Tofacitinib Effective, Safe in Chinese Patients With Active Psoriatic Arthritis
Study results are the first to demonstrate that tofacitinib may be an effective treatment option for Chinese patients with active psoriatic arthritis.
The efficiency of tofacitinib (Xejianz, Pfizer) was greater than placebo in Chinese patients with active psoriatic arthritis (PsA) and inadequate response to at least 1 conventional synthetic disease-modifying antirheumatic drug (csDMARD), according to a study published in RMD Open.1
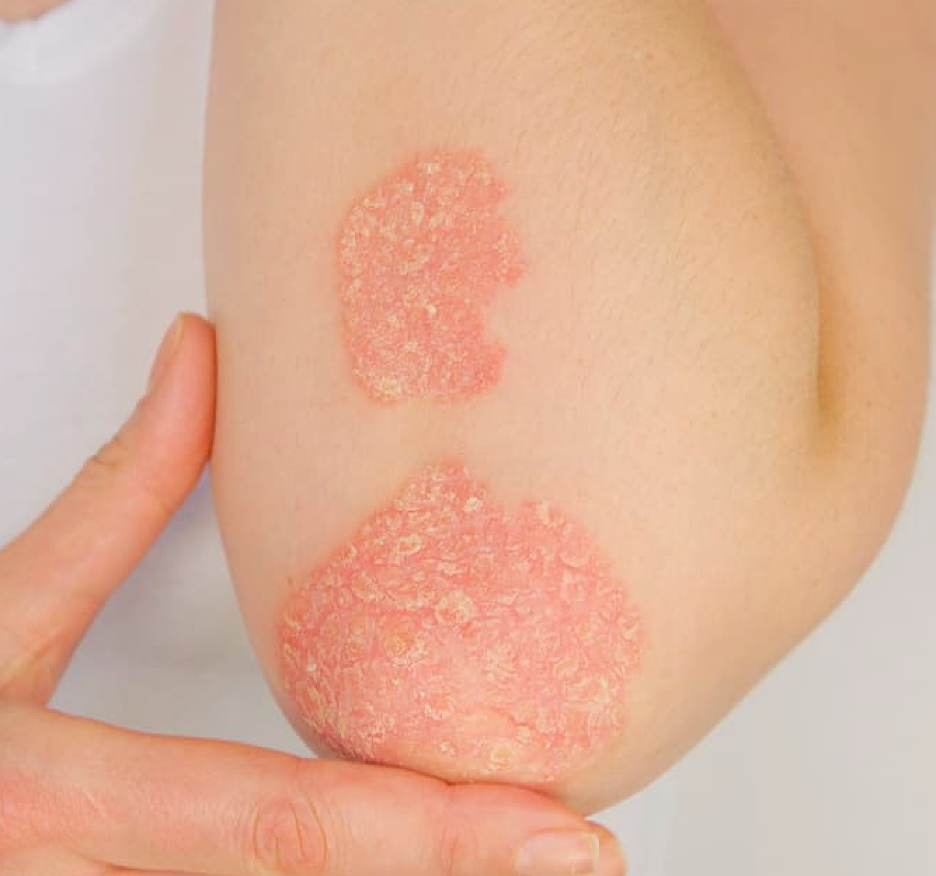
Image Credit: Adobe Stock/helivideo
“The results of this study are the first to demonstrate that tofacitinib may be an effective treatment option for Chinese patients with active PsA,” Xiaofeng Zeng, MD, of Peking Union Medical College Hospital in Beijing, China, stated. “Tofacitinib was well tolerated, with safety outcomes consistent with the established safety profile in the PsA global clinical program and other indications.”
Tofacitinib, an oral Janus kinase inhibitor, is approved by the US Food and Drug Administration (FDA) for the treatment of active PsA when 1 or more tumor necrosis factor (TNF) blocker medicine has been used and did not work well or cannot be tolerated. Tofacitinib is also approved for the treatment of PsA in Taiwan, but there are no approved advanced therapies for PsA in mainland China. Mainland China was not included in the global clinical development program of tofacitinib in PsA and only a small number of patients from Taiwan were enrolled in the program. Therefore, data supporting the efficacy and safety of tofacitinib in Chinese patients with PsA are limited.
This 6-month, double-blind, phase 3 study randomized 136 patients (mean age 45.3 years, 79% male) to tofacitinib 5 mg twice daily and 68 patients (mean age 43.9 years, 42% male) to placebo; switched to tofacitinib 5 mg twice daily after month 3. The primary endpoint was the American College of Rheumatology (ACR50) response at month 3. Secondary endpoints, through month 6, included: ACR20/50/70 response; change from baseline in Health Assessment Questionnaire-Disability Index (HAQ-DI); ≥75% improvement in Psoriasis Area and Severity Index (PASI75) response, and enthesitis and dactylitis resolution. Safety was assessed throughout.
The primary endpoint was met, with 38.2% of the tofacitinib group and 5.9% of the placebo group achieving the ACR50 response rate at month 3 (p <.0001). For secondary endpoints, ACR20/ACR70/PASI75 responses were higher with tofacitinib versus placebo. Enthesitis and dactylitis resolution rates and HAQ-DI reduction were greater with tofacitinib versus placebo.
The incidence of adverse events (AEs)/serious AEs through to month 3 were 68.4%/0% for tofacitinib and 75.0%/4.4% for placebo. One death was reported in the placebo group due to an accident. By month 6, one serious infection, non-serious herpes zoster, and lung cancer case each were reported in the tofacitinib group, and 4 serious infections and 1 non-serious herpes zoster case were reported the placebo group. There were no reports of non-melanoma skin cancer, major adverse cardiovascular or thromboembolism events.
The limitations of this study include the 6-month duration, which prevents conclusions on the long-term effectiveness and assessment of long-latency safety events of tofacitinib in Chinese patients with PsA.
References
- Leng X, Lin W, Liu S, et al. Efficacy and safety of tofacitinib in Chinese patients with active psoriatic arthritis: a phase 3, randomised, double-blind, placebo-controlled study. RMD Open. 2023;9(1):e002559. doi:10.1136/rmdopen-2022-002559