Study Uncovers Frequent Overdiagnosis of Barrett's Esophagus
Barrett's esophagus is frequently overdiagnosed in clinical settings, which has broad implications for patient health, medical costs, and psychological stress due to perceived cancer risk.
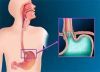
Barrett’s esophagus (BE) is frequently overdiagnosed in clinical settings, which has broad implications for patient health, medical costs, and psychological stress due to perceived cancer risk, according to results from the Barrett’s Esophagus Endoscopic Revision (BEER) study published in the April 2014 issue of Gastrointestinal Endoscopy.
Robert Ganz, MD, FASGE, of Minnesota Gastroenterology, PA, in St. Paul, MN, and colleagues studied 130 patients diagnosed with BE who previously underwent endoscopy and were scheduled to return for routine surveillance endoscopy and biopsy. In the study, BE was defined as columnar-lined epithelium (CLE) in the tubular esophagus proximal to the gastric folds and intestinal metaplasia (IM), with goblet cells on biopsy.
Among the patients previously diagnosed with BE, 88 (67.7%) were confirmed to have the digestive disease by the study authors, while 42 (32.3%) had their diagnosis revised to no BE [95% confidence interval (CI), 24.4-41.1%]. While all 3 of the endoscopists involved in the study agreed on the confirmed cases of BE, they only agreed on 38 of the 42 cases with a revised diagnosis.
Of the 42 patients with a revised diagnosis, 5 had no visible CLE above the gastric folds, but they did have IM. Meanwhile, 18 of the 42 had neither visible CLE nor IM. Even though the remaining 19 patients with a revised diagnosis appeared to be visually consistent with BE, IM could not be confirmed.
Based on the sample represented in this study, at least 24.4% of patients diagnosed with BE in the United States would not have their diagnosis verified on repeat examination endoscopies and surveillance biopsies, the authors concluded.
Patients who were young, female, and had small or absent hiatal hernia were more likely to have their diagnosis revised. The investigators also found patients with short-segment BE were more likely to have a diagnosis revision. Only 1 of the 30 patients with long-segment BE had the initial diagnosis revised.
In response to their findings, the researchers called for an enhanced definition of the gastroesophageal junction region, stricter accountability for a BE diagnosis, and improved education of endoscopists. They suggested reconsidering published estimates of the prevalence of BE and the cancer risk based on unconfirmed endoscopic diagnoses of BE, particularly for studies with a large number of patients with short-segment BE.
“Given the accepted limitations and lack of uniform consensus of endoscopic definitions in BE diagnosis, it is surprising that there has not been more consideration of the impact of incorrect, overdiagnosis of BE,” the authors wrote.
