www.ncbi.nlm.nih.gov/pubmed/21855727.
About the Authors

Daniel Stulberg, MD, is a Professor of Family and Community Medicine at the University of New Mexico. After completing his training at the University of Michigan, he worked in private practice in rural Arizona before moving into full-time teaching. Stulberg has published multiple articles and presented at many national conferences regarding skin care and treatment. He continues to practice the full spectrum of family medicine with an emphasis on dermatology and procedures.
