Ring-shaped Lesions on a Man's Arm
A 59-year-old man presented to clinic with concerns that his ezetimibe prescription was causing an itchy rash. The rash first appeared on his hand 1 year ago and now it involves his arm, as well. The man's past medical history is significant for coronary artery disease, hypertension, hyperlipidemia, and hypothyroidism. He has tried a topical antifungal agent and oral fluconazole to no avail.
a) Granuloma annulare
b) Tinea versicolor
c) Tinea corporis
d) Psoriasis
e) Urticaria
Diagnosis
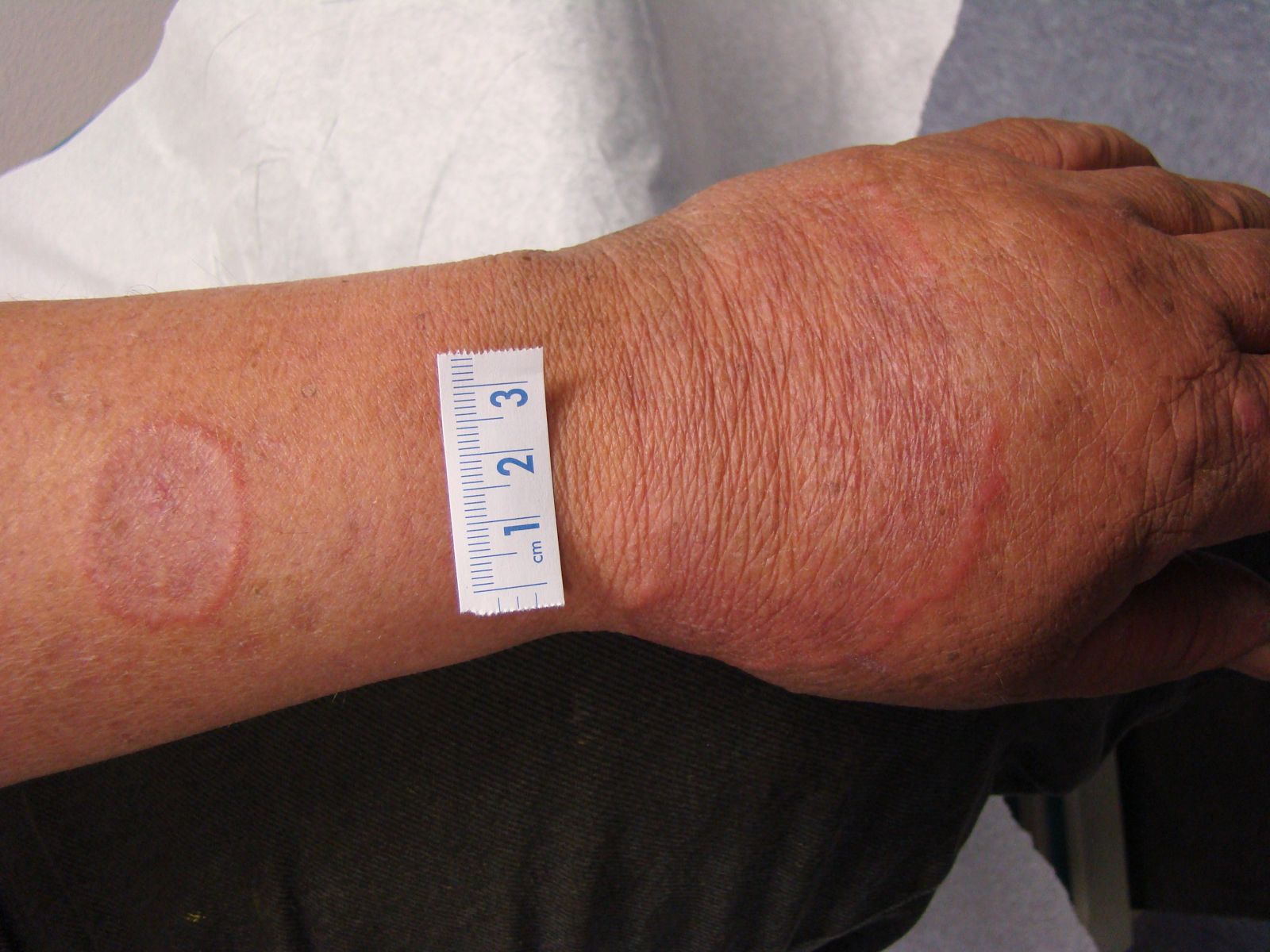
This man has granuloma annulare (GA), which is clinically characterized by an enlarged, raised ring of tissue that is usually flesh colored or erythematous. The annular lesions often start out as papules or clusters that coalesce into the raised, bordered lesions seen on this patient’s hand and arm. If the diagnosis is uncertain, biopsies can be helpful, as they will show palisading granulomas and degenerating collagen.
GA can present in children or adults and its localized form is usually self-limited over the course of 2 years. The most common GA treatment is high-potency topical or intralesional steroids injected into the raised portions of the lesions. Although many other treatments have been attempted in GA, a recent review article found the evidence for pharmacologic treatment is limited to case reports and small trials.1 Cryosurgery and photodynamic therapy have also been used in small trials with some success.
While there are associations to many systemic diseases in patients with generalized or atypical GA, there are no clear links. Therefore, those patients should undergo further testing based on their history, physical, and risk factors for malignancy.
Tinea versicolor (TV) is characterized by hyper- or hypopigmented lesions on the trunk caused by pityrosporum orbiculare, which is also known as malassezia furfur. The condition often has fine scales that show a “spaghetti and meatballs” pattern on microscopy. TV responds to topical antifungal agents, in addition to the oral fluconazole this patient received.2
Tinea corporis often affects the extremities in a circular pattern, leading to the lay term of ringworm. Unlike GA, it is usually scaly and lacks the central depression of the annular lesions. Tinea corporis should also respond to antifungal treatments.
The plaques of psoriasis typically have thick, silvery scales. However, the condition can present without scales in intertriginous areas or when it is partially treated with topical steroids. Like tinea corporis, psorasis lacks the central depression of GA.
Urticaria can present acutely or chronically as raised erythematous plaques, which contrast with the annular shape of GA. Since urticarial lesions are caused by histamine and fluid shifts, they tend to change relatively quickly in minutes or days. On the contrary, GA lesions occur and resolve over a period of months to years, since GA is a granulomatous disease.
References
1. Thornsberry LA, English JC 3rd. Etiology, diagnosis, and therapeutic management of granuloma annulare: an update. Am J Clin Dermatol. 2013 Aug;14(4):279-90. http://www.ncbi.nlm.nih.gov/pubmed/23696233.
2. Farschian M, Yaghoobi R, Samadi K. Fluconazole versus ketoconazole in the treatment of tinea versicolor. J Dermatolog Treat. 2002 Jun;13(2):73-6. http://www.ncbi.nlm.nih.gov/pubmed/12060505.
About the Author

Daniel Stulberg, MD, is a Professor of Family and Community Medicine at the University of New Mexico. After completing his training at the University of Michigan, he worked in private practice in rural Arizona before moving into full-time teaching. Stulberg has published multiple articles and presented at many national conferences regarding skin care and treatment. He continues to practice the full spectrum of family medicine with an emphasis on dermatology and procedures.
