Publication
Article
Poor Functioning, Costly EHRs Not Worth the Effort for Family Physicians
Author(s):
Nearly two-thirds of family physicians would not purchase their current electronic health record (EHR) system again due to poor functionality and high costs, according to new data that discovered alarming disconnect between care providers' health information technology needs and the present state of EHR technology.

Nearly two-thirds of family physicians (FPs) would not purchase their current electronic health record (EHR) system again due to poor functionality and high costs, according to new data that discovered alarming disconnect between care providers’ health information technology (HIT) needs and the present state of EHR technology.
In a national survey conducted by research firm MPI Group and published in Medical Economics on Feb. 10, 2014, approximately 1,000 physicians — 32% of whom practice in family medicine — responded to queries regarding the impact of their current EHRs on costs, care coordination, functionality, patient care quality, and financial losses or gains.
Despite receiving up to $107,750 in EHR adoption incentives through the Medicaid and Medicare Meaningful Use programs, 63% of the FPs surveyed said their systems have resulted in financial losses for their practices due to “increasing costs of implementation, training, annual licensing fees, hardware and associated serves … (and) unanticipated costs associated with the need to increase staff, coupled with a loss in productivity.”
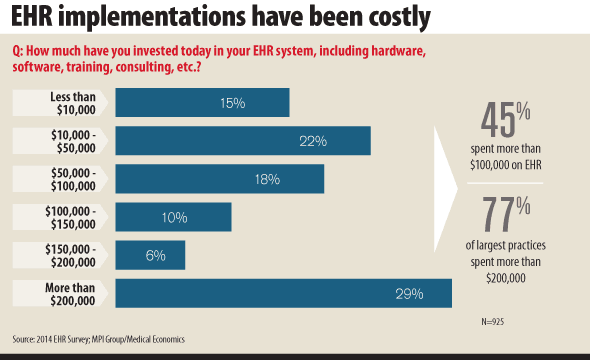
Aside from cost, 67% of the respondents noted their frustration with system functionality is driving their decision to switch EHR software. Interestingly, poor functionality had greater significance among those representing practices with 10 or more physicians, as nearly three-quarters of them reported it would influence their decision to switch systems, compared to 43% who cited cost as their top decision factor.
In response to those functionality issues, 45% of the FPs indicated EHRs are worsening patient care. In fact, one respondent anonymously commented that his or her practice “used to see 32 patients a day with one technician; now, we struggle to see 24 patients a day with 4 techs, and we provide worse care.” Additionally, roughly two-thirds of FPs said their coordination of care with hospitals has not improved with EHR use.
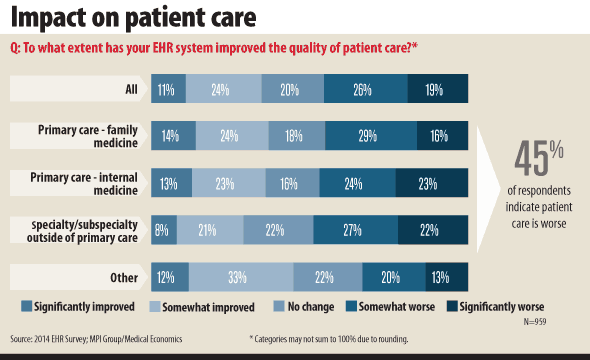
“While some physicians cited benefits of accessing patient data, availability of practice metrics, and e-prescribing conveniences for patients, most physicians do not believe these systems come close to creating new efficiencies or sharing data with multiple providers or improving patient care,” the survey said. As a result, nearly 70% of FPs said their EHR investment has not been worth the effort, resources, and costs. In fact, an earlier report by RAND Corporation found the aforementioned issues related to EHR use are driving professional dissatisfaction among physicians.
In spite of their high dissatisfaction, two-thirds of FPs felt optimistic that their current EHR system will be viable in 5 years. Only 25% of the survey respondents doubted their HIT vendor would still be in business by that time.
