Female Patients with Psoriasis, Related Clinical Characteristics More Likely to Develop Psoriatic Arthritis
This retrospective cohort study suggests the potential benefits of greater use of screening, though additional research on these predictive factors may be necessary as well.
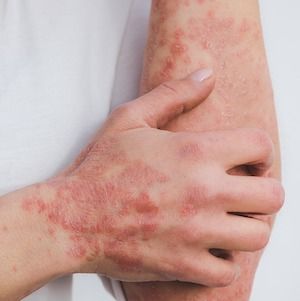
Female psoriasis patients with severe disease, nail involvement, and requiring oral systemic therapy for their condition may have a greater risk of developing psoriatic arthritis (PsA), according to recent findings.1
These data resulted from a new retrospective cohort study conducted to assess the different clinical characteristics of individuals with psoriasis. The research team sought to identify the predictive factors of PsA.
This research was led by Wai Yang Loo, MD, from the department of medicine at Universiti Malaya, Kuala Lumpur’s division of rheumatology. Loo and colleagues noted that the recognition of these predictive elements in PsA’s development could promote more informed decision-making, especially given that addressing PsA early is known to allow for better long-term outcomes among patients.2
“Thus, the objective of this study was to evaluate the clinical characteristics of patients with psoriasis who have developed PsA, and to identify factors that predict PsA in a relatively large and diverse group of patients with psoriasis,” Loo and colleagues wrote.
Background and Findings
The investigators used a retrospective cohort study design, carrying out their research on adult patients with psoriasis at the University of Malaya Medical Centre (UMMC) located in Kuala Lumpur. This research took place from January 2010 - December 2019.
Those with psoriasis diagnoses made by dermatologists and who had had follow-up appointments were included, and individuals shown to have unconfirmed diagnoses or overlapping issues such as rheumatoid arthritis were excluded by the investigators. The research team collected demographic and comorbidity information using electronic medical records, looking at race, body mass index (BMI), sex, education, habits related to smoking, marital status, intake of alcohol, and comorbidities such as diabetes and hypertension.
Clinical characteristics of psoriasis as well as PsA were also evaluated by the team, as they looked into duration, age at the time of patients’ diagnosis, family history, skin and nail involvement and severity, and other treatments for psoriasis. The team also looked at duration between psoriasis and PsA diagnosis, age during PsA diagnosis, inflammatory markers (ESR and CRP), involvement of joints, and treatment modalities for psoriasis before a diagnosis of PsA.
Treatment categories the investigators identified included phototherapy, topicals, oral systemic therapy (including acitretin and conventional synthetic disease-modifying anti-rheumatic drugs [DMARDs]), and biologic DMARDs. The research team made distinctions regarding treatment initiation for psoriasis versus PsA.
The team ended up recruiting 330 subjects with psoriasis, among whom 25% were found top have later developed PsA. Among individuals in the study who later reported PsA, 45.8% were of Malay ethnicity, 28.9% were of Chinese descent, and 25.3% were of Indian descent. They noted that the average age at diagnosis of PsA was 54.2 years, adding that the duration average was 36 months from first diagnosis of psoriasis to that of PsA.
Overall, the research team found that the elements linked with greater risk of PsA diagnosis included being female (odds ratio [OR] = 3.33, 95% confidence interval [CI] 1.78–6.22), having a severe case of psoriasis (OR = 27.41, 95% CI 7.58–99.11), the existence of nail involvement (OR = 5.36, 95% CI 2.50–11.51), and having had of oral systemic treatment before the diagnosis of PsA (OR = 4.09, 95% CI 2.04–8.22).
“The findings of this study suggested that patients with psoriasis who are female, have nail involvement, severe skin psoriasis, and use of systemic therapies for psoriasis are at greater risk of developing PsA,” they wrote. “Patients may benefit from increased screening, which can lead to earlier diagnosis and treatment. More extensive studies are needed to better understand the predictive factors of PsA.”
References
- Loo WY, Tee YC, Han WH, et al. Predictive factors of psoriatic arthritis in a diverse population with psoriasis. Journal of International Medical Research. 2024;52(1). doi:10.1177/03000605231221014.
- Haroon M, Gallagher P, FitzGerald O. Diagnostic delay of more than 6 months contributes to poor radiographic and functional outcome in psoriatic arthritis. Ann Rheum Dis 2015; 74: 1045–1050.
2 Commerce Drive
Cranbury, NJ 08512
All rights reserved.