Federal Funding in Pain Research Falls, But Project Pipeline Grows
Though the total National Institutes of Health (NIH) budget has stayed flat over the past several years, chronic pain research has enjoyed an expanded slice of the federal funding pie, as dollars committed to that portion of science grew from $279 million in 2008 to $396 million in 2012.

Though the total National Institutes of Health (NIH) budget has stayed flat over the past several years, chronic pain research has enjoyed an expanded slice of the federal funding pie, as dollars committed to that portion of science grew from $279 million in 2008 to $396 million in 2012. But in her keynote address to the 32nd Annual Scientific Meeting of the American Pain Society, Story Landis, PhD, director of the National Institute for Neurological Disorders and Stroke (NINDS), said federal cuts resulting from the sequester will shave off approximately 5.7 percent of the NIH’s fiscal-year 2013 budget and decrease this year’s chronic pain research funding in turn.
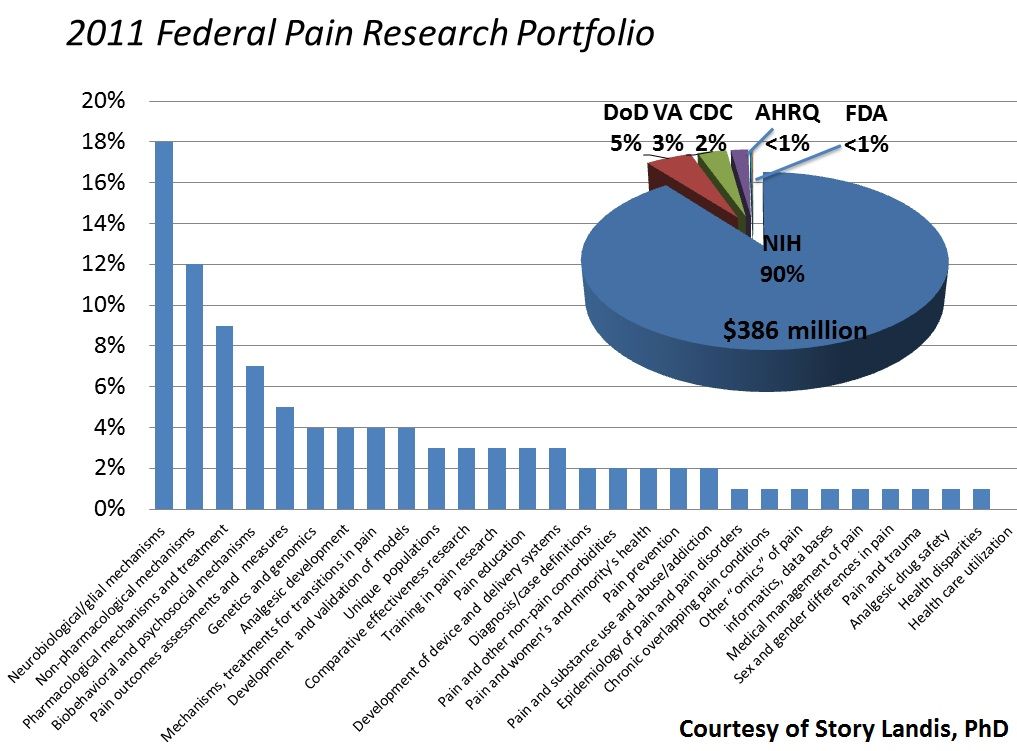
However, despite a smaller national government budget, Landis said the NINDS — the lead NIH institute for pain research — currently supports a number of studies funded by the NIH examining a variety of topics related to pain, such as prolonged sensitivity from morphine administration after peripheral nerve injury and the intrathecal administration of resolvins to relieve inflammatory and neuropathic pain. Additionally, the NINDS plays an active role in the NIH’s Health Care Systems Research Collaboratory, which Landis said aims to “provide a framework of implementation methods and best practices to enable the participation of many health care systems in clinical research … to strengthen the relevance of research results for everyday health practice” — a study subject that was at the bottom of the federal pain research portfolio’s totem pole in 2011. (See Graph Below)
One demonstration project under the Collaboratory set out to determine the utility of aggressive interventions in patients with lower back pain based on MRI findings, while another is examining the effectiveness of collaborative chronic pain management in a primary care setting.
But the federally funded study with the most hype at the moment is the “Brain Research Through Advancing Innovative Neurotechnologies” (BRAIN) initiative launched by President Barack Obama on April 2, 2013, which Landis said will support “not just research in static brain imaging, because it’s going to be research looking at information transferred through circuits in the brain.”
In his speech announcing the major research initiative, Obama said “that knowledge could be — will be – transformative,” and Landis noted it will have significant implications for understanding and treating chronic pain. To date, the NIH has invested $40 million to develop new tools and training opportunities for brain research, while the Defense Advanced Research Projects Agency has invested $50 million for demonstrating breakthrough applications based on insights on dynamic functions of the brain, and private-sector partners have invested a combined $122 million to develop new imaging technologies and understand how brain activity leads to perception and decision-making — all of which exemplify successful collaboration in pain research, Landis said.
“As we move forward, we’re all going to have to work together, from health care professionals, to advocacy, to private industry,” Landis said. “If we partner and work together toward common goals, I think we can make a huge difference.”
Responding to Landis's keynote speech, American Pain Society President Roger B. Fillingim, PhD, noted "investments in pain research will further demonstrate the benefits of the multidisciplinary approach in treating pain, not as the consequence of a specific disease, but rather as a multi-faceted human condition characterized by suffering related to myriad sensations, thoughts, emotions, and behaviors, all within a social context." However, Fillingim pointed out that pain research only accounts for 1 percent of NIH research grants at a time when the annual cost of untreated and undertreated chronic pain is estimated at $635 billion a year.
“The federal government’s limited investment in pain research is terribly out of sync with the prevalence and impact of chronic pain in our society, which is estimated at 100 million, or one in three Americans, and accounts for more than 25 percent of all physician office visits," Fillingim said in a press release. “The best hope for achieving significant advances in pain prevention and treatment is through directing a more appropriate level of funding for pain research grants that will translate advances in pain science into relief for patients.”