Conducting the “nonshoulder” shoulder examination
Optimal shoulder function is achieved with the kinetic chain. Alterations in this sequenced activation of body segments often are associated with shoulder injury. A screening examination of areas proximal to the shoulder where these alterations often are found can help physicians make the diagnosis.
ABSTRACT: Optimal shoulder function is achieved with the kinetic chain. Alterations in this sequenced activation of body segments often are associated with shoulder injury. A screening examination of areas proximal to the shoulder where these alterations often are found can help physicians make the diagnosis. Core stability provides proximal stability for the distal mobility and function of the limbs. Excessive scapular protraction alters the roles of the scapula in shoulder function. Glenohumeral internal rotation deficit creates abnormal scapular kinematics. Many types of tests may be used to estimate or measure core strength. Physical examination of the scapula is designed to establish the presence or absence of scapular dyskinesis. If the examiner detects scapular dyskinesis, corrective maneuvers can be applied. (J Musculoskel Med. 2011;28:58-64)
Persons performing complex athletic and work tasks achieve optimal shoulder function because of the kinetic chain. This coordinated, sequenced activation of body segments places the distal segment in the optimal position at the optimal velocity with the optimal timing to produce the desired task.1
Alterations in the kinetic chain-including core instability, scapular dyskinesis (alteration of scapular motion), and glenohumeral internal rotation deficit (GIRD)-have been associated with shoulder injury in 50% to 100% of reported cases.2-5 Scapular dyskinesis is found in a particularly high percentage of patients with shoulder injury.
The “nonshoulder” shoulder examination-a screening examination of areas proximal to the shoulder that often are associated with shoulder injury-helps physicians understand the entire spectrum of alterations in the kinetic chain that contribute to the diagnosis of shoulder injury in patients who present with chronic shoulder pain. If alterations are found, more specific and detailed orthopedic examination can proceed. In addition, the alterations that are identified can be managed as part of treatment of patients with shoulder injury.
In this article, we describe the biomechanical basis of kinetic chain alterations that are associated with shoulder injury. Then we outline the key aspects of the nonshoulder physical examination.
BIOMECHANICAL BASIS
The shoulder and core stability
The various body segments play specific roles in the kinetic chain activation sequence. The muscles and joints of the hips, pelvis, and spine (known collectively as the core) are centrally located and can perform many of the stabilizing functions that the body requires for the distal segments (eg, the limbs) to perform their specific functions. Thus, core stability provides proximal stability for the distal mobility and function of the limbs.6
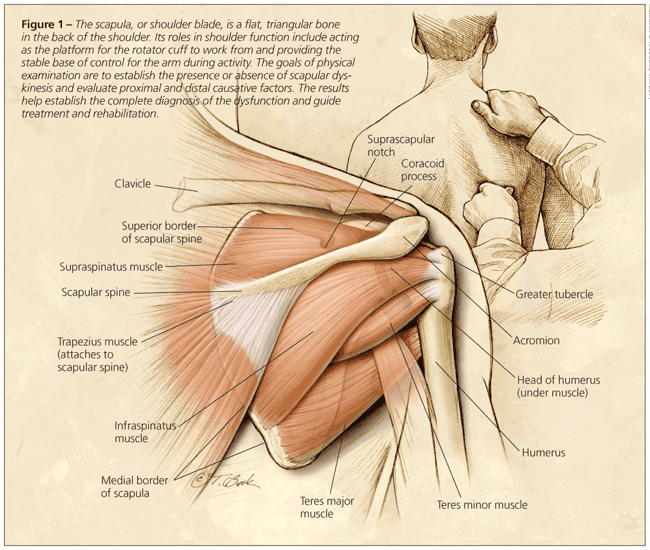
The shoulder acts as a funnel, regulating and transferring forces generated from the core structures to the hand. The scapula (Figure 1) acts as the platform for the rotator cuff to work from and is the stable base of control for the arm during activity.
Scapular motion has been examined in a 3-dimensional context. Studies have shown that it is a composite of 3 motions: upward/downward rotation around a horizontal axis perpendicular to the scapular plane, internal/external rotation around a vertical axis through the plane, and anterior/posterior tilt around a horizontal axis in the plane.2,7 With an intact acromioclavicular (AC) joint, there are 2 translations: upward/downward translation on the thoracic wall and retraction/protraction around the ellipsoid curve of the rib cage.
In this more complex framework, the scapula is shown to have several additional roles in shoulder function: it must posteriorly tilt and externally rotate to clear the acromion from the arm moving in forward elevation or abduction,3,7 and it must internally/externally rotate and posteriorly tilt to maintain the glenoid as a congruent socket for the moving arm and to maximize concavity/compression as well as ball-and-socket kinematics.8 In addition, it must be stabilized dynamically in a position of relative retraction during arm use to maximize activation of all the muscles that originate on it.9
Scapular dyskinesis
This kinetic chain alteration is a combination of decreased posterior tilt and decreased external
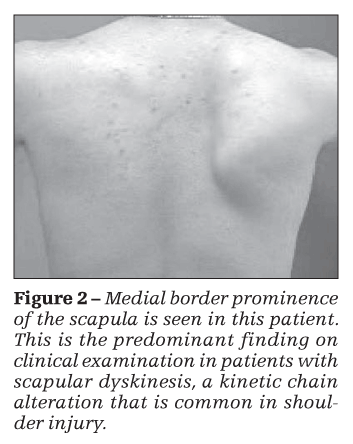
rotation as well as decreased upward rotation.2,3 The predominant finding on clinical examination is prominence of the medial border of the scapula on observation at rest or on motion of the arm in elevation (Figure 2). The prominence represents loss of dynamic control of the translation of scapular retraction-regarded as a key element in closed-chain coupled scapulohumeral rhythm2,7,10-and of the motion of external rotation. If control is lost, gravity, forward arm motion, and muscle activations take the arm and shoulder girdle forward. The biomechanical result is a tendency toward scapular internal rotation and protraction around the rib cage.
Excessive scapular protraction alters the roles of the scapula in shoulder function.11 The normal timing and magnitude of acromial motion are changed; the subacromial space distance is altered; “hyperangulated” joint; and maximal muscle activation may be decreased.
There are 2 categories of causes of scapular dyskinesis: those proximal and those distal to the scapula.12 Proximal causative factors most often include direct alteration of muscle properties- inflexibility, weakness, fatigue, and nerve injury-and usually are managed with rehabilitation.
Muscle weakness has been demonstrated in the serratus anterior and lower trapezius muscles in patients with impingement.3,13 Inflexibility in the pectoralis minor muscle-an absolute decrease in muscle length and increased muscle activation in response to tensile loads-is a common finding in these patients.14 A somewhat rare proximal cause is true nerve injury to the long thoracic or
accessory nerve. Bony proximal causes include thoracic kyphosis and scoliosis with resultant alteration in scapular position.
Distal causative factors most often are associated with anatomical injuries in the AC or GH joints. They also alter muscle activation patterns or activations by causing instability of the bones or through pain-based inhibition; they often require surgery to eliminate their effects and provide the basis for effective rehabilitation. GH instability is associated with altered serratus anterior activation.15
GIRD
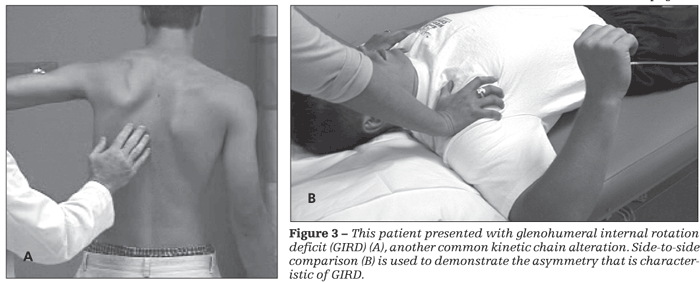
This common distal causative factor-defined as side-to-side asymmetry of greater than 25°or an absolute value of less than 25°(Figure 3)-is thought to be produced by acquired posterior capsular contracture and posterior muscle stiffness; it is seen frequently in all types of shoulder injuries.16,17 GIRD creates abnormal scapular kinematics as a result of the “windup” effect of the arm on the scapula. As the arm is forward flexed, horizontally adducted, and internally rotated during a throwing or working activity, the tight capsule and muscles pull the scapula into a protracted, internally rotated, and anteriorly tilted position; this causes downward rotation of the acromion, thus creating undesired scapular positioning.
THE PHYSICAL
EXAMINATION
Assessing quality of movement
Many types of tests have been described to estimate or measure core strength. Because core strength and core stability are composite actions that involve many segments, tests of individual joints and muscles usually are not satisfactory. Evaluation of specific patterns of motion and sequences of muscle activation and assessment of the result-the quality of the movement-is most beneficial for determining how to institute rehabilitation.18
In assessment of core stability and strength, it is important to evaluate the muscles working in an eccentric, load-absorbing function; the body segments in a closed-chain manner; and the resulting motions in the 3 planes of trunk motion. This method of analysis is difficult to quantify, but it is similar to actual 3-planar core function testing.
One assessment method that incorporates many of these variables is a 3-part protocol: a 1-leg standing balance ability test; a 1-leg squat test; and a standing, 3-plane core strength test.6 The screening part of the evaluation includes the 1-leg standing and 1-leg squat tests.
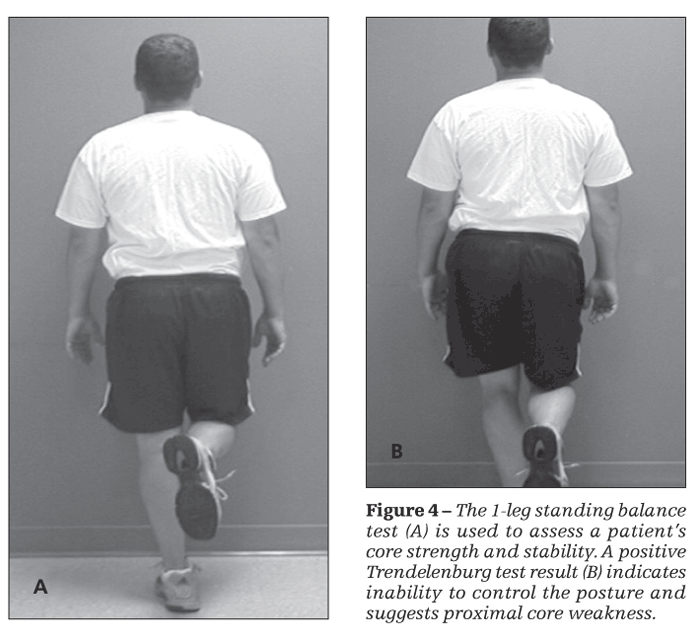
In the standing balance test, the patient is asked to stand on 1 leg and is given no other verbal cue (Figure 4). A positive test result, known as the Trendelenburg sign, is seen when the hip drops on the unsupported side. This indicates inability to control the posture and suggests proximal core weakness.
The 1-leg squat increases load and may show deficits that are not seen in stance. The patient assumes the same starting point as in the standing balance test; he or she is asked to perform repetitive partial (quarter to half) squats and is given no other verbal cues. Deviations in the quality of the movement similar to those in the standing balance test are assessed. A Trendelenburg sign may not be noted on standing balance but may be elicited with a 1-leg squat. The patient may use his arms for balance or may go into an exaggerated flexed or rotated posture known as “corkscrewing” to provide the gluteal or short rotator muscles with greater tension to compensate for other muscular
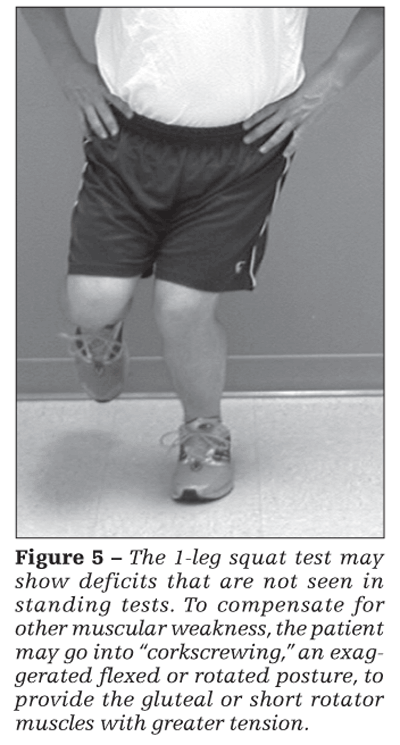
weakness (Figure 5).
3-Plane core testing
This is a more in-depth evaluation used to quantify core control in the various planes of spine and core motion. Reliability and validity studies of specific tests have not been done, but clinical experience has demonstrated that this battery of tests provides useful information that allows specific rehabilitation protocols to be instituted for increased core function.6
Testing is done with the patient standing a given distance (usually 3 inches) away from a wall (Figure 6). In sagittal plane testing, he faces away from the wall. He is asked to move his body backward slowly, keeping his feet flat on the floor, to just barely touch his head against the wall. This can be done with both legs on the ground initially and progress to partial weight bearing on each side and, ultimately, to single-leg standing. Sagittal plane core strength testing creates eccentric activation in the abdominal, quadriceps, and hip flexor muscles and concentric activation in the hip and spine extensor muscles.

Frontal plane testing (Figure 7) is done by asking the patient to stand with one side and then the other 3 inches away from the wall. While he is standing on the outside leg, he is asked to barely touch his inside shoulder to the wall. This test evaluates eccentric strength of the quadratus lumborum, hip abductors, and some long spinal muscles that are working in a frontal plane.
As in the sagittal plane test, transverse plane motion is evaluated by asking the patient to stand 3 inches away from the wall and progress from bilateral weight bearing to a single-leg stance and touch one shoulder and then the other just barely against the wall. Quality of motion and speed can be assessed. With lesser degrees of core strength, there is a greater breakdown in the patient’s ability to maintain a single-leg stance and to just barely touch the wall. Transverse plane motions assessed with this test incorporate abdominal, hip rotator, and spine extensor muscles. If muscles and planes of motion are found to be deficient, appropriate therapy may be instituted.
Examining the scapula
Physical examination of the scapula is designed to establish the presence or absence of scapular

dyskinesis and evaluate proximal and distal causative factors. Dynamic maneuvers may be used to assess the effect of correction of dyskinesis on impingement symptoms. The examination results help establish the complete diagnosis of all the elements of the dysfunction and guide treatment and rehabilitation.
The scapular examination should be conducted mostly from the posterior aspect.8 The scapula should be exposed for complete visualization by having the patient wear gowning or a tank top or remove his shirt. The patient should be checked in the resting posture for side-to-side asymmetry and, especially, for evidence of inferior medial or medial border prominence. If determining the positions is difficult, marking the superior and inferior medial borders may help.
Screening for dyskinesis
Such screening may be done by asking the patient to move his arms in ascent and descent 3 to 5 times. Usually, this movement demonstrates muscle weakness and medial border prominence, which indicates dyskinesis. If necessary, performance of up to 10 more repetitions or addition of 3- to 5-lb weights will further highlight the weakness.19 Alteration in medial scapular border motion in any plane, singly or in combination, is recorded in a “yes” (present) or “no” (absent) fashion. The clinically observed yes/no evaluation has a correlation of 0.84 with biomechanically determined abnormalities in symptomatic patients and has a high predictive value.20,21
Watching scapular position for dyskinesis while the patient performs wall push-ups may help assess periscapular muscle strength. Isolated serratus anterior and trapezius muscle testing can be done for nerve-related palsies. Any deficits found during the screening examination should be evaluated in more depth. Often found is some evidence of proximal muscle weakness or inflexibility, which affects the optimum mechanics of scapulohumeral rhythm. It may not be the sole factor, but it must be considered in the rehabilitation protocols.22
Corrective maneuvers
If the examiner detects scapular dyskinesis, then corrective maneuvers can be applied. Maneuvers that alter the injury symptoms provide the examiner and the patient with information about the role of scapular dyskinesis in the total picture of dysfunction that accompanies shoulder injury and needs to be corrected.
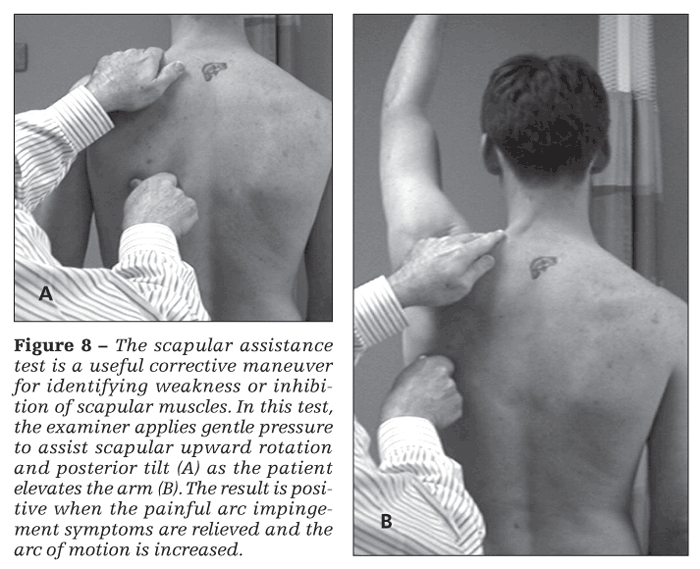
The scapular assistance test (SAT) and the scapular retraction test (SRT) are useful corrective maneuvers. In the SAT (Figure 8), the examiner applies gentle pressure to assist scapular upward rotation and posterior tilt as the patient elevates the arm. The result is positive when the painful arc impingement symptoms are relieved and the arc of motion is increased. This finding helps the clinician identify weakness or inhibition of scapular muscles, especially the lower trapezius muscle.
In the SRT, the examiner places and stabilizes the scapula in a retracted position. The result is positive when the demonstrated supraspinatus strength, determined by manual muscle testing, is increased in the retracted position.
Weakness of the supraspinatus can be apparent during the classic “empty can” manual muscle test, in which downward resistance is applied to the arm positioned in 90° of abduction in the scapular plane and the humerus is internally rotated. With the use of a handheld dynamometer, the SRT has been shown to elicit a 24% greater increase in supraspinatus strength than does the empty can test.23
The SRT result also may be positive when the symptoms of “internal impingement” (pain at the posterior joint line with arm external rotation) are relieved by scapular retraction. This finding indicates that the scapula is excessively protracted, resulting in impingement of the glenoid, labrum, and humeral head. A positive SAT or SRT result shows that scapular dyskinesis is directly involved in producing the symptoms and indicates a need for early scapular rehabilitation exercises to be included to improve scapular control.
Screening evaluation of GIRD
This screening should be done by stabilizing the scapula, placing the arm in 90° of abduction in the scapular plane, and rotating the arm. Rotation should be taken to tightness in the motion or the start of forward scapular movement in a windup fashion or both. Bilateral measurements should be obtained.
Coracoid-based inflexibility may be assessed with palpation of the pectoralis minor and biceps short head muscles as they run off the coracoid tip. Usually, they are tender to palpation, even if they are not symptomatic in use; can be traced to their insertions as taut bands; and will create symptoms of soreness and stiffness when the scapulae are maximally retracted manually. A rough measurement of pectoralis minor tightness may be obtained by asking the patient to stand against a wall and measuring the distance from the wall to the anterior acromial tip.
References:
References
1. Putnam CA. Sequential motions of body segments in striking and throwing skills: descriptions and explanations. J Biomech. 1993;26(suppl 1):125-135.
2. Lukasiewicz AC, McClure P, Michener L, et al. Comparison of 3-dimensional scapular position and orientation between subjects with and without shoulder impingement. J Orthop Sports Phys Ther. 1999;29:574-586.
3. Ludewig PM, Cook TM. Alterations in shoulder kinematics and associated muscle activity in people with symptoms of shoulder impingement. Phys Ther. 2000;80:276-291.
4. Cools AM, Witvrouw EE, Declercq GA, et al. Scapular muscle recruitment patterns: trapezius muscle latency with and without impingement symptoms. Am J Sports Med. 2003;31:542-549.
5. Warner JJ, Micheli LJ, Arslanian LE, et al. Scapulothoracic motion in normal shoulders and shoulders with glenohumeral instability and impingement syndrome: a study using Moiré topographic analysis. Clin Orthop Relat Res. 1992;285:191-199.
6. Kibler WB, Press J, Sciascia A. The role of core stability in athletic function. Sports Med. 2006;36:189-198.
7. McClure PW, Michener LA, Sennett BJ, Karduna AR. Direct 3-dimensional measurement of scapular kinematics during dynamic movements in vivo. J Shoulder Elbow Surg. 2001;10:269-277.
8. Kibler WB, McMullen J. Scapular dyskinesis and its relation to shoulder pain. J Am Acad Orthop Surg. 2003;11:142-151.
9. Kebaetse M, McClure P, Pratt NA. Thoracic position effect on shoulder range of motion, strength, and three-dimensional scapular kinematics. Arch Phys Med Rehab. 1999;80:945-950.
10. Happee R, Van der Helm FC. Control of shoulder muscles during goal directed movements, an inverse dynamic analysis. J Biomech. 1995;28:1179-1191.
11. Kibler WB. The role of the scapula in athletic shoulder function. Am J Sports Med. 1998;26:325-337.
12. Rubin BD, Kibler WB. Fundamental principles of shoulder rehabilitation: conservative to postoperative management. Arthroscopy. 2002;18(9 suppl 2):29-39.
13. Cools AM, Witvrouw EE, Mahieu NN, Danneels LA. Isokinetic scapular muscle performance in overhead athletes with and without impingement symptoms. J Athl Train. 2005;40:104-110.
14. Borstad JD, Ludewig PM. The effect of long versus short pectoralis minor resting length on scapular kinematics in healthy individuals. J Orthop Sports Phys Ther. 2005;35:227-238.
15. Glousman R, Jobe F, Tibone J, et al. Dynamic electromyographic analysis of the throwing shoulder with glenohumeral instability. J Bone Joint Surg. 1988;70A:220-226.
16. Burkhart SS, Morgan CD, Kibler WB. The disabled throwing shoulder: spectrum of pathology Part I:
pathoanatomy and biomechanics. Arthroscopy. 2003;19:404-420.
17. Tyler TF, Nicholas SJ, Roy T, Gleim GW. Quantification of posterior capsule tightness and motion loss in patients with shoulder impingement. Am J Sports Med. 2000;28:668-673.
18. Nadler SF, Malanga GA, DePrince M, et al. The relationship between lower extremity injury, low back pain, and hip muscle strength in male and female collegiate athletes. Clin J Sport Med. 2000;10:89-97.
19. McClure P, Tate AR, Kareha S, et al. A clinical method for identifying scapular dyskinesis, part 1: reliability. J Athl Train. 2009;44:160-164.
20. Tate AR, McClure P, Kareha S, et al. A clinical method for identifying scapular dyskinesis, part 2: validity. J Athl Train. 2009;44:165-173.
21. Uhl TL, Kibler WB, Gecewich B, Tripp BL. Evaluation of clinical assessment methods for scapular dyskinesis. Arthroscopy. 2009;25:1240-1248.
22. Kibler WB, McMullen J, Uhl TL. Shoulder rehabilitation strategies, guidelines, and practice. Oper Tech Sports Med. 2000;8:258-267.
23. Kibler WB, Sciascia A, Dome D. Evaluation of apparent and absolute supraspinatus strength in patients with shoulder injury using the scapular retraction test. Am J Sports Med. 2006;34:1643-1647.
Recommended readings
The authors suggest the following sources for readers seeking more information:
• Ekstrom RA, Donatelli RA, Soderberg GL. Surface electromyographic analysis of exercises for the trapezius and serratus anterior muscles. J Orthop Sports Phys Ther. 2003;33:247-258. This study demonstrates that the relationship between the trapezius fibers and the serratus anterior is a crucial factor in the proper function of the scapula.
• Kibler WB, Sciascia A. Current concepts: scapular dyskinesis. Br J Sports Med. 2010;44:300-305. This article contains great detail regarding the roles of the scapula in normal function as well as the alterations that can occur when injury is present.
• Myers JB, Laudner KG, Pasquale MR, et al. Scapular position and orientation in throwing athletes. Am J Sports Med. 2005;33:263-271. This article demonstrates adaptations in scapular kinematics that result from throwing.