Congenital Skin Lesion in a Newborn
This newborn infant was noted to have a congenital skin malformation on both sides of his face. However, the pregnancy was uncomplicated, he is feeding well, and no other abnormalities were seen on examination.
a) Branchial cleft cyst
b) Preauricular sinus
c) Cystic hygroma
d) Dermoid cyst
e) Accessory tragus
Diagnosis
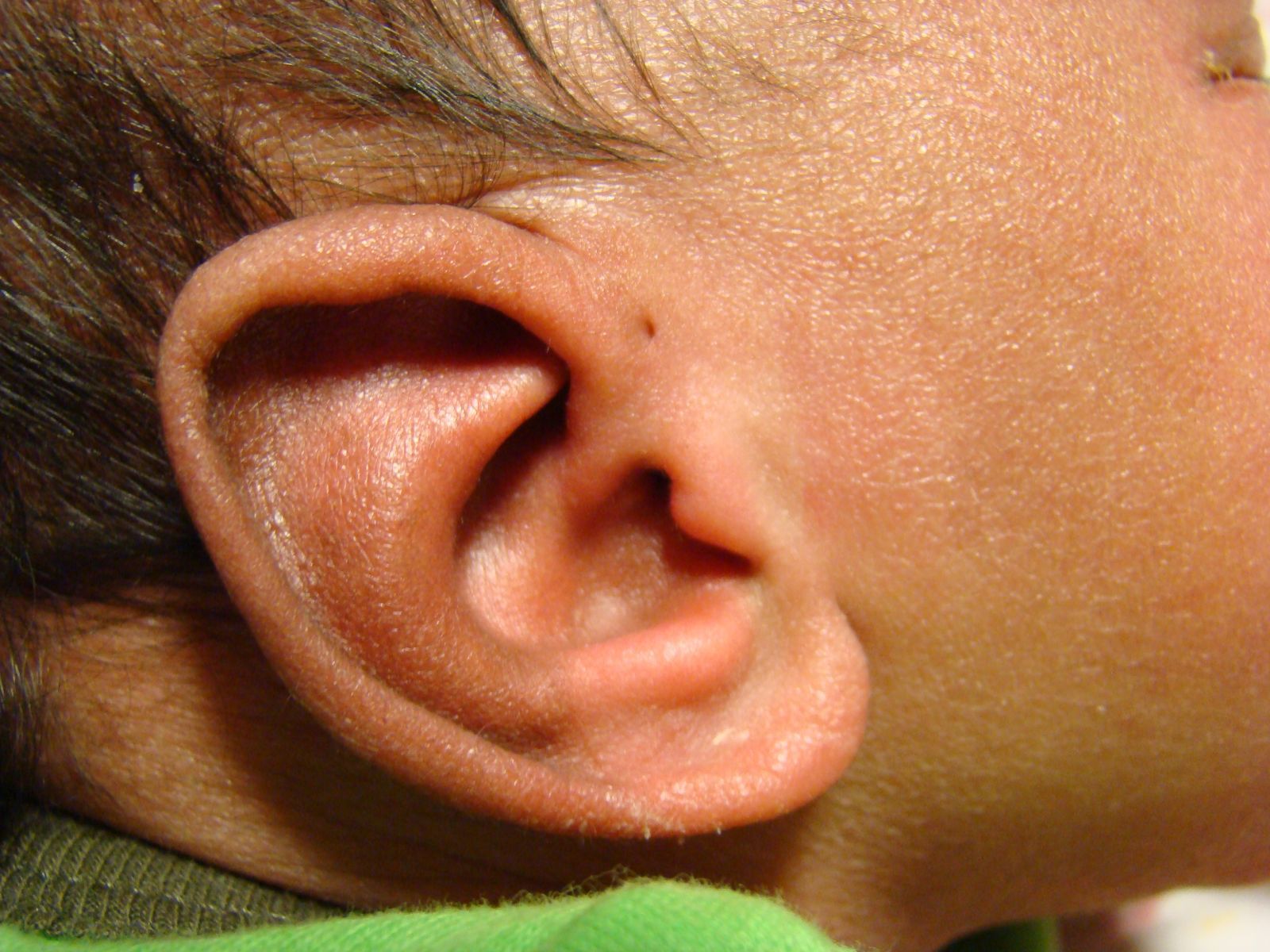
Preauricular sinuses usually occur either bilaterally or unilaterally at the anterosuperior aspect of the attachment of the ear, due to imperfect pinna formation from the developing tubercles. Although the pits are usually asymptomatic, they can get inflamed or infected, or even produce chronic drainage.
If the lesion is symptomatic, then resection of the entire sinus tract — possibly including a portion of cartilage and sometimes requiring a flap — is required to prevent recurrence and complications.1 If there are no other anomalies aside from the preauricular sinuses, then the incidence of renal abnormalities is no greater than baseline, so no further imaging or studies would be required beyond a thorough physical examination.2
In contrast, branchial cleft cysts occur inferior to the angle of the jaw or in the upper neck, and they are often diagnosed when they become fluctuant as a result of inflammation or infection.3
Cystic hygroma has more recently been called macrocystic lymphatic malformation, and just as the name implies, it is an enlargement of the lymph channels that can cause significant swelling. Since the lesion is filled with lymphatic fluid, it can be transilluminated on occasion.3
Dermoid cysts of the head and neck usually occur in the midline, inferior to the chin, due to an invagination of the epithelium. The resulting cystic structure can enlarge over time, and it is typically treated with excision.3
An accessory tragus is also related to the embryonic formation of the ear and would occur in the same location as a preauricular sinus. However, it is a raised lesion that requires no treatment.
References
1. Gan E, Anicete R, Tan H, Balakrishnan A. Preauricular sinuses in the pediatric population: techniques and recurrence rates. International Journal of Pediatric Otorhinolaryngology. 2013 Sep; 77(3): 372-78. http://www.ncbi.nlm.nih.gov/pubmed/23266157.
2. Firat Y, Sireci S, Yakinci C, Akarçay M, KarakaÅŸ HM, Firat AK, Kizilay A, SelimoÄŸlu E. Isolated preauricular pits and tags: is it necessary to investigate renal abnormalities and hearing impairment? Eur Arch Otorhinolaryngol. 2008 Sep;265(9):1057-60. http://www.ncbi.nlm.nih.gov/pubmed/18253743.
3. Flint P, Haughey B, Lund V, Niparko, J, Richardson M, Robbins T, Thomas J. (2010). Differential diagnosis of neck masses. Cummings Otolaryngology: Head and Neck Surgery. (5th ed.). Philadelphia: Mosby.
About the Authors

Daniel Stulberg, MD, is a Professor of Family and Community Medicine at the University of New Mexico. After completing his training at the University of Michigan, he worked in private practice in rural Arizona before moving into full-time teaching. Stulberg has published multiple articles and presented at many national conferences regarding skin care and treatment. He continues to practice the full spectrum of family medicine with an emphasis on dermatology and procedures.
