Vitamin D Supplementation May Reduce Pain, Improve Sleep in Knee Osteoarthritis Patients
Expanding upon previous investigations of the associations among low vitamin D levels, chronic pain, and poor sleep within the general and non-pain populations, a research poster presented at the American Pain Society 33rd Annual Scientific Meeting suggests correcting inadequate vitamin D levels in middle-aged to older patients with knee osteoarthritis may reduce their clinical pain and improve sleep quality.
Expanding upon previous investigations of the associations among low vitamin D levels, chronic pain, and poor sleep within the general and non-pain populations, a research poster presented at the American Pain Society 33rd Annual Scientific Meeting, held April 30, 2014, to May 3, 2014, in Tampa, FL, suggests correcting inadequate vitamin D levels in middle-aged to older patients with knee osteoarthritis (OA) may reduce their clinical pain and improve sleep quality.
As a sub-study of the ongoing Understanding Pain and Limitations of Osteoarthritic Disease (UPLOAD) trial, Megan E. Petrov, PhD, of Arizona State University in Phoenix, AZ; Roger Fillingim, PhD, and Toni L. Glover, PhD, GNP-BC, FNP-BC, CPE, of the University of Florida in Gainesville, FL; and Burel R. Goodin, PhD, and Laurence A. Bradley, PhD, of the University of Alabama at Birmingham, recruited 100 African-American and non-Hispanic white adults aged 45-75 years with unilateral or bilateral symptomatic knee OA between February 2012 and August 2013.
During an initial visit, the study participants received bilateral knee joint evaluations from a rheumatologist and were assessed on overall health, the Pittsburgh Sleep Quality Index (PSQI), and the Western Ontario and McMaster Universities Arthritis Index (WOMAC) pain subscale. Within the following 2 weeks, the knee OA patients returned for a second visit, during which the researchers collected serum for vitamin D assay via high-performance liquid chromatography. Through that assay, the investigators determined 80% of the patients had serum 25-hydroxyvitamin D [25(OH)D] levels <30 ng/mL; in other words, “vitamin D inadequacy was highly prevalent among community-dwelling people with knee OA,” Petrov and her co-authors wrote.
According to the researchers, knee OA patients with inadequate vitamin D self-reported significantly greater clinical pain on the WOMAC subscale and considerably poorer sleep quality on the PSQI than those with 25(OH)D levels ≥30 ng/mL. Furthermore, “vitamin D group differences in sleep quality were significantly mediated by group differences in clinical pain after controlling for age, race, body mass index (BMI), and symptoms of depression,” the poster authors wrote.
As a result, the researchers said their findings imply “supplementation of vitamin D may reduce clinical pain reports, as well as improve sleep quality among community-dwelling people with knee OA.”
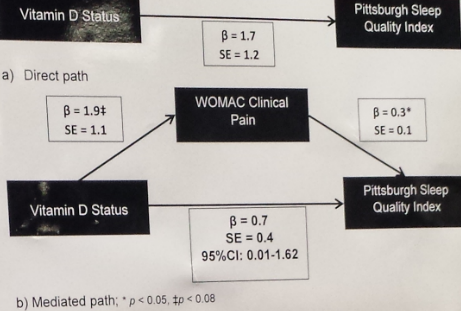
“The relationship between sleep and pain is often thought to be reciprocal; however, in the present sample, clinical pain appears to predict poor sleep quality among those with vitamin D inadequacy,” Petrov and her co-authors noted. Thus, “heightened clinical pain partially explains the association between vitamin D inadequacy and poor sleep quality in middle-aged to older participants with knee OA,” they added.
The study, which was entitled “The Role of Clinical Pain in the Association between Vitamin D Status and Sleep Quality among Adults with Knee Osteoarthritis,” received grant funding from the National Institute on Aging (NIA).