Publication
Article
Older Woman With Scaling Behind Her Ears
Author(s):
This 69-year-old woman requested evaluation of scaling behind her left ear, which has been present for 8 months after she started a new shampoo.
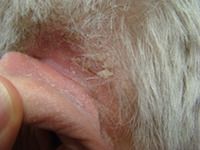
This 69-year-old woman requested evaluation of scaling behind her left ear, which has been present for 8 months after she started a new shampoo. She stopped the shampoo about a month ago and has applied antibiotic ointment with no improvement. She also notes erythema and scale behind her right ear. Her past medical history includes a previous stroke, COPD and history of basal cell cancer.
What is your diagnosis?
A. Auricular rosacea
B. Psoriasis
C. Eczema
D. Tinea capitis
E. Seborrhea
The hallmark of seborrhea, also known as seborrheic dermatitis, is its waxy greasy scale as seen behind the ear in this older woman. It usually occurs in the nasolabial folds, eyebrows, beard area, and scalp, frequently with associated erythema. Milder cases will have finer scaling than this woman's thick sloughing scale.
Occasionally, as in this case, there will be fissuring and serous drainage. Seborrhea is caused by inflammation associated with the yeast Malassezia furfur, also called pityrosporum ovale or orbiculare, which can overgrow in skin with numerous sebaceous glands. Seborrhea is treated primarily with antifungal medications including topical ketoconazole and ciclopirox.
Ketoconazole is available as a topical cream, lotion, foam and shampoo. The associated inflammation can be treated with topical steroids. For unclear reasons, seborrhea is more common in patients with HIV, Parkinson's and strokes. It is unlikely that the patient's shampoo played a role in her seborrheic dermatitis1.
Rosacea is an inflammatory condition with associated erythema and telangiectasias predominantly of the mid-face. There is an ocular form causing inflammation around the eyes with potential for conjunctivitis, blepharitis and corneal disease. There is no auricular form2.
Psoriasis frequently involves the scalp, but its hallmark scale is silvery, usually on top of erythematous plaques. In addition to the scalp and trunk it has a predilection for the extensor surfaces of the extremities.
Eczema causes scale with associated erythema. It is more common on flexural surfaces, often in circular patches with fine scale. It is frequently seen in atopic individuals who have allergies and asthma, and is exacerbated by drying agents and irritation.
Tinea capitis should also be included in the differential diagnosis of scale on the scalp. Its scale is usually much finer and infection can involve the hair shafts and follicles which requires treatment with systemic antifungal medications. Occasionally there is thickened boggy associated inflammation called kerion which is treated with steroids to reduce the inflammation along with systemic antifungals3.
References
May-Jun;27(3):226-8.
About the author:
Daniel Stulberg, MD, is a Professor of Family and Community Medicine at the University of New Mexico. After completing his training at the University of Michigan, he worked in private practice in rural Arizona before moving into full-time teaching. Dr. Stulberg has published multiple articles and presented at many national conferences regarding skin care and treatment. He continues to practice the full spectrum of family medicine with an emphasis on dermatology and procedures.





