Facial Rash in an Elderly Woman
This 70-year-old woman was referred for this waxing and waning erythematous facial rash of two years duration. She has tried topical metronidazole and clindamycin without improvement. Her past medical history is significant for hypertension and hypothyroidism, otherwise she is in good health and a review of systems is negative except for the itching facial rash.
This 70-year-old woman was referred for this waxing and waning erythematous facial rash of two years duration. She has tried topical metronidazole and clindamycin without improvement. Her past medical history is significant for hypertension and hypothyroidism, otherwise she is in good health and a review of systems is negative except for the itching facial rash.
What is your diagnosis?
a) Lupus Erythematosus
b) Methicillin-resistant staph aureus infection (MRSA)c) Sarcoidosisd) Polymorphous light eruption (PMLE)
e) Rosacea
Diagnosis
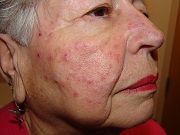
Rosacea has four subtypes, this patient has type 2 (Papulopustular rosacea.) It is characterized by erythematous papules or pustules of the mid-face including the cheeks nose and sometimes the chin and forehead. The etiology is uncertain; it may be inflammatory due to the presence of bacteria or Demodex folliculorum mites.
The erythema is exacerbated by vasodilation that can be caused from heat, exercise, alcohol, spicy foods etc. Rosacea occurs in both men and women, usually after age 30. Type 1 is erythematotelangiectatic, type 3 is phymomatous (as in rhinophyma) and type 4 is granulomatous.[i]
This patient did not respond to topical metronidazole which is appropriate first-line therapy as is topical azelaic acid. She was treated with oral tetracycline 500 mg BID and was clear of lesions at 3 months.
MRSA can present as single or multiple abscesses or ulcerations. Oral drugs of choice for cutaneous MRSA include trimethoprim sulfamethoxazole, clindamycin and doxycycline. The chronicity and waxing/waning nature of this patient's rash point away from an acute bacterial infection.
Cutaneous Lupus Erythematosus (CLE) presents as erythematous papules and plaques on sun exposed skin including the face. This patient had a negative anti-nuclear antibody test for lupus. CLE is treated with topical steroids, topical calcineurin inhibitors, or systemic medications as needed.[ii]
Sarcoidosis is a granulomatous disease that can present with a myriad of cutaneous findings. Erythematous papules, plaques or nodules which can occur throughout the body are the most common findings in contrast to this patient's localized facial findings.[iii]
Polymorphous light eruption (PMLE) causes papules, vesicles and plaques with delayed onset in sun exposed areas. This patient does not have the typical pattern or history of onset of rash following episodes of sun exposure.[iv]
References
2014 Jan-Feb;32(1):24-34.
Dermatol Online J. 2014 Jan;5(1):7-13
Dermatol. 2012 May;66(5):699.e1-18
Photomed. 2008 Jun;24(3):155-61.
About the Author

Daniel Stulberg, MD, is a Professor of Family and Community Medicine at the University of New Mexico. After completing his training at the University of Michigan, he worked in private practice in rural Arizona before moving into full-time teaching. Stulberg has published multiple articles and presented at many national conferences regarding skin care and treatment. He continues to practice the full spectrum of family medicine with an emphasis on dermatology and procedures.
