In Multi-Faceted Psoriasis Treatments, Immunosuppressants can Play Key Role
A small British study indicates that the use of several immunosuppressive agents can restore the effectiveness of ustekinumab (Stelara) in patients with psoriasis and psoriatic arthritis.
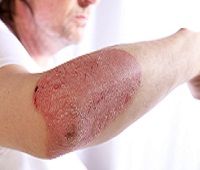
A small British study indicates that the use of several immunosuppressive agents can restore the effectiveness of ustekinumab (Stelara) in patients with psoriasis and psoriatic arthritis.
Investigators retrospectively studied 76 patients who took ustekinumab between October, 2009 and April, 2015. They identified 7 patients who stopped responding well to treatment and began taking the immunosuppressive medications methotrexate (2 patients), fumaric acid esters (1 patient), azathioprine (1 patient) or hydroxyurea (3 patients). The cohort included 2 women and 5 men. All of them had psoriasis, and 2 of them had psoriatic arthritis as well.
Patients used ustekinumab anywhere from 8 months to 20 months (average time: 14.1 months) before the drug’s effect began to wane and they began taking an immunosuppressive agent. Each combination then controlled disease for at least 37 additional months (and for as much as 68 additional months) in all patients. Indeed, combination therapy continued to control disease in all but 2 patients at the end of the study period.
Investigators performed a non-paired 2-tail t test and found a significant difference with a P value of .002 between the Psoriasis Area and Severity Index (PASI) before and after an immunosuppressive agent was added.
“In our population of patients, we found that the addition of an immunosuppressive agent to ustekinumab seemed to restore response,” the study authors wrote in JAAD Case Report. “Patients 1 through 6 had a good response at week 16 and subsequently efficacy dipped. At this point, an immunosuppressive agent was added, and efficacy was then recaptured. Because there is evidence that the survival of a biologic depreciates year after year, this combination could potentially prolong the survival of a biologic therapy, thereby delaying the inevitable decrease in efficacy when one is switched from one biologic to another.”
The new study is not the first to find to find value in combining immunosuppression and biologic treatments in patients with rheumatic diseases.
A 2010 study published in The Journal of Rheumatology found that the combination of adalimumab (Humira) and methotrexate produced better 5-year outcomes than adalimumab alone (or methotrexate alone) in 497 patients who had early rheumatoid arthritis at baseline. A 2012 study published in the Annals of the Rheumatic Diseases found that methotrexate reduces immunogenicity in a dose-dependent manner when used on rheumatoid arthritis patients treated with adalimumab.
A 2014 study of 239 patients with ulcerative colitis, moreover, found that the combination of azathioprine and infliximab (Remicade) worked better than either agent used as monotherapy. Corticosteroid-free remission was achieved at week 16 by 39.7% (31 of 78) of patients receiving infliximab/azathioprine, compared with 22.1% (17 of 77) receiving infliximab alone (P = 0.017) and 23.7% (18 of 76) receiving azathioprine alone (P = 0.032). As far back as 2006, a study published in Gastroenterology found that the addition of azathioprine increased the efficacy of infliximab in patients with Crohn’s disease.
Most prior studies have assumed that combinations work better than monotherapy because both parts of the combination fight disease directly (immunosuppressants are effective treatments for rheumatic disease in many cases). However, the authors of the new study believe the pattern of response in their cohort suggests that another benefit to combinations is that immunosuppression boosts the effect of biologic medication.
“None of our patients responded to systemic immunosuppression on their own,” they wrote. “These same immunosuppressants were subsequently introduced in addition to ustekinumab. We found that in most of the cases the doses of the additional immunosuppressive agents tended to be smaller than the standard dose of the same agents when used in the treatment of psoriasis.”