Extraintestinal Manifestations of Inflammatory Bowel Disease: A Step Toward Standardizing Assessment
Investigators from the Cleveland Clinic standardized diagnostic, follow-up, and treatment targets for 5 major EIMs: peripheral arthritis, axial arthritis, pyoderma gangrenosum, erythema nodosum, and uveitis.
Katie Falloon, MD

Though inflammatory bowel disease (IBD) is characterized by inflammation of the gastrointestinal tract, a significant proportion of patients with IBD suffer from a myriad of complications outside of the bowel.
These complications, called extra-intestinal manifestations, are found in as many as half of all patients with IBD and yet have received only limited research attention, particularly in the US.
This is problematic, as EIMs significantly impact patients’ quality of life, are associated with increased morbidity, and often require complex decision making and multi-specialty collaboration on the part of healthcare providers.
Due the heterogeneity in the literature and the lack of clear EIM definitions, we sought to standardize diagnostic, follow-up and treatment targets for 5 major EIMs (peripheral arthritis, axial arthritis, pyoderma gangrenosum, erythema nodosum, and uveitis).
To do this, we convened a modified Delphi consensus panel consisting of 12 gastroenterologists, 4 rheumatologists, 3 ophthalmologists, 6 dermatologists, and 4 patient representatives.
The modified Delphi consensus methodology is an evidence-based approach that incorporates both previously published evidence and clinical expertise in order to arrive at answers to research questions.
Following literature review, development of candidate items, lively debate, and 3 voting rounds, we arrived at consensus criteria for appropriate and, when possible, optimal means of diagnosing and monitoring the 5 EIMs in question.
The results provide guidance for the practicing clinician on items essential to management of EIMs, such as which provider should clinically diagnose each EIM and how frequently patients should be seen based on type and severity of EIM.
For example, uveitis can be vision threatening and requires ophthalmology involvement in diagnosis and monitoring with close follow-up, while erythema nodosum, which often self resolves, can be managed by either a gastroenterologist or a dermatologist and requires less intensive follow-up.
The results also standardize concepts that are essential to successfully conducting further research in this area, for example by outlining multi-specialty approved strategies to assess for improvement or worsening of each of the 5 EIMs, which is critical to determining if a given therapy is working effectively.
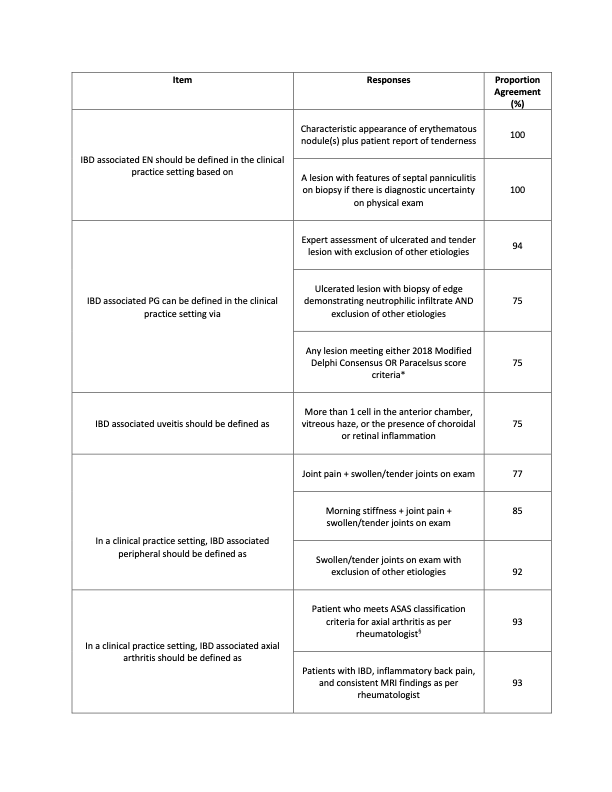
The results of our work were published in Alimentary Pharmacology and Therapeutics early this year and are summarized in the table provided (Table 1).
Table 1. Extraintestinal Manifestation Definitions
I am excited to continue to build upon this work and move forward with further exploration of EIMs in IBD. With funding support from the Crohn’s and Colitis Foundation, we have built a network of 11 centers across the country and are creating a prospective registry of patients with EIMs (entitled CHASE-EIM [Cohort for Healing Arthritis, Skin, and Eye Extra-Intestinal Manifestations]) utilizing the definitions we developed.
Initially we will focus solely on peripheral arthritis, which while the most common EIM is also arguably one of the least well-understood.
We are recruiting 100 patients across our network and following them for the course of 1 year. We will collect both objective measures of disease and EIM activity as well as patient reported outcomes via clinic visits and regular surveys.
In so doing, we hope to better understand the overall clinical presentation of peripheral arthritis, investigate response to various therapies (both for IBD and for peripheral arthritis specifically), and clarify risk factors for development, progression, and recurrence of peripheral arthritis.