Surgery Can Manage Fibrous Dysplasia of the Proximal Femur
Results show that blade plates or intramedullary nails placed via surgery can be effective treatments for patients with fibrous dysplasia of the proximal femur.
Results from a study recently published in the Orphanet Journal of Rare Diseases show that blade plates or intramedullary nails placed via surgery can be effective treatments for patients with fibrous dysplasia of the proximal femur.
Fibrous dysplasia is a rare bone disorder that is genetic and non-inheritable. It is characterized by a post-zygotic activating mutation of the GNAS gene, which decreases GTPase activity of the stimulatory G-protein (Gsα). This mutation causes an increase in intracellular levels of cAMP in bone forming cells, which causes deformity, pathological fractures, and clinical manifestations of pain due to local replacement of lamellar bone with ill-woven, under mineralized (fibrous) tissue of poor quality in affected parts of the skeleton.
Most often, proximal femur and craniofacial bones are affected.
The study enrolled 32 patients from the Netherlands and Austria who were treated with surgical intervention using either an angled blade plate (n = 27) or an intramedullary nail (n = 5) between 1985 and 2015 and who had a follow-up of at least 1 year post surgery.
The primary outcome was successful completion of the surgery according to the revised Henderson classification. Secondary outcomes included pain and change in femoral neck-shaft angle over time; these were assessed at 1 year and at the end of the follow-up. The revision-free survival rate acted as the primary measure.
According to the results, after a median follow-up of 4.1 years, the revision-free survival rate was 72% with revision being necessary in 7 patients due to an angled blade plate-induced iliotibial tract pain and 2 patients for structural failure due to a fracture distal to an angled blade plate. However, 91% of all patients experienced good walking ability and were pain free at the end of the follow-up. Additionally, no patients experienced significant postoperative change in femoral neck shaft angle.
In addition, it was noted that more challenges exist for surgery regarding the proximal femur in pediatric fibrous dysplasia patients as growth of the bone has to be considered and allocated for.
Based off the data, a patient-tailored algorithm for the surgical management of fibrous dysplasia of the proximal femur was proposed. The algorithm is represented in the figure below. (photo cred: Orphanet)
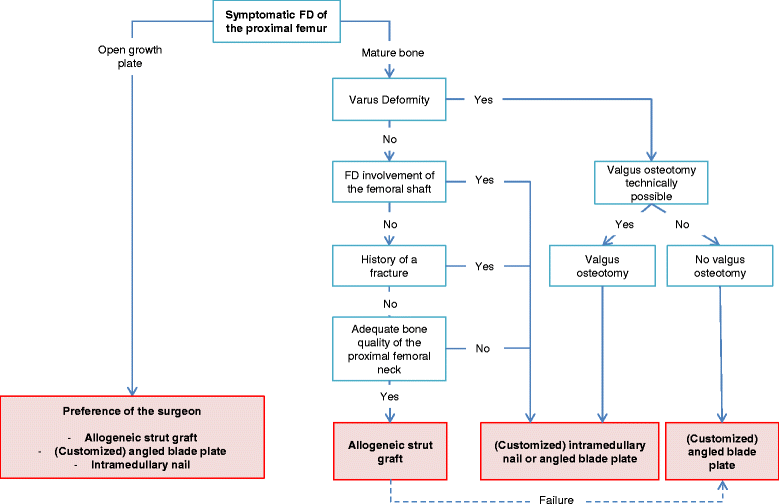
In the algorithm, there is a spot for allogeneic strut grafting that is limited to cases without a previous fracture; without a fibrous dysplasia lesion extending to the femoral shaft; without a deformity of the femur requiring a valgus osteotomy; and with adequate bone-stock proximally in the femoral neck.
A revision surgery with an angled blade plate is preferred over the placement of an intramedullary nail in the case of failure of the allogeneic strut graft since the introduction of a blade is easier to perform in a femoral neck with remnants of strut grafts. In patients with risk
factors associated with the placing of an allogeneic strut graft, internal fixation with either an intramedullary nail or an angled blade plate is preferred. The fibrous dysplasia lesion being completely bridged especially in the femoral head, with adequate, bipolar fixation of the implant ends in healthy bone with either the blade of the angled blade plate or the screw of the intramedullary nail is of the upmost importance when using either of these devices.
To prevent the development of complaints of the iliotibial tract, angled blade plates should also be adequately submerged into the cortex. A customized blade plate is the implant of choice in the case of severe deformity of the femur without the possibility of a valgus osteotomy. In fibrous dysplasia of the proximal femur, the use of dynamic or compression hip screws and TENs is not recommended.
For more from the rare disease community, follow Rare Disease Report on Facebook and Twitter.