Taking a closer look at rotator cuff disorders
ABSTRACT: Symptomatic rotator cuff disease usually occurs whenbiological factors combine with dynamic events in the setting of staticstructural problems. At risk are persons with compromised blood supplyto the cuff tissues; a history of repetitive overhead or sudden,acute trauma to the rotator cuff; or abnormalities that disrupt thebalance of forces across the cuff. The key to management lies in understandingrotator cuff anatomy and biomechanics. Patients maypresent with pain and weakness, but tears also may be asymptomatic.A combination of physical examination, shoulder testing, and MRIusually will confirm the diagnosis. Evidence suggests that rotator cuffdisease can progress if the patient does not receive treatment. Rest,corticosteroids, and physical therapy are the basics of conservativecare. (J Musculoskel Med. 2008;25:481-488)
ABSTRACT: Symptomatic rotator cuff disease usually occurs when biological factors combine with dynamic events in the setting of static structural problems. At risk are persons with compromised blood supply to the cuff tissues; a history of repetitive overhead or sudden, acute trauma to the rotator cuff; or abnormalities that disrupt the balance of forces across the cuff. The key to management lies in understanding rotator cuff anatomy and biomechanics. Patients may present with pain and weakness, but tears also may be asymptomatic. A combination of physical examination, shoulder testing, and MRI usually will confirm the diagnosis. Evidence suggests that rotator cuff disease can progress if the patient does not receive treatment. Rest, corticosteroids, and physical therapy are the basics of conservative care. (J Musculoskel Med. 2008;25:481-488)
Recent advances have greatly improved the understanding of and treatment options for disorders of the rotator cuff and associated subacromial pathology. As a result, several concepts have emerged as central tenets of evaluation and treatment.
Rotator cuff disease has a constellation of signs and symptoms that are associated with an alteration of normal anatomy and function. The incriminating anatomical structure or precipitating event that causes rotator cuff disease may not only relate to abnormal anatomy of the anterior acromion and coracoacromial arch but also include traumatic events, repetitive overhead activity, or glenohumeral joint imbalance associated with asymmetrical capsular tightness. In addition, poor biological health of the rotator cuff tissue may hinder the ability of tendon tissue to recover from small injuries. An appreciation of the complexity of shoulder anatomy, physiology, and biomechanics is an important part of evaluating and treating patients with suspected disorders of the rotator cuff and subacromial space.
A thorough understanding of rotator cuff disease is important to the orthopedists who may provide surgical treatment. It is also important to the primary care physicians, physical therapists, and athletic trainers who are well positioned to make a diagnosis and manage these disorders early in the spectrum of disease progression.
In this 2-part article, I discuss and present a rationale for patient evaluation and management of rotator cuff disease.This first part reviews the anatomy and pathogenesis of various types of rotator cuff disease and approaches to patient evaluation. In the second part, to appear in an upcoming issue of this journal, I will describe the surgical technique and rehabilitation of arthroscopic subacromial decompression, as well as repair of the rotator cuff by both arthroscopic and "mini-open" methods.
ANATOMY AND BIOMECHANICS
Accurate diagnosis and effective management of rotator cuff injuries requires an understanding of shoulder anatomy and biomechanics. An awareness of the discerning features of a patient's history and physical examination, as well as an understanding of potential contributions from surrounding structures, helps clinicians develop a differential diagnosis and formulate an effective treatment plan.
The rotator cuff is formed from the coalescence of the tendon insertions of the subscapularis, supraspinatus, infraspinatus, and teres minor muscles into 1 continuous band over the greater and lesser tuberosities of the proximal humerus (Figure). This arrangement reflects their purpose of functioning in concert. In fact, the name "rotator" cuff may be a misnomer; although the individual muscles of the rotator cuff can rotate the humerus, the major function of the rotator cuff is to depress and stabilize the humeral head, effectively compressing the glenohumeral joint to provide a stable fulcrum for arm movement.1-4
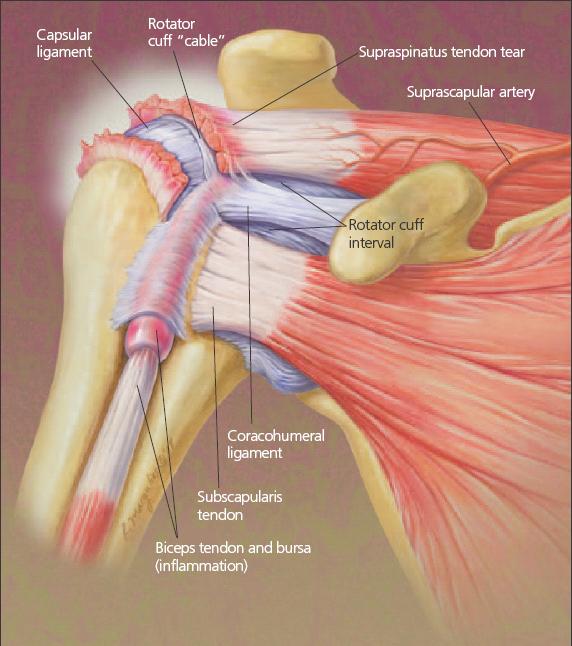
Figure 1 –
An understanding of shoulder anatomy and biomechanics helps clinicians make an accurate diagnosis and effectively manage rotator cuff injuries. Although the individual muscles of the rotator cuff can rotate the humerus, the major function of the rotator cuff is to depress and stabilize the humeral head, effectively compressing the glenohumeral joint to provide a stable fulcrum for arm movement. At the rotator cuff interval, the tendon of the long head of the biceps traverses the glenohumeral joint and the cuff is reinforced by the coracohumeral ligament with extensions to a restraining sling around the biceps and to the rotator cuff "cable," a sling formed from a confluence of the glenohumeral and coracohumeral ligaments. Anterolateral pain results from inflammation; it could mimic rotator cuff impingement.
Abduction strength, although powered by the deltoid, requires a stable fulcrum provided by a functioning rotator cuff. Passive restraints to glenohumeral translation are lax in mid range, so joint stability in this position relies on functioning rotator cuff muscles, which act as dynamic stabilizers.
Dynamic stabilization of the glenohumeral joint is achieved by the coupling of the forces of each rotator cuff muscle5 and the 3 heads of the deltoid muscle.6 The balanced muscle pull increases the concavity compression of the glenohumeral joint. This "force coupling" occurs when the anterior forces from the subscapularis and anterior supraspinatus are balanced by the posterior supraspinatus, infraspinatus, and teres minor. Balancing these forces with even a partial repair of large retracted tears is thought to provide a more stable fulcrum for shoulder motion, leading to functional improvement.3,4
Balancing muscle forces to stabilize the shoulder joint is thought to involve the rotator cuff "cable," an important band of tendon thickening.7 The cable is a normal thickening in the intact supraspinatus and infraspinatus tendons that routinely may be seen arthroscopically from the joint side of a normal rotator cuff.
This thickening in the capsule and overlying tendon extends from its insertion just posterior to the biceps tendon to the inferior border of the infraspinatus tendon7 and is thought to allow the forces across the rotator cuff to be dispersed in a manner similar to a suspension bridge.8 This organization of force distribution explains why some patients can maintain reasonable shoulder function in the setting of a painful full-thickness tear. If their rotator cuff cable is maintained, it can allow for balanced kinematics.9
There is considerable debate about the function of the long head of the biceps tendon within the glenohumeral joint. Some reports suggest it plays a role as a humeral head depressor,10,11 but careful clinical analyses has demonstrated that its role as a humeral head depressor may be less than previously thought.12
The tendon of the long head of the biceps traverses the glenohumeral joint at the rotator cuff interval (see Figure). There the cuff is reinforced by the coracohumeral ligament, with extensions to a restraining sling around the biceps, and to the rotator cuff cable.13 This sling is formed from a confluence of the glenohumeral and coracohumeral ligaments.14 Inflammation in this region produces anterolateral pain, which could mimic rotator cuff impingement but is often discernible by tenderness directly over the biceps tendon in several arm positions.
Although the rotator cuff interval is a normal-appearing gap between the anterior supraspinatus and the superior edge of the subscapularis, the 2 tendon edges are confluent near their insertion onto the humerus. A tear in this region can disrupt the integrity of the biceps' normal restraining mechanism, and biceps stability must be assessed carefully.
The suprascapular artery is a primary vascular supplier to the supraspinatus tendon. The quality of the blood supply to the cuff insertion on the greater and lesser tuberosity is thought to be a factor in the development of rotator cuff disease, particularly in this "critical zone" of the supraspinatus tendon.
The microvascular structure of the supraspinatus tendon suggests that there is a region with a tenuous blood supply and an associated limited capacity for intrinsic repair. This is a common location of partial- and full-thickness rotator cuff tears.15 The proximity of this critical zone of the supraspinatus tendon to the long head of the biceps tendon makes it difficult to determine whether pain in this region is coming from the rotator cuff or the biceps tendon.
Altered bone and ligament anatomy in the subacromial space may be both a cause and an effect of rotator cuff disease. For example, a hooked type 3 acromion, a thickened or calcified coracoacromial ligament, or an excrescence on the anterolateral corner of the acromion represents abnormal bone anatomy, which can cause abrasion of the bursa and supraspinatus tendon, resulting in the inflammation and pain characteristic of early impingement syndrome.
Alternatively, a large retracted rotator cuff tear in which the force coupling has failed will permit superior migration of the humeral head, which may articulate with the coracoacromial arch. Over time, this pathological articulation results in rotator cuff arthropathy in which permanent bone changes occur as the result of a rotator cuff injury.
PATHOGENESIS
The pathogenesis of rotator cuff disease is multifactorial; underlying biological factors set the stage for pathology by limiting the tendon's ability for self-repair. Aging changes the biology of the tendons, resulting in fiber thickening and granulation tissue. Some regions of the tendons have a naturally tenuous blood supply, reducing the intrinsic ability for healing after small injuries. Diabetes mellitus (DM) and nicotine exposure further harm the microvascular supply and, therefore, the healing capacity of the tendon.
Static and dynamic causes of pathology
Symptomatic rotator cuff disease usually occurs when these and other biological factors combine with dynamic events that occur in the setting of static structural problems.16 Structural abnormalities of the coracoacromial arch may cause abnormal compression of the cuff, weakening the tendon and leading to cuff disease and injury. In addition, an accumulation of small injuries to the cuff may lead to dysfunction, which causes other structural problems in the subacromial arch and precipitates further progression of the cuff injury. This vicious circle and the interrelationship between dynamic events and static causes of rotator cuff pathology may be inconsistent: primary structural abnormalities do not always lead to cuff pathology, but cuff pathology often leads to structural abnormalities.
Static structural causes of cuff disease are related to the coracoacromial arch morphology. Changes or abnormalities in the arch can compress the rotator cuff. For example, an acromion with an anterior hook or a lateral slope can pinch the cuff tendon. Acromioclavicular joint arthritis and medial acromial spurring can impinge the supraspinatus. An os acromial or nonunion of an acromial fracture will compress the underlying cuff by changing the shape of the acromion and by promoting the regional growth of osteophytes. Coracoacromial ligament ossification or hypertrophy changes the flexibility and shape of the anterior scapulohumeral articulation, causing abnormal compression of the cuff in provocative positions.
Without a clear-cut high-energy traumatic event, external or internal impingement usually precedes an injury to the rotator cuff. External impingement occurs when the bursal side of the rotator cuff is compressed against the coracoacromial arch. Dynamic causes of external impingement include muscle weakness, which allows for a superior orientation of the humeral head, causing the cuff to abrade on the undersurface of the acromion and coracoacromial ligament. A type 2 superior labral anterior to posterior (SLAP) tear can allow excessive humeral head motion toward the coracoacromial arch. Weak scapular stabilizers can aggravate these problems by placing the acromion at an angle that promotes contact with the underlying cuff tendon.
Internal impingement exists when the articular side of the cuff is pinched between the posterosuperior glenoid and an eccentrically articulating humeral head. Internal impingement may result from a tight posterior capsule, which causes the humeral head to ride superiorly and anteriorly, as often seen in adhesive capsulitis or in throwing athletes (particularly baseball pitchers) who have glenohumeral internal rotation deficit.17
As originally described, internal impingement occurs with the arm in the cocked position of 90° abduction and full external rotation.18 In throwers and overhead athletes, this position brings the articular surface of the rotator cuff insertion against the posterosuperior glenoid rim. Repeated forceful contact between the undersurface of the rotator cuff and the posterosuperior glenoid and labrum is said to cause posterior superior labral lesions. With time, undersurface partial thickness rotator cuff tears follow.
Despite contact between these 2 structures occurring physiologically, theory holds that repetitive contact with excessive force can produce injury. However, many patients with this constellation of pathological findings are not overhead athletes,19 and the condition does not develop in most throwers even though the position is achieved regularly.20
Burkhart and associates17,21,22 developed a comprehensive evaluation of arthroscopic findings, patient outcomes, and biomechanical experimental data to indicate that the so-called internal impingement found in throwers is caused by a complex syndrome related to scapular dyskinesis and kinetic chain abnormalities that result in scapular malposition, inferior medial border prominence, coracoid pain and malposition, and dyskinesis of scapular movement (ie, SICK scapula).This combination of pathomechanics initiates a cascade that leads to type 2 SLAP tears and partial-thickness rotator cuff tears.
EPIDEMIOLOGY/NATURAL HISTORY
Small full-thickness rotator cuff tears exist in shoulders that are somewhat pain-free and have little or no limitation in function. In one study, 23% of 411 asymptomatic volunteers with normal shoulder function were found to have full-thickness rotator cuff tears diagnosed by ultrasonography. In this study,13% were aged 50 to 59 years and 51% were older than 80 years.23 Cadaver dissections have demonstrated rates of up to 60% of partial-thickness or small full-thickness tears in cadavers older than 75 years at the time of death.24 Several factors affect the natural history of various tears; therefore,whether asymptomatic tears will become symptomatic with time often is unpredictable.
Yamaguchi and colleagues25 monitored 44 patients with known bilateral rotator cuff tears in an effort to learn the natural history of asymptomatic rotator cuff tears. In this study, 23 (51%) of the previously asymptomatic shoulders became symptomatic over a mean of 2.8 years, and 9 of 23 patients (39%) who underwent repeat ultrasonography had tear progression. The study results indicate that there is a considerable risk that the size or symptoms or both of an asymptomatic tear will progress without treatment.
The probability of progression of an untreated cuff tear varies with tear characteristics (eg, size, location, mechanism, chronicity), the biological health of the torn tissue (vascularity, presence of DM, nicotine exposure), the status of force coupling in the shoulder (ie, intact rotator cuff cable), and the activity level of the patient. When pain is the predominant presenting complaint, the vast majority of small symptomatic tears often may be managed effectively with oral antiinflammatory medication, selective use of corticosteroid injections,and rehabilitation of the shoulder to improve range of motion and to strengthen the muscles of the rotator cuff and the periscapular stabilizers. It is important to counsel patients that when a small symptomatic tear is successfully "treated" nonoperatively, the tear persists as an asymptomatic tear, rather than spontaneously healing to bone.
Left unmanaged, small painful tears with intact mechanics can enlarge and lead to progressive loss of balanced forces coupling because of violation of the rotator cuff cable. With this progression, the patient begins to experience a significant loss of function in addition to shoulder pain. As the tear enlarges, fat atrophy and retraction of the tear can worsen.26
Further enlargement of the tear may occur with a paradoxical decrease in pain.With extreme tear enlargement and loss of coracohumeral and glenohumeral ligament integrity, the humeral head may rise into the subacromial space, articulate with the acromion and, in time, lead to rotator cuff arthropathy. The probability of a patient progressing through these steps is unpredictable and based on multiple factors, but progression generally occurs at a slow pace over several years.
The course usually is more predictable in overhead athletes. Competitive throwing athletes execute many repetitions of highly demanding motions with complex mechanics. Any imbalance in the kinetic chain, including a weak subscapularis, inadequate scapular mobility or stabilization, or even throwing techniques that cause improper foot placement or arm position during throwing, can initiate the cascade toward pathology.
Recognized early, these problems can be corrected through rehabilitation and training. Failure to recognize or manage these conditions can lead to progression and cause lesions that require surgical repair, including posterosuperior labral tears, anterior shoulder instability, and articular-sided rotator cuff tears.
These lesions should be suspected in a throwing athlete who is not responding to rest, rehabilitation, and appropriate nonoperative treatment. Early symptoms in the throwing athlete include slow warm-ups and stiffness, with no pain. During this time, the shoulder usually responds to rest. If the condition is allowed to progress, cuff-associated pain will occur at the start of the acceleration phase of throwing. Shoulder pain elicited on examination often is alleviated with a relocation of the humeral head to articulate concentrically with the glenoid. These and other subtleties of the shoulder examination are important features of the clinical signs and symptoms of rotator cuff disease.
CLINICAL SIGNS AND SYMPTOMS
Shoulder complaints often are a combination of "pain," "weakness," and "stiffness." An element of each may be caused by rotator cuff pathology. The presentation of rotator cuff disease varies with the etiology and classification of the cuff pathology, ranging from traumatic rotator cuff tears to articular-sided partial-thickness tears associated with "internal impingement" in a thrower or overhead athlete to a classic impingement process with an insidious onset resulting from repetitive overhead activities.
A traumatic tear usually is the result of abrupt traction or impact on the arm that produces immediate pain and weakness in a previously "normal" shoulder. An overhead athlete or thrower with articular-sided rotator cuff tendon pathology will describe a progression of slow warm-ups, stiffness, pain, and loss of performance (eg, fastball velocity or accuracy) as glenohumeral joint imbalance or scapular dyskinesis worsens.
Patients who are progressing along the spectrum of cuff impingement syndrome toward a full cuff tear have a different presentation. Structural abnormalities combined with dynamic events (eg, repetitive overhead activity), perhaps with coexisting intrinsic biological problems in the cuff tendon (eg, poor vascular supply15), often lead to a gradual onset of symptoms that worsen with overhead activities or during sleep directly on the affected shoulder.
In these patients, the initial symptom is pain, which produces a sense of weakness. True weakness evolves with increased pain as a cuff tear develops and may worsen if the tear enlarges to involve the rotator cuff cable. In large, chronic, unmanaged tears, patients experience both pain and weakness; with a chronically nonfunctioning atrophied cuff, they often complain more of weakness than of pain.
PHYSICAL EXAMINATION
When a patient with suspected or known rotator cuff disease is evaluated, a thorough shoulder examination helps the clinician classify the disorder, assess contributing features of the symptoms, and identify potential solutions. Many patients with rotator cuff disease or injury have tenderness at the anterolateral aspect of the humerus at the insertion of the supraspinatus tendon, as well as positive impingement signs, as described by Neer27 and Hawkins and Kennedy.28 In addition, evaluating the long head of the biceps tendon for tenderness and stability is important. Biceps tendon injuries are a common source of anterior shoulder pain; a coexisting subscapularis tear can involve the biceps stabilizing sling, which can lead to painful snapping of the biceps tendon out of the anterior humeral groove.29 Acromioclavicular joint tenderness is a common contributor to shoulder pain. Although degenerative changes seen in this joint on x-ray films often are not painful, bone spurs in this area often promote impingement of the underlying supraspinatus tendon.
Testing
Strength testing of the rotator cuff tendons should isolate each tendon to the greatest extent possible. A patient with a large tear that results in loss of the balanced force coupling across the humeral head often may be able to only shrug the shoulder in an effort to raise the arm. Specific weakness or pain elicited with resisted internal rotation, abduction, or external rotation may be found with isolated tears of the subscapularis, supraspinatus, or infraspinatus, respectively. Often the pain associated with the use of a torn muscle causes weakness. The subscapularis is responsible for internal rotation of the shoulder and can be tested in isolation.
The "belly-press," or Napoleon, test requires that the patient press the hand into the belly.30,31 During this maneuver, the examiner must maintain a straight position of the patient's wrist and prevent the patient from pulling the elbow posteriorly in an effort to compensate for a torn subscapularis.
References:
References
- 1. Burkhart SS. Arthroscopic debridement and decompression for selected rotator cuff tears: clinical results, pathomechanics, and patient selection based on biomechanical parameters. Orthop Clin North Am.1993;24:111-123.
- 2. Burkhart SS. Reconciling the paradox of rotator cuff repair versus debridement: a unified biomechanical rationale for the treatment of rotator cuff tears. Arthroscopy. 1994;10:4-19.
- 3. Burkhart SS. Partial repair of massive rotator cuff tears: the evolution of a concept. Orthop Clin North Am. 1997;28:125-132.
- 4. Burkhart SS, Nottage WM, Ogilvie-Harris DJ, et al. Partial repair of irreparable rotator cuff tears. Arthroscopy. 1994;10:363-370.
- 5. Magarey ME, Jones MA. Dynamic evaluation and early management of altered motor control around the shoulder complex. Man Ther. 2003;8:195-206.
- 6. Lee SB, An KN. Dynamic glenohumeral stability provided by three heads of the deltoid muscle. Clin Orthop Relat Res. 2002;(400):40-47.
- 7. Burkhart SS. Shoulder arthroscopy. New concepts. Clin Sports Med. 1996;15:635-653.
- 8. Burkhart SS, Esch JC, Jolson RS. The rotator crescent and rotator cable: an anatomic description of the shoulder’s “suspension bridge” [published correction appears in Arthroscopy. 1994;10:239]. Arthroscopy. 1993;9:611-616.
- 9. Burkhart SS. Fluoroscopic comparison of kinematic patterns in massive rotator cuff tears: a suspension bridge model. Clin Orthop Relat Res. 1992;(284):144-152.
- 10. McGough RL, Debski RE, Taskiran E, et al. Mechanical properties of the long head of the biceps tendon. Knee Surg Sports Traumatol Arthrosc. 1996;3:226-229.
- 11. Eakin CL, Faber KJ, Hawkins RJ, Hovis WD. Biceps tendon disorders in athletes. J Am Acad Orthop Surg. 1999;7:300-310.
- 12. Nove-Josserand L, Levigne C, Noel E, Walch G. The acromio-humeral interval: a study of the factors influencing its height [in French]. Rev Chir Orthop Reparatrice Appar Mot. 1996;82:379-385.
- 13. Hulstyn MJ, Fadale PD. Arthroscopic anatomy of the shoulder. Orthop Clin North Am. 1995;26:597-612.
- 14. Werner A, Mueller T, Boehm D, Gohlke F. The stabilizing sling for the long head of the biceps tendon in the rotator cuff interval: a histoanatomic study. Am J Sports Med. 2000;28:28-31.
- 15. Lohr JF, Uhthoff HK. The microvascular pattern of the supraspinatus tendon. Clin Orthop Relat Res. 1990;(254):35-38.
- 16. Sano H, Ishii H, Trudel G, Uhthoff HK. Histologic evidence of degeneration at the insertion of 3 rotator cuff tendons: a comparative study with human cadaveric shoulders. J Shoulder Elbow Surg. 1999;8:574-579.
- 17. Burkhart SS, Morgan CD, Kibler WB. The disabled throwing shoulder: spectrum of pathology, part I: pathoanatomy and biomechanics. Arthroscopy. 2003;19:404-420.
- 18. Davidson PA, Elattrache NS, Jobe CM, Jobe FW. Rotator cuff and posterior-superior glenoid labrum injury associated with increased glenohumeral motion: a new site of impingement. J Shoulder Elbow Surg. 1995;4:384-390.
- 19. Budoff JE, Nirschl RP, Ilahi OA, Rodin DM. Internal impingement in the etiology of rotator cuff tendinosis revisited. Arthroscopy. 2003;19:810-814.
- 20. Burkhart SS, Parten PM. Dead arm syndrome: torsional SLAP lesions versus internal impingement. Tech Shoulder Elbow Surg. 2001;2:74-84.
- 21. Burkhart SS, Morgan CD, Kibler WB. The disabled throwing shoulder: spectrum of pathology, part II: evaluation and treatment of SLAP lesions in throwers. Arthroscopy. 2003;19:531-539.
- 22. Burkhart SS, Morgan CD, Kibler WB. The disabled throwing shoulder: spectrum of pathology, part III: the SICK scapula, scapular dyskinesis, the kinetic chain, and rehabilitation. Arthroscopy. 2003;19:641-661.
- 23. Tempelhof S, Rupp S, Seil R. Age-related prevalence of rotator cuff tears in asymptomatic shoulders. J Shoulder Elbow Surg. 1999;8:296-299.
- 24. Sakurai G, Ozaki J, Tomita Y, et al. Incomplete tears of the subscapularis tendon associated with tears of the supraspinatus tendon: cadaveric and clinical studies. J Shoulder Elbow Surg. 1998;7:510-515.
- 25. Yamaguchi K, Tetro AM, Blam O, et al. Natural history of asymptomatic rotator cuff tears: a longitudinal analysis of asymptomatic tears detected sonographically. J Shoulder Elbow Surg. 2001;10:199-203.
- 26. Nakagaki K, Ozaki J, Tomita Y, Tamai S. Fatty degeneration in the supraspinatus muscle after rotator cuff tear. J Shoulder Elbow Surg. 1996;5:194-200.
- 27. Neer CS 2nd. Anterior acromioplasty for the chronic impingement syndrome in the shoulder: a preliminary report. J Bone Joint Surg. 1972;54A:41-50.
- 28. Hawkins RJ, Kennedy JC. Impingement syndrome in athletes. Am J Sports Med. 1980;8:151-158.
- 29. Gerber C, Hersche O, Farron A. Isolated rupture of the subscapularis tendon. J Bone Joint Surg. 1996;78A:1015-1023.
- 30. Burkhart SS, Tehrany AM. Arthroscopic subscapularis tendon repair: technique and preliminary results. Arthroscopy. 2002;18:454-463.
- 31. Lo IK, Burkhart SS. The etiology and assessment of subscapularis tendon tears: a case for subcoracoid impingement, the roller-wringer effect, and TUFF lesions of the subscapularis. Arthroscopy. 2003;19:1142-1150.