Reduced Tendon Stiffness, Physical Function Observed in Rheumatoid Arthritis and Ankylosing Spondylitis
Though physicians are already aware that rheumatoid arthritis (RA) and ankylosing spondylitis (AS) cause inflammation in joints, tendons, and surrounding muscle tissues, the effects of those chronic autoimmune disorders on stiffness, strength, and function of the patellar tendon have not yet been determined.
Though physicians are already aware that rheumatoid arthritis (RA) and ankylosing spondylitis (AS) cause inflammation in joints, tendons, and surrounding muscle tissues, the effects of those chronic autoimmune disorders on stiffness, strength, and function of the patellar tendon — which works with the quadriceps muscles and quadriceps tendon to straighten the knee and maintain balance — have not yet been determined.
In an attempt to identify the adverse alterations in the tendon’s physiological properties as a result of RA and AS, Verena Matschke, MD, and colleagues from the School of Sport, Health, and Exercise Sciences at Bangor University in Wales compared 18 stable RA patients to 18 age- and sex-matched healthy control subjects and 12 stable AS patients to 12 controls. All participants were submitted to electromyography, isokinetic dynamometry, and ultrasound in order to obtain accurate assessments of patella tendon stiffness and cross-sectional area (CSA), as well as quadriceps muscle force and CSA.
The results of their “Patellar Tendon Properties and Lower Limb Function in Rheumatoid Arthritis and Ankylosing Spondylitis versus Healthy Controls” cross-sectional clinical study, which were recently published in The Scientific World Journal, found patella tendon stiffness was greatly reduced in RA and AS patients compared to the control subjects, which the authors attributed to “local and systemic effects of cytokines on the tendon, since proinflammatory cytokines are known to alter tendon structural characteristics in inflammatory arthropathies.”
However, there was no significant difference in quadriceps muscle force or quadriceps CSA among the three participant groups, though despite their preserved muscle strength and size, the RA and AS patients had substantial impairments in physical function accompanying the changes in their patella tendons’ physiological properties. (Table)
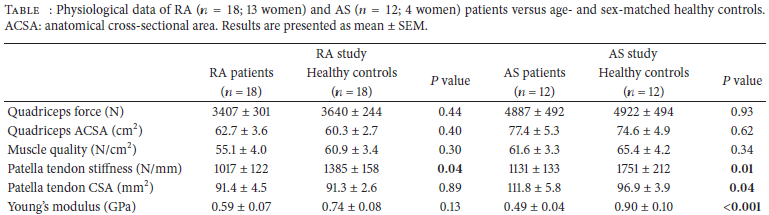
In addition, tendon CSA was much larger in AS patients, but not in RA patients, due to the fact that the tendon thickened in the AS group, yet remained unchanged in size in the RA group — reflecting “characteristic entheseal inflammatory changes of perientheseal swelling and edema and bone marrow edema associated with knee synovitis” that are apparent in AS but not seen in RA, the authors noted.
“The present study reveals that patella tendon properties are adversely affected in RA and AS and possibly contribute to the disability associated with these conditions. The demonstration of different changes in tendon structure add to our increasing understanding of the differences between the pathologies of RA and AS,” the authors concluded. “However, further research is needed to elucidate the role of tendon properties in the impact of chronic arthropathies, and to develop and evaluate treatments for preserving and restoring function of the muscle-tendon complex.”
The cross-sectional study was supported by a grant from the North West Wales National Health Service Trust.