Vaccine Hesitancy Differs for COVID-19, Flu Shots
Data from a nationally representative survey show that, despite most US adults agree the COVID-19 and flu vaccines are safe and effective, there is discrepancy in why some may not want one or the other.
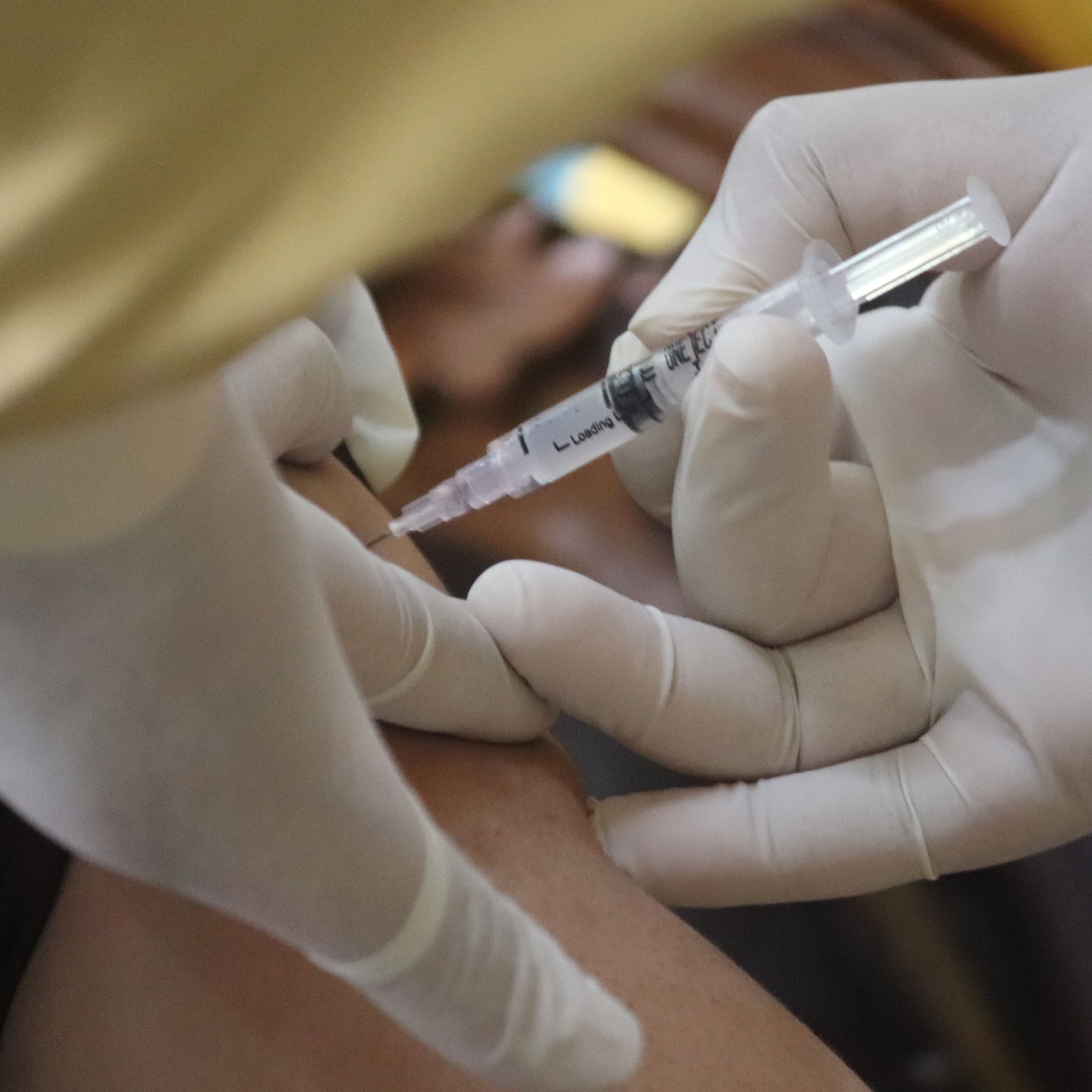
US adults are less likely to receive a COVID-19 vaccine than influenza vaccine this season, according to data from a nationally representative survey. Chief among the reasons given for COVID-19 vaccine hesitancy among adults remains an expressed wish for “more clinical research” as well as concerns over the vaccines’ safety versus the annual flu shot—despite a similar rate of adults stating they believe either vaccine is efficacious for preventing the viruses.1
A team of US-based investigators reported survey findings in a new research letter that which showed a greater national distrust of COVID-19 vaccine benefit-risk profiles compared to that of flu vaccines, despite robust data showing the former may be more efficacious and similarly safe to the latter. Led by Gillian K. SteelFisher, PhD, MSc, and Mary G. Findling, PhD, ScM, of the department of Health Policy and Management at Harvard T.H. Chan School of Public Health, investigators believe the data show a need for more nuanced—and disease-specific—approaches to vaccine education by clinicians.
SteelFisher, Findling and colleagues sought to examine the attitudes toward COVID-19 and flu vaccination through a survey study regarding the now seasonal tendencies of US adults with available booster doses for both viruses. They hoped their research would elucidate guidance for programmatic and policy-related decisions going forward.
“As the viral landscape shifts, there is new urgency to understand US adults’ views on relevant vaccines, including whether they perceive annual vaccines similarly, or whether there are differences that may impact coadministration and communications,” they noted.
Public health-related research in recent years has additionally observed a “spillover” effect of increasing overall vaccine hesitancy for other diseases, such as human papillomavirus (HPV) and hepatitis B virus (HBV), in the wake of the rapid development of COVID-19 vaccines.2
The Harvard team’s analysis included findings from a nationally representative, probability-based survey sample of US adults aged ≥18 years old, conducted from July 7 – 16 of this year. Respondents were prompted to provide their attitudes toward the effectiveness and safety of COVId-19 and flu vaccines, their own intentions with vaccination opportunities, and any major reasons they may have for hesitancy to receive such a vaccine. Investigators assessed data for both all adults and those aged ≥50 years old, who may have higher risk of severe illness due to the flu or COVID-19.1
The final analysis included 1430 respondents. Adults primarily believed COVID-19 vaccines and flu vaccines were “very effective” (42% and 40%, respectively), followed by “somewhat effective (28% and 38%, respectively). Just 20% of respondents believed COVID-19 vaccines were “not too effective” or “not at all effective”; even fewer (11%) believed so for the flu vaccine.
Similarly, a majority of respondents believed COVID-19 vaccines were “very safe” or “somewhat safe” (70%); even more believed so for flu vaccines (74%). Despite this, only 54% and 64% of respondents were somewhat or very likely to get the COVID-19 or flu vaccination this season.
Rationale for vaccine hesitancy varied significantly among adults were not likely to get the COVID-19 or flu vaccines. Among those against the COVID-19 vaccine, the most commonly reported reasons included the following:
- Wanting to see more research done on the updated vaccine (60%)
- Worried about the safety of the updated vaccine (51%)
- Distrust of government agencies that which promote the updated vaccine (45%)
- Disbelief an updated vaccine would be effective in protecting against the virus (40%)
Among those against the flu vaccine, the most commonly reported reasons included the following:
- A preference to attempt to receive natural immunity from infection (37%)
- A feeling the people are expected to get too many vaccines in general (30%)
- Distrust of government agencies that which promote the updated vaccine (27%)
- Disbelief an updated vaccine would be effective in protecting against the virus (27%)
“Results were similar among adults aged 50 years and older,” investigators noted. “Subanalyses by degrees of hesitancy (somewhat, not too, and not at all likely) show that many differences in reasons for hesitation held along the continuum, with greater proportions having concerns about COVID-19 vaccines at each degree of hesitancy.”
The team concluded that health care providers should expected a limited demand for COVID-19 vaccines, and only moderate interest in the annual flu shot. “Where coadministration is offered, communications should lead with the more popular influenza vaccine, provide consistent messaging on safety and effectiveness of both vaccines, and address vaccine-specific beliefs, such as the limits of protection from prior COVID-19 infection,” they wrote.
They additionally stressed the importance of public health agencies and leaders working collaboratively with trusted messengers in community settings to help foster better trust in vaccines and their supporting clinical data. “Vaccine hesitancy in the US is not monolithic, and it is essential that health professionals and communicators address nuances in public opinion to promote vaccine uptake this season and beyond,” they concluded.
Reference
- SteelFisher GK, Findling MG, Caporello HL, McGowan E, Espino L, Sutton J. Divergent Attitudes Toward COVID-19 Vaccine vs Influenza Vaccine. JAMA Netw Open. 2023;6(12):e2349881. doi:10.1001/jamanetworkopen.2023.49881
- Kunzmann K. Research Explores Link Between COVID-19 Vaccine Hesitancy and HBV, HPV Uptake. HCPLive. Published August 22, 2023. https://www.hcplive.com/view/research-link-covid-19-vaccine-hesitancy-hbv-hpv-uptake