Painful Buttock Lesion in a Pregnant Woman
A 36-year-old pregnant woman at 27 weeks gestation presented to the obstetrical triage for evaluation of possible abscess due to a lesion on her buttock that first appeared 1 week ago. Since that time, it has become increasingly painful and itchy. Although she denies any systemic symptoms, her pregnancy is complicated by gestational diabetes and obesity. However, she is HIV negative and her other prenatal labs were unremarkable.
a) Gestational pemphigoid
b) Abscess
c) Herpes zoster
d) Cholestasis of pregnancy
e) Herpes simplex
Diagnosis
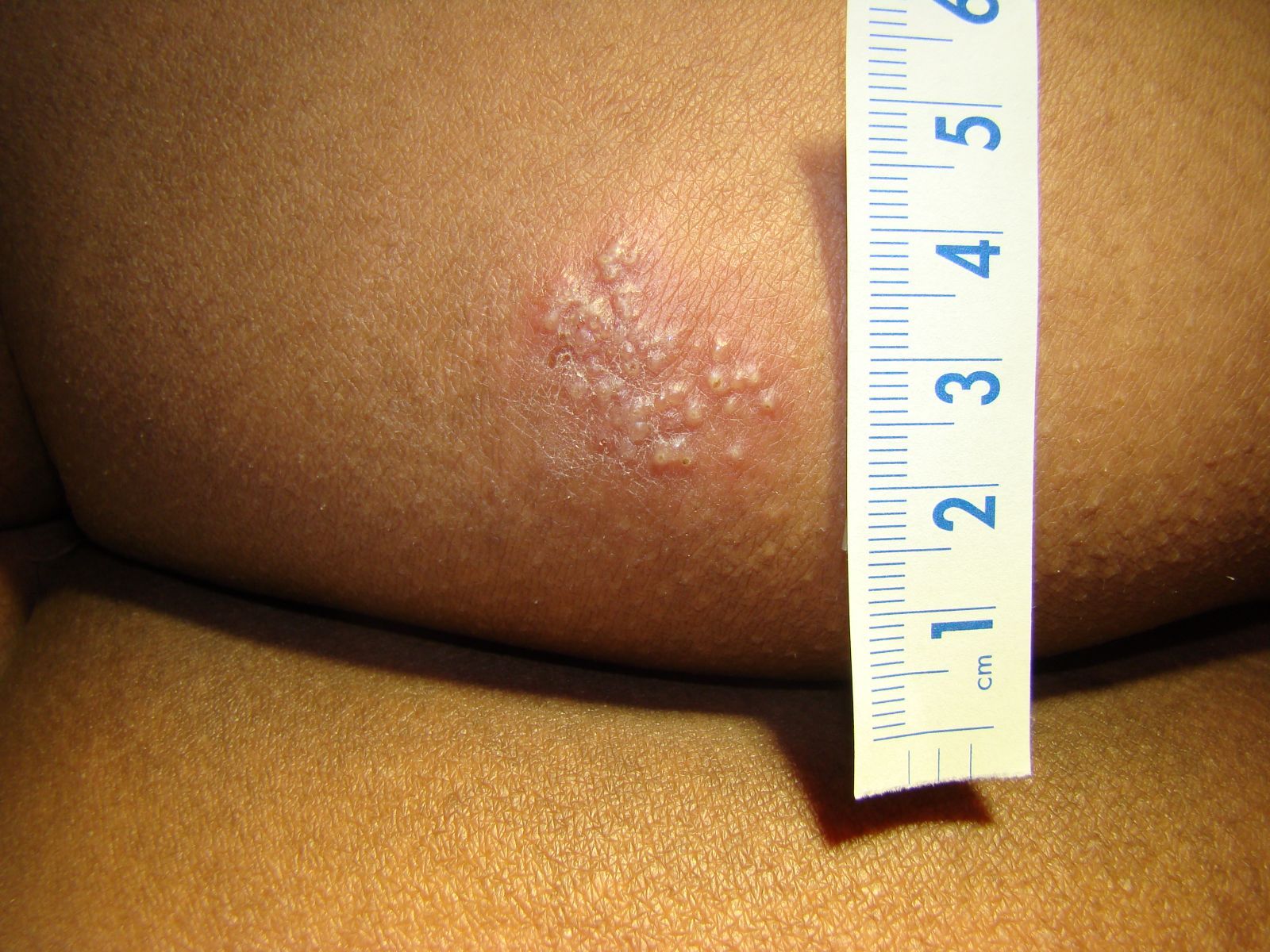
Herpes simplex virus (HSV) presents as a cluster of vesicular lesions on an erythematous base. Over time, the vesicles often become pustular and there is typically associated pain and itching.
HSV outbreaks anywhere near the genitals are usually assumed to be herpes genitalis, or related to sexual transmission. In the setting of an active lesion, its diagnosis can be based on culture or polymerase chain reaction (PCR), which is more sensitive than culture. Serology with immunoglobulin G (IgG) and immunoglobulin M (IgM) is also helpful for determining whether a lesion is primary or recurrent.
In this case, viral culture was obtained after the woman’s unroofed vesicles were positive for HSV. Serology was also performed and revealed positive HSV 2 IgG and negative HSV IgM, which indicated recurrence, rather than a primary outbreak.
Since this patient is pregnant, she will be treated with acyclovir for suppression starting at 36 weeks gestation and continuing through delivery. If the patient has any genital lesions or prodromal symptoms at the onset of labor, then she will require delivery by cesarean section to reduce the likelihood of vertical transmission to the neonate, which can be fatal.1-2
Gestational pemphigoid, or herpes gestationis, is a rare autoimmune disease characterized by blistering skin lesions that start near the umbilicus and progress to cover the entire body. The lesions are typically accompanied by itching and usually regress after delivery. They can be treated with oral corticosteroids.3
Although the patient was referred for evaluation of possible abscess due to her gestational diabetes, which increases risk for abscess formation, there was neither fluctuance on palpation of the area nor purulent drainage.
While herpes zoster has a similar vesicular appearance, it occurs as a result of the reactivation of the virus from previous varicella infection or immunization. On the trunk, the infection is activated in the nerves of the dorsal root ganglion; therefore, it tends to present in a dermatomal distribution instead of a localized cluster.
Cholestasis of pregnancy causes severe itching, but unless it progresses to jaundice, there are no skin findings. The diagnosis is confirmed by serum bile acid levels. As fetal loss may occur,4 delivery is indicated when the fetal lungs mature around 37 weeks gestation or when signs of fetal distress are present, whichever occurs earlier.
References
1. ACOG Committee on Practice Bulletins. ACOG Practice Bulletin. Clinical management guidelines for obstetrician-gynecologists. No. 82. Management of herpes in pregnancy. Obstet Gynecol. 2007 June;109:1489.
2. Watts DH, et al. A double-blind, randomized, placebo-controlled trial of acyclovir in late pregnancy for the reduction of herpes simplex virus shedding and cesarean delivery. Am J Obstet Gynecol. 2003;188:836-43. http://www.ncbi.nlm.nih.gov/pubmed/12634667.
3. LipozenÄić J, Ljubojevic S, Bukvić-Mokos Z. Gestational pemphigoid. Clin Dermatol. 2012 Jan-Feb;30(1):51-5. http://www.ncbi.nlm.nih.gov/pubmed/22137226.
4. Geenes V, Chappell LC, Seed PT, Steer PJ, Knight M, Williamson C. Association of severe intrahepatic cholestasis of pregnancy with adverse pregnancy outcomes: a prospective population-based case-control study. Hepatology. 2014 Apr;59(4):1482-91. http://www.ncbi.nlm.nih.gov/pubmed/23857305.
About the Authors

Daniel Stulberg, MD, is a Professor of Family and Community Medicine at the University of New Mexico. After completing his training at the University of Michigan, he worked in private practice in rural Arizona before moving into full-time teaching. Stulberg has published multiple articles and presented at many national conferences regarding skin care and treatment. He continues to practice the full spectrum of family medicine with an emphasis on dermatology and procedures.
Lauren Thaxton, MD, MBA, is a graduate of the Texas Tech University Health Sciences Center and currently an Obstetrics and Gynecology Resident at the University of New Mexico.
