Sick Day Rules in Nephrology, with Kim Zuber, PA-C, and Jane Davis, DNP
In their latest column, Kim Zuber, PA-C, and Jane Davis, DNP, break down the concept of "sick day rules" and what this means for providers caring for those with kidney disease.
(Left to Right) Jane Davis, DNP, and Kim Zuber, PA-C
Credit: Self

‘Sick day rules’ (managing medications when not eating or drinking) are frequently applied in medicine.
Chart 1: Signs and symptoms for activation of ‘Sick Day Rules’4

It is routine to adjust medications when patients are ill or undergoing procedures, but the ‘formal’ adoption of ‘sick day rules’ is unusual in the US. However, outpatient ‘sick day rules’ are common in Canada, Australia, New Zealand, and many European countries. The local pharmacist often adjusts outpatient medications to decrease acute kidney injury (AKI) incidence.1,2 When sick day guidelines were originally conceived in 2013, they were part of a worldwide effort to decrease the incidence of AKI.3 Yet, as is often the case in medicine, there are more nuances to ‘sick day rules’ than the original concept introduced.
Chart 2: Need for Immediate Medical Intervention4
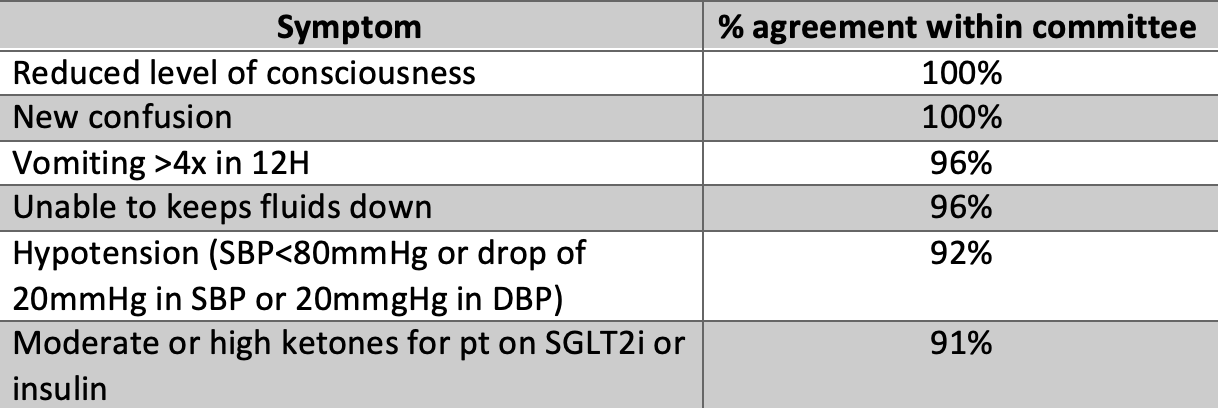
Chart 3: Self-Management appropriate4

The National Institute for Health Care Excellence (NICE) convened an international expert panel in late 2022 to develop a consensus on ‘sick day rules.’4 The panel included a multidisciplinary group of 26 experts from 4 countries and 10 medical disciplines. The panel listed 42 specific recommendations: 5 that are signs or symptoms of dehydration (Chart 1), 6 that require immediate medical interventions (Chart 2), and 14 scenarios for patient self-management (Chart 3). Although some scenarios had less than 100% agreement, most recommendations were close to unanimous. The expert panel also agreed on which medications qualify under the ‘sick day rules.’ (Chart 4)
Chart 4: Medications to be adjusted for sick day rules4
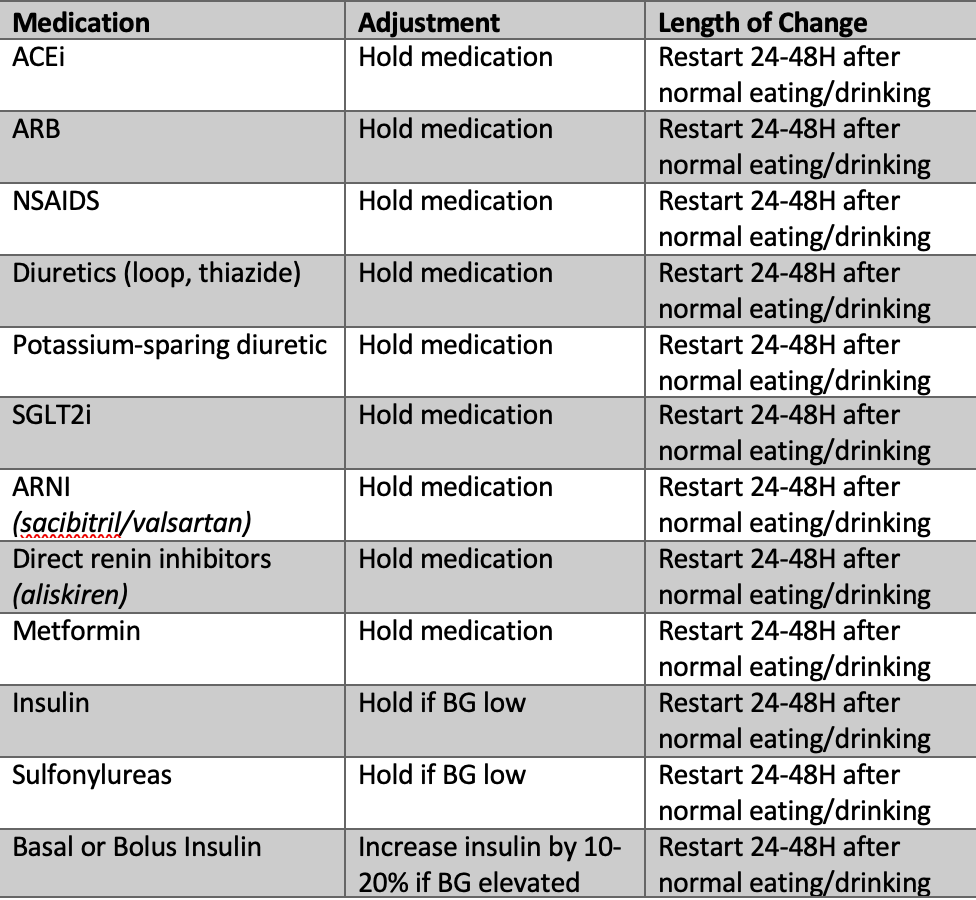
Educating and involving patients in adjusting medications to fit circumstances is essential for successful self-management. Up to 50% of Americans are estimated to have at least chronic disease, which requires management and, often, medication adjustment.5 Self-management techniques have proved to be successful for patients with diabetes, asthma and hypertension.6 However, ‘sick day rules’ represent a new frontier in medication management. The guidelines establish categories for intervention based on severity ranging from complete self-management to a 911 call. While most sick day guidelines focus on diabetes management, the newer guidelines include SGLT2 inhibitors, anti-hypertensive medications, and diuretics. The focus is to address complications related to either volume depletion, hypo or hyperglycemia, or ketoacidosis.
Any guideline has its supporters and detractors; however, the concept of holding medications while ‘sick’ is postulated to decrease the incidence of iatrogenic AKI and thus save nephrons. However, only time will tell.
References:
- National Institute of care and Excellence (NICE) Acute kidney injury: prevention, detection and management, NICE guideline. December 18, 2019, www.nice.org.uk/guidance/ng148, guideline 1.2.13 pg 12. Accessed June 17, 2023
- Lea-Henry TN, Baird-Gunning J, Petzel E, Roberts DM. Medication management on sick days. Aust Prescr. 2017 Oct;40(5):168-173.
- Sick day guidance - think kidneys. Think Kidneys NHS. January 2018. Accessed June 17, 2023. https://www.thinkkidneys.nhs.uk/aki/wp-content/uploads/sites/2/2018/01/Think-Kidneys-Sick-Day-Guidance-2018.pdf.
- Watson KE, Dhaliwal K, Robertshaw S, et al for PAUSE (Preventing Medication Complications During Acute Illness Through Symptom Evaluation and Sick Day Guidance) Medication Safety Advisory Panel. Consensus Recommendations for Sick Day Medication Guidance for People With Diabetes, Kidney, or Cardiovascular Disease: A Modified Delphi Process. Am J Kidney Dis. 2023 May;81(5):564-574.
- Watson KE, Dhaliwal K, McMurtry E, et al. Sick Day Medication Guidance for People With Diabetes, Kidney Disease, or Cardiovascular Disease: A Systematic Scoping Review. Kidney Med. 2022 May 28;4(9):100491.
- Kwong YD, Tuot DS. Optimizing Self-Management Programs in Kidney Disease: Implementation of Sick-Day Protocols. Kidney Med. 2022 Aug 11;4(9):100530.